Advancing Cleveland Clinic’s clinical systems integration by creating a secure, single database designed and built to modern healthcare standards

We’re in the midst of a data explosion. And the healthcare industry takes the lead by generating up to 30% of the world’s data volume. That’s faster than the manufacturing, financial services, media and entertainment industries.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“While there’s enormous potential with all this data, its usefulness depends on sound, secure applications and programming,” says Brent Hicks, Cleveland Clinic’s enterprise architect.
Hicks’ expertise covers the oversight, direction and collaboration among internal stakeholders, vendors and application development teams to ensure reliable, efficient processes.
“The tech industry is constantly evolving and with that comes more and more options.” Hicks continues, “With more choices, there’s also a sharp jump in requests from our caregivers.”
Hicks considers all the different applications and solutions to ensure they work as designed and that there’s a solid operational plan.
He adds, “Any new technology needs to integrate seamlessly with our existing applications without duplicating our current tools.”
Digital tools strengthen patient care by creating connected experiences and optimizing operational efficiencies.
Hicks explains, “Working with clinical teams gives us the bandwidth to succinctly knit together our technical capabilities to broaden our reach. Pulling data from our electronic health records generates real-time clinical support. Alerts, care management guidelines, reminders — these come from computer-based logic linked to best practices.”
He shares this example: “Organ procurement is complex and time-sensitive. There are several moving parts typically done by phone and on paper. We’ve automated the process by adding an algorithm within Epic that applies designated criteria to patient records to determine organ availability and necessity.”
Advertisement
Most healthcare organizations’ electronic health record systems are vendor-based, which entails proprietary restrictions and limitations. This one-way integration limits access and functionality. Transitioning to an advanced, bi-directional integration system expands access to better use of data and predictive modeling.
This transition is happening with Hicks’ input. He supports Cleveland Clinic’s clinical systems integration process by creating a secure, single database designed and built to modern healthcare standards. This approach provides seamless vendor integrations, synced data and rapid application development with immediate access.
Part of this optimization started with the onset of the Fast Healthcare Interoperability Resources (FHIR), which defines healthcare data standards. The Health Level Seven (HL7) standards operationalize FHIR by defining guidance standards for transferring and sharing data among providers.
“FHIR defines how healthcare information can be exchanged between different computer systems regardless of how it is stored in those systems,” says Hicks. “This ensures easier, cohesive integration across platforms to enhance care delivery.”
Hicks continues, “Since limitless applications can access this single source of truth, it removes the need to make more and more data copies (as done in the past), which vastly speeds up project development.”
Beyond clinical decision-making, predictive modeling also addresses staffing and logistics.
“One example is looking for data patterns to predict patient cancelations.” Hicks explains, “These details give our caregivers the foresight to offer services to help patients come in for their appointment. If the patient has a transportation issue, they can schedule an Uber ride. Caring for our patients is more than an office visit and we can use data to help eliminate obstacles”
Advertisement
Similarly, nurse managers have access to digital tools for staffing support.
“They can use administrative data, such as timekeeping, and patient volume to anticipate care gaps and shift nursing coverage,” says Hicks.
Patients’ needs and experiences are evolving with emerging technologies, so being patient-centric is essential.
“Streamlining data to create ‘frictionless’ experiences is top of mind for us and our patients.” Hicks adds, “Friction in healthcare describes obstacles that delay access to care. When applied to technology, think of trying to schedule an online appointment and then having to call for the appointment. That’s friction — and that’s frustrating.”
He continues, “We’re working smarter by pushing and pulling data from our integrated systems to produce the desired outcome. This eliminates the need to check multiple systems, limits phone calls and gives patients what they want.”
Despite technology’s endless potential, data validation remains critical prior to launching digital tools.
“The application build may be technically perfect, but if it fails operationally, it’s absolutely useless,” says Hicks. “The validation piece confirms the testing component and ensures the best outcome for our patients and caregivers. That’s when it’s clear your work is meaningful.”
Advertisement
Advertisement

Digital “tripwires” detect and respond to malicious activity, boosting cybersecurity maturity

Thoughtful collaboration, data-driven decisions and effective change management lead to significant savings

Clinical input is integral to technology implementation and adoption strategy

Unit-based project decreases non-urgent alarms

Integrating technology is more than product delivery
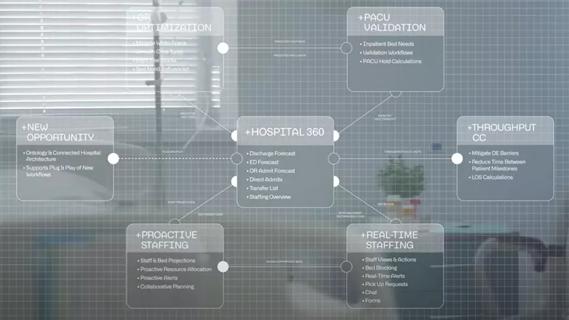
Cleveland Clinic partners with Palantir to create logistical command center

Cleveland Clinic’s roadmap to recovering critical digital assets stems from strategic planning and preparedness

The Friends of Cybersecurity program bridges innovative technology solutions with mitigating security risks