Goals include reduced morbidity, shorter hospital stays
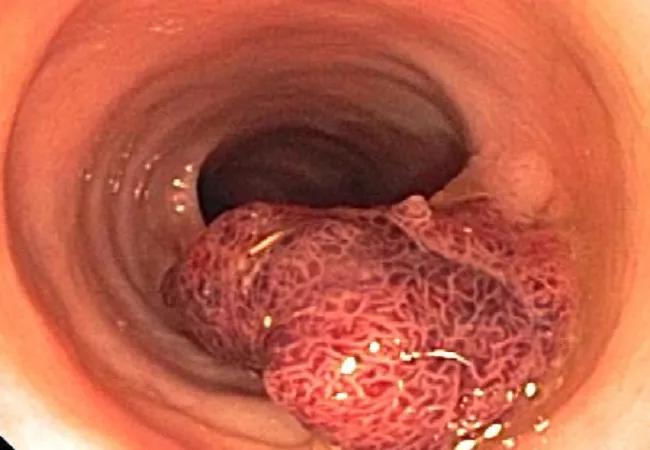
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/72d71d8c-8506-447d-ae11-05bb18a4fa62/Polyp-image-Copy_png)
Polyp image – Copy
Precancerous, cancerous and complex polypoid lesions have traditionally required surgical resection.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Recent advances in technology and endoscopic techniques have essentially enabled the ability to operate through an endoscope, birthing a new field of endoluminal surgery that permits the removal of these lesions through an endoscope — allowing patients to avoid surgery, keep their native organs and have an improved quality of life.
Endoluminal surgery involves procedures such as endoscopic submucosal dissection, complex endoscopic mucosal resection, endoscopic full-thickness resection, and submucosal tunneling endoscopic resection.
Cleveland Clinic’s new Endoluminal Surgery Center was created to:
The center’s directors, colorectal surgeon I. Emre Gorgun, MD, and advanced endoscopist Amit Bhatt, MD, joined forces to create the center within Cleveland Clinic’s Digestive Disease & Surgery Institute. Dr. Gorgun focuses on lesions in the lower tract (i.e., colon), while Dr. Bhatt focuses on lesions of the upper tract (i.e., esophagus, stomach, small bowel). Both bring extensive experience and expertise in endoluminal surgery to the table, and say their collaboration will only make these programs stronger.
Cleveland Clinic physicians adapted the endoluminal resection technique that was initially developed by clinicians in Japan. “When we brought it over to the U.S., it was something new, and now it’s grown,” Dr. Bhatt says. “We’ve been doing this at Cleveland Clinic for six years, with excellent patient outcomes. Now, more and more patients are coming in seeking advanced endoluminal resection.”
Advertisement
“A large number of patients require this kind of care,” Dr. Gorgun says. “Annually, there are more than 30,000 colon and rectal resections for non-cancerous colonic lesions and benign polyps nationwide. Surgical removal of the colon for benign reasons is associated with higher risks, morbidity, longer hospital stays — plus increased costs. Advanced endoluminal approaches can be superior from that perspective.
“Hence the need for a center — that’s why we created it,” Dr. Gorgun says.
“We collectively come together and discuss each case, similar to what we do with cancers at our multidisciplinary tumor board, but this is more like a complex polyp board,” Dr. Gorgun says. “In more challenging cases, we rely on our colleagues from other departments and may need to obtain further imaging, like a polyp MRI or rectal MRI from radiology, endorectal ultrasound, or a review of the pathology. It’s an entire multidisciplinary approach, making decision-making more reliable.”
Dr. Bhatt agrees that complete resection of a lesion is a distinct advantage. “Through advancements in endoscopy, we are now able to dissect these tumors out in one piece … which allows us to confirm that we removed all of the tumor and there are no high-risk features within it,” he says. The benefit for patients, he says, is “this allows us to potentially get rid of a tumor or cancer with minimal morbidity. It allows patients to keep their native organ — their esophagus, stomach, colon or rectum — so they can maintain their quality of life.”
Advertisement
The center’s patient-focused goals include aiming for less morbidity and shorter hospital lengths of stay.
Traditionally, diseases of the upper tract such as esophageal or gastric cancer have been treated with surgery. For elderly patients, who are prone to develop these tumors, surgery can be “quite a big deal, or they may not even be candidates for surgery due to co-morbid illnesses,” Dr. Bhatt says. For example, esophagectomy is associated with significant morbidity and mortality.
In addition to streamlining and improving patient experience, Dr. Bhatt says the center will have the infrastructure to enhance long-term post-treatment surveillance, when needed. “We’re not a ‘one-and-done’ shop,” he says.
“We want to make sure our patients with complex polyps remain healthy long-term,” Dr. Bhatt says. “The center will allow us to not only push the envelope on procedures, but to take better care of our patients.”
Working with industry on new device development, leveraging experience from Cleveland Clinic’s large patient volume, and conducting ongoing research in endoluminal techniques and optimal patient outcomes are among the center’s additional goals.
“We recently completed a multicenter study showing the benefits of endoscopic submucosal dissection compared traditional endoscopic mucosal cancer for esophageal adenocarcinoma,” Dr. Bhatt says.
Dr. Gorgun emphasized the importance of ongoing research, which will allow the center’s clinicians to continuously improve patient care. “We are collecting our experience through a patient registry database, which will enable us to continue to do more ground-breaking research that will, most importantly, translate into better patient outcomes,” he says. “Our goal is to be a cutting-edge, world-leading center.”
Advertisement
Advertisement
Reframing cancer survivorship
New guidelines empower clinicians with practical diagnostic framework
Pivotal Studies Guide Treatment Decisions in Muscle-Invasive Bladder Cancer
Reflections from an oncology provider and communications educator on new ASCO Guidelines on Patient-Clinician Communication
Phase 1 trial outcomes offer encouraging news for developing targeted therapy for solid tumors
Cleveland Clinic to administer first-of-its-kind T-cell therapy
Heavily pretreated patients experience improved progression-free survival and quality of life with CD20xCD3 therapy
Innovative procedure reduces scarring, recovery time and nipple sensation