By working in tandem, a pediatric otolaryngologist and speech-language pathologist can diagnose conditions and develop treatment plans in the same visit
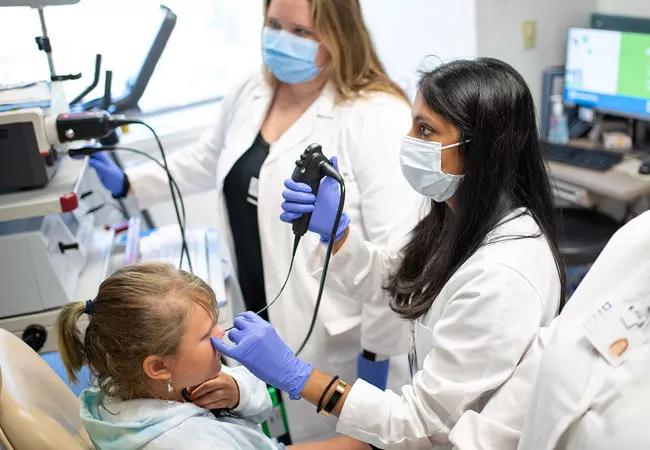
A new service at the Cleveland Clinic aims to provide state-of-the-art multidisciplinary specialist services for pediatric patients with voice disorders.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Funded by a special Head & Neck Institute Catalyst Grant, and co-led by pediatric otolaryngologist Swathi Appachi, MD, and speech-language pathologist Emma Laurash, MS, CCC-SLP, the new center will also collect data on treatment outcomes to help advance the field. The grant will primarily be used to help expand the program.
“The idea is to have a multidisciplinary place where children with voice disorders could be evaluated by an otolaryngologist and a speech pathologist during the same visit, so we can both diagnose the condition and develop a treatment plan for voice disorders at one time,” Dr. Appachi says.
And, Laurash adds, “When the family knows that the entire care team is on the same page with the plan, it tends to help increase family motivation to comply with recommendations.”
Voice disorders can affect up to 15% to 20% of children. One of the most common is hoarseness due to vocal cord nodules or swelling, also known as phonotraumatic lesions. These are especially common in younger children who tend to vocalize often, and can be exacerbated by illnesses, post-nasal drip or reflux. Although they’re benign and tend to disappear as the child ages, the hoarseness can lead to problems.
“The child might not want to talk because they’re self-conscious about their voice and that can hold them back socially or in school,” explains Dr. Appachi. “The literature shows that a hoarse voice or one that doesn’t sound normal can impact the way the child is viewed by teachers and peers in school. There’s definitely a quality-of-life aspect to it.”
Advertisement
Some children may benefit from voice therapy, especially those children with vocal fold nodules. However, some may need surgery to address their voice concerns. For example, a polyp or cyst may need to be surgically removed as these don’t tend to respond as well to initial voice therapy as do nodules. Vocal cord paralysis may also require surgery to address this problem. Recurrent respiratory papillomatosis is another example where surgery is indicated. Many children may also need voice therapy following surgery.
To evaluate children with voice conditions, the larynx is examined with videostroboscopy, a device that goes through the nose to circumvent the gag reflex, allowing visualization of the larynx and surrounding structures.
“This tool is one of the major benefits of a child coming to see us in pediatric voice clinic versus just a visit with [ear, nose, and throat] alone,” explains Laurash. “Stroboscopy is the gold standard evaluation procedure for any patient with a voice disorder. It allows us to better evaluate the movement, pliability, closure and tissue changes of the vocal folds during phonation. These parameters help us understand why the voice sounds the way it does and help us determine what we will target in voice therapy.” Most children tolerate the stroboscopy procedure well, she adds.
The team also administers a pediatric “voice handicap index (VHI)” questionnaire that measures the patient’s perception of the emotional, functional and physical implications of a voice disorder on their daily life. “We give this to patients at each visit and compare it against previous visits to see how their perception of the issues has changed. The hope is that we see a decrease in pediatric VHI scores over the course of treatment,” Laurash explains.
Advertisement
Laurash says that voice samples are also audio recorded at each visit. “We can then analyze this to get acoustic data that directly reflects characteristics of the voice that we would like to see improve over the course of treatment. This gives us a more objective measure than just our own perceptual assessment and the patient’s perception of the issue.”
Moreover, Laurash notes, “Data can be used as a great way to show patients their progress during treatment. It can be difficult for patients to remember where they were prior to therapy, so allowing the family to hear old recordings or compare how they rated the voice six months prior can be a great tool.”
Thus far the voice clinic has been offered about once a month, to about four patients at a time. “We’re hoping that as we get more equipment and referrals, it will grow it will be a twice-a-month offering. We’re going to open up more slots in anticipation of this,” Dr. Appachi says.
It’s located physically in the same building where an adult voice center has been operating for several years. Although the team has brought in pediatric scopes, it hopes to obtain several more in order to see more patients.
There’s also a research component to the clinic, with approval from the Institutional Review Board and Pediatric Research Review Committee already in place. In one study, voice samples are being analyzed with software that can objectively assess voice quality to monitor improvement. “Everything we’re doing is evidence-based, but a lot of the literature is retrospective so we’re hoping to collect data prospectively,” Dr. Appachi notes.
Advertisement
“I think this is an exciting opportunity to serve an unmet need,” she says. We hope to start drawing more referrals from the region so we can help more pediatric patients meet their complete potential.”
Advertisement
Advertisement

A wide-ranging discussion on the latest in laryngology

A multidisciplinary approach and individualized plan of care are imperative
Newly published research shows how the surgical technique is a game-changer for patients with ORN

Analysis of HNSCC patients shows HPV status to be predictive of higher abundance of oncobacteria within the tumor

Case study illustrates the potential of a dual-subspecialist approach

Evidence-based recommendations for balancing cancer control with quality of life

Study shows no negative impact for individuals with better contralateral ear performance

HNS device offers new solution for those struggling with CPAP