A unique approach provides long-lasting results with minimal impact on the disease state
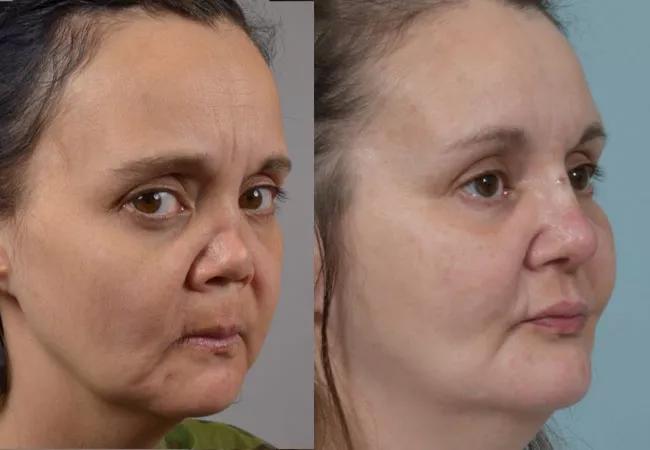
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/461d2da7-cc39-4e28-be90-f43583e61452/21-HNI-2202208-Nasal-recon-autoimmune-disease1-Fritz-Ciolek-CQD_650x450-1_jpg)
Before and after GPA patient
Written by Michael Fritz, MD
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Granulomatosis with polyangiitis (GPA), formerly called Wegener’s Granulomatosis, is an autoimmune vasculitis that can affect the lungs, kidneys, airway and sinonasal regions. It can lead to severe complications that compromise the nasal structure and lead to deformities. Despite the rarity of this disease, the plastic and reconstructive surgeons in Cleveland Clinic’s Head & Neck Institute have extensive experience correcting these nasal deformities. With an osteocartilaginous L-strut technique, we provide long lasting and aesthetically favorable results to patients with GPA, and we’re able to help them return to normal life in a lasting way.
Because GPA is a remarkably uncommon disease which can affect multiple body sites and organ systems, it can be challenging to diagnose. Patients often present in different ways with possible disease symptoms related to kidneys, lungs, trachea (stenosis), nose and sinuses. In particular, anybody who has a septal perforation without a history of trauma or complications from previous surgery should always be tested for GPA.
Patients who suffer from this disease often develop complete loss of all nasal structural support and dramatic scarring of the external and internal nose, including near total septal perforations. The nose is chronically crusted and infected, making it difficult to breathe through. Nasal deformity due to GPA or related autoimmune vasculitis (e.g., sarcoidosis or relapsing polychondritis) pose significant challenges to the reconstructive surgeon.
Advertisement
First, profound collapse and scarring typically require extensive modification of tissue and framework replacement. Second, despite dramatic changes and contraction of the nasal lining, surgeons are required to use a technique that completely avoids entering the nose (i.e., only under the skin) to avoid worsening of the disease itself. Lastly, patients are typically on immunosuppressant medications, which can impair wound healing.
In order to treat this disease, our Head & Neck Institute collaborates very closely with our rheumatologists in Cleveland Clinic’s Orthopaedic and Rheumatology Institute. Because we can only perform the surgery when GPA has gone into remission, we need approval from our rheumatologists that the disease is under optimal control. The rheumatologists at Cleveland Clinic are world-class, and they are very meticulous about preventing disease flare ups in our patients. Someone with GPA may be in remission, but that means that they’re very often still getting quarterly immunosuppressive shots, they’re still on some element of steroids, and we need to be cognizant of these factors when it comes time for surgery.
Because we never enter the nasal cavity, our technique ensures that we do not cause any disease flare ups. We never disturb tissue that has been profoundly affected by the vasculitis. It’s critical that we don’t enter the nose and create significant inflammation, tissue turnover and potentially infection because that could flare the disease process. Our reconstruction is entirely underneath the skin, and as a result, there is minimal risk of affecting the disease itself.
Advertisement
The reconstructive technique we employ involves a combination of rib bone and cartilage articulated into an L-strut which provides robust support for the nasal bridge and tip. The key factor in a successful reconstruction is to create a strong construct which restores normal nasal appearance and airway support and also resists tissue tension and scarring to prevent postoperative collapse or deviation of the nose.
This osseocartilaginous L-strut is placed in a precise pocket created through incisions at the end of the nostrils and continued over the nasal bridge – extensive scar release is performed so that the skin can drape over the structure. In addition, the rib bone is sculpted in a fashion that allows it to precisely fit upon and integrate with the patient’s own nasal bones, forming a very strong, fused construct that supports the nasal tip and bridge. An advantage of the cartilage component of the reconstruction at the nasal base is that the patient’s own tip cartilages can be secured easily to this construct to achieve the most natural angles and shape. Often, patients’ appearance is returned to normal after just one operation, but given the magnitude of the initial deformity, a second stage with modification of the nasal tip or additional cartilage grafting (typically from behind the ear) may be required to achieve an optimal result.
Another advantage of this surgery is the relatively simple post-operative recovery. When the rib is removed, we use a long-term numbing agent that lasts 72 hours: this ensures that by the time the patient notices the pain, the window where they would be impacted the most has passed. Patients can go back to normal activities after a couple of weeks. Recovery for the osseocartilaginous L-strut is similar to a normal rhinoplasty, and patients are either released the day of the surgery or the following morning. The L-strut takes a few months to fully stabilize and about a year to completely heal. At three months after surgery, patients return to the office for a simple in office procedure to remove a pin that stabilizes the rib to the nasal bones and allows them to fuse together.
Advertisement
Patients who have suffered from this disease but have managed to overcome it through aggressive immunotherapy, unfortunately, often have profound nasal deformity which persists afterwards. These individuals have such obvious stigmata of their disease that they continue to suffer its effects from a social and functional standpoint even after remission. This reconstructive effort allows them to return to normal life without deformity.
Advertisement
Advertisement
Systematic review indicates more can be done for higher-risk patients
Analysis of HNSCC patients shows HPV status to be predictive of higher abundance of oncobacteria within the tumor
Case study illustrates the potential of a dual-subspecialist approach
Evidence-based recommendations for balancing cancer control with quality of life
Study shows no negative impact for individuals with better contralateral ear performance
HNS device offers new solution for those struggling with CPAP
Patient with cerebral palsy undergoes life-saving tumor resection
Specialists are increasingly relying on otolaryngologists for evaluation and treatment of the complex condition