Experts from the Weiss Center treat severe polyposis
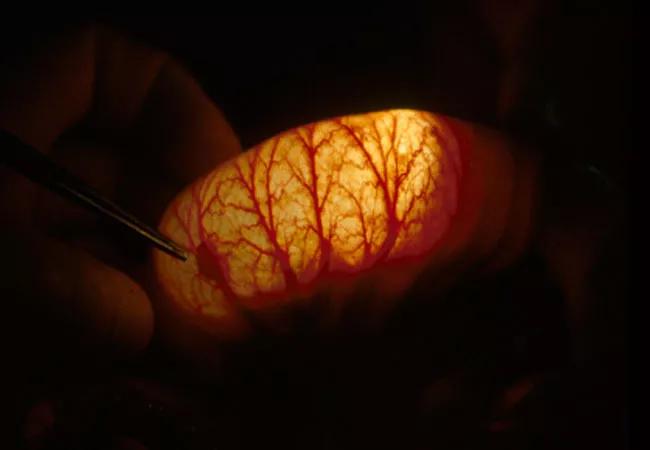
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/51963070-0462-462c-a2a0-e7b61d5b3a45/20-DDI-1973689-PJS-Case-Study-Hero_jpg)
20-DDI-1973689-PJS-Case-Study-Hero
A 27-year-old female occupational therapist from out of state presented to Cleveland Clinic with only 125 cm (about 25% of normal) of remaining small bowel after multiple surgeries and resections due to severe polyposis. She was at risk for short gut syndrome, which is associated with dehydration and malnutrition that may necessitate total parenteral nutrition. She had previously been diagnosed with and surgically treated for Peutz-Jeghers Syndrome (PJS), a hereditary colorectal cancer syndrome that causes hamartomatous polyps, an elevated lifetime cancer risk of 37 to 93% and mucocutaneous pigmentation.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“She came to us with few surgical options remaining,” said David Liska, MD, Director of the Sanford R. Weiss, MD, Center for Hereditary Colorectal Neoplasia at Cleveland Clinic’s Digestive Disease & Surgery Institute. “She was not followed by a registry and so did not have appropriate surveillance.”
Weiss Center caregivers performed an MR enterography that showed massive polyposis of the small bowel. Endoscopic removal was attempted, but adhesions from previous surgeries prevented necessary endoscopic access. Instead, Amit Bhatt, MD, and Dr. Liska performed a “clean sweep,” or intraoperative pan-enteroscopy, a procedure that removes polyps inaccessible on balloon enteroscopy.
“Although she had only 125 cm of small bowel left, we successfully removed 180 polyps through this combined approach, and allowed her to keep her small bowel,” notes Dr. Bhatt, an advanced endoscopy specialist with the Weiss Center. “That’s an extraordinary number, and would only be possible through this team approach. Fortunately none of them were cancerous polyps.”
The patient is doing well and is returning to the Weiss Center for another procedure. Her brother is now a patient as well.
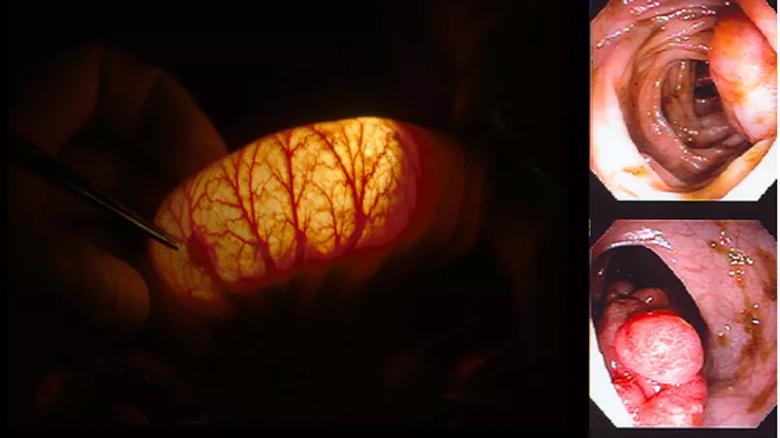
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/9d09e3f3-02eb-4570-9cea-f69c828528ea/20-DDI-1973689-PJS-Case-Study-Inset_jpg)
Patients with PJS are often diagnosed in middle childhood or the early teen years and present needing emergency surgery for small bowel obstruction due to polyposis-related intussusception and resulting in bowel ischemia or necrosis. “These patients often require several surgeries over the years,” notes Dr. Liska. “At the Weiss Center, we have a registry that allows us to follow patients very closely to avoid emergency procedures and instead use prophylactic measures to prevent bowel obstructions and cancer.”
Advertisement
Since patients with PJS are also predisposed to several types of cancer, the Weiss Center coordinates screening and surveillance so that cancers can be diagnosed and treated early. The multidisciplinary center’s mission is to prevent death or complications from cancer and to maintain quality of life for patients with hereditary colorectal conditions. Other syndromes of hereditary colorectal neoplasia include familial adenomatous polyposis, PTEN hamartoma tumor syndrome, juvenile polyposis syndrome and Lynch syndrome.
Patients with PJS are at increased risk for intestinal cancer and at high risk for bowel obstructions. The Weiss Center team monitors patients for polyps via enterography and capsule endoscopy with the hope that polyps can be removed endoscopically before they get big enough to cause obstruction or to develop into cancers.
“Sometimes, as in our patient from out of state, they simply cannot be totally removed endoscopically for various reasons,” says Dr. Bhatt. “Then, we use an advanced, team-based method in the OR that allows us to view the entire intestine from mouth to anus using manually guided intraoperative endoscopy to remove polyps and prevent obstructions or cancer.”
James Church, MD, the Weiss Center’s first director, nicknamed this procedure the “clean sweep.” A recent study of 50 Cleveland Clinic patients demonstrated that this procedure decreases the need for emergency laparotomies for small bowel obstruction due to polyp-related intussusception in patients with PJS. Further studies are planned to confirm these results.
Advertisement
These studies all draw from a ground-breaking concept. In 1979, Dr. David G. Jagelman established Cleveland Clinic’s Familial Polyposis Registry. His intent was to follow high-risk colorectal patients and families with a personal and/or family history of familial adenomatous polyposis and other similar syndromes. In 1989, hereditary nonpolyposis colorectal cancer was added to the registry.
“Now the registry includes thousands of patients and their families and has allowed us to learn more about the best ways to track and treat these disorders,” says Dr. Liska. For instance, the registry’s presence promotes proactive screening for Lynch syndrome. The Digestive Disease & Surgery Institute, Genomic Medicine Institute, Pathology and Laboratory Medicine Institute and Women’s Health Institute collaborate through the Weiss Center to provide comprehensive and coordinated risk-based screening, surveillance and treatment for patients with Lynch syndrome.
Because these hereditary syndromes are so rare, the Weiss Center receives referrals from all over the world. “We are a one-stop shop for patients. Patients from out of town can get all of their visits in a single day, and we employ three full-time coordinators to ensure the referral process is as easy as possible for physicians and patients.”
Feature image: “Clean Sweep” procedure. Left image show intraoperative enteroscopy transilluminating the small bowel with the silhouette of a polyp outlined. Right images show endoscopic appearance of PJS polyps.
Advertisement
Advertisement
Pivotal Studies Guide Treatment Decisions in Muscle-Invasive Bladder Cancer
Reflections from an oncology provider and communications educator on new ASCO Guidelines on Patient-Clinician Communication
Phase 1 trial outcomes offer encouraging news for developing targeted therapy for solid tumors
Cleveland Clinic to administer first-of-its-kind T-cell therapy
Heavily pretreated patients experience improved progression-free survival and quality of life with CD20xCD3 therapy
Innovative procedure reduces scarring, recovery time and nipple sensation
Best practices for supporting patients with honesty and compassion
Goal-of-care discussions drive earlier hospice access