Recognizing mobility as a human right is instrumental to change
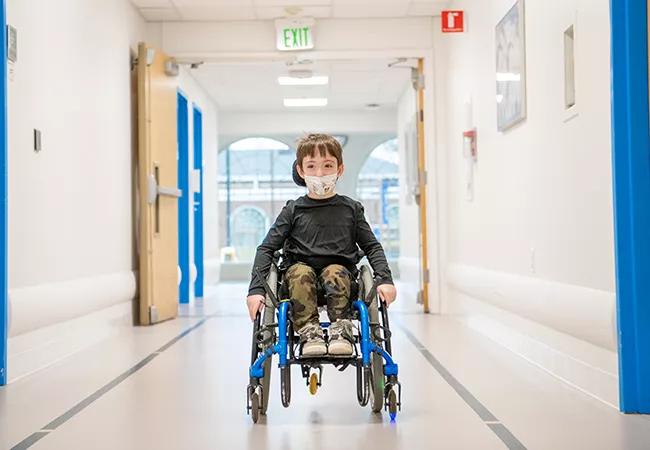
Traditionally, mobility is defined as the ability to get from one place to another, “but it’s so much more than that,” says Andrina Sabet, PT, ATP. “It’s how we make our own choices, show people what we like, disengage from what we don’t like. You can substitute the transportation, but you can’t substitute all the agency and the identity that goes around mobility.”
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
As a pediatric physical therapist at Cleveland Clinic Children’s Hospital for Rehabilitation, many of the children Sabet works with have significant mobility issues. “There are so many barriers to alternative mobility, and much of this is related to the culture around mobility,” she says. “Most cultures see walking as the gold standard, and that has greatly impacted research, medical practice, the design of technologies and the access to these technologies for young children.”
Despite the fact that mobility is integral to every child’s development, Sabet says in many areas, kids with disabilities often don’t have access to alternative means of mobility. This deficit inspired Sabet and her colleagues to publish a paper in Pediatric Physical Therapy that delves into a deeper look at mobility in its current context and the necessity of treating it as a human right.
The paper also proposes a new framework to aid clinicians in supporting children of all abilities in their right to mobility. “It defines mobility more broadly, going beyond that definition of translocation and looking at the agency that is around mobility,” says Sabet. “It’s not just a motor skill; it’s tied to autonomy and the emergence of identity.”
The framework, called ON Time Mobility, “challenges the notion that walking is the gold standard,” Sabet says. “If we can shift that paradigm to mobility as the gold standard, in whatever form that may happen, that should be the criteria we strive for.”
With the twin goals of encouraging discussion and examining clinical practice, research and approaches to mobility, the authors narrowed the ON Time Mobility framework down to five interrelated principles.
Advertisement
Timing: Mobility begins in the first year of life, but when children have disabilities, their motor skills are often delayed. This principle aims “to shift our perception of when we intervene so that all kids get to experience mobility at the same time, regardless of their motor capacity,” says Sabet. “When we go back to that human rights aspect, can we match the timing to when typically developing kids would have mobility with the children that are not having the same motor trajectory?”
Urgency: If mobility is a human right, Sabet says it deserves to be elevated to the same priority as other human rights, such as water, food, safety and education. “So many of our kids are transported passively for long periods or large portions of their day,” Sabet says. “We need to have a more urgent approach to having active mobility as opposed to passive.”
Multimodal: This principle encourages embracing a wide variety of mobility options for kids with mobility issues. “When it comes to a child with disabilities, people tend to support just one way for that child to move,” Sabet says. “Kids with typical development have a lot of variety and opportunity to select the way they move based on what best meets their needs for what they’re doing. We want our kids with disabilities to have that same opportunity.”
Frequency: The article notes that typical young children move constantly in their real-world environments, citing the 14,000 steps, 100 falls and distances equivalent to 46 football fields that toddlers collect over only six hours. “We tend to lose sight of how frequently kids move,” says Sabet. “Often kids with mobility issues will get an hour of therapy a week or a half hour in school when they’re in a mobility device and that’s their movement time. When you look at what their peers get, there’s such a discrepancy in terms of frequency. We have a really high bar to match what their typical peers are able to experience.”
Advertisement
Sociability: The interactions and communication between parent and child change dramatically as the child learns to move and gains independence. “That social relationship is tied very closely with the emergence of mobility in typical development, and if you take that a step further, when those kids get to a peer setting, movement is such a huge part of that,” says Sabet. “If you can’t keep up with your peers, you’re left behind and then your socialization is with adults.”
This principle states that social mobility should be a developmental requirement for young kids in all their environments. Appropriate interventions, technologies and policies need to be created to enable children with disabilities to engage in a wide range of social interactions throughout their lives.
There’s a lack of recognition as to how mobility alters development, which is a disservice to children with disabilities. “The ‘let’s-wait-and-see’ attitude changes kids and the people that care for them,” says Sabet. Children learn to depend on others instead of becoming autonomous, and their caregivers learn to provide for them instead of encouraging them to be independent. “That’s very repetitive, ingrained behavior and it really impacts the whole trajectory of development,” Sabet says.
“It’s easy for us, even those who work with children, to forget — or at least not prioritize — early mobility, but it’s very important to try to facilitate mobility for our patients to assist in development of all sorts of skills,” says Lainie Holman, MD, Chair of Pediatric Medicine and Rehabilitation at Cleveland Clinic Children’s Hospital for Rehabilitation. “There are many ways to assist everyone’s independence and exploration of their environment. Because children are smaller and more ‘portable,’ it is sometimes overlooked.”
Advertisement
Sabet hopes the ON Time Mobility framework will challenge clinicians to examine their internal biases around mobility, as well as how they define mobility for themselves and thus for their patients. She wants clinicians to view mobility as a human right, something she was never taught.
Secondly, Sabet invites clinicians to think about how to align their practices to support the right to mobility. “I think when we get in a clinical environment where we’re surrounded by all the priorities of clinical care, even our strong beliefs can shift lower on the priority list and maybe fall off altogether,” she says.
Another goal is to find better ways to support families of children with mobility issues. “When you have a child with significant delays or no mobility, there’s a lot of emotion tied up in that because mobility is so inherent to our culture,” says Sabet. “We need to support children to have mobility, no matter what the form is.” Rather than focusing on traditional motor milestones, “we can help families see from very early on that mobility is the key so that their child can form relationships and discover their identity,” she says.
Because mobility is a human right, “we can’t wait,” says Sabet. “It can’t be something that we just think about or talk about. We really need to have a call to action to make some changes in this arena.”
Advertisement
Advertisement

Staged pivotal noninferiority study is comparing BrioVAD with HeartMate 3

New developments offer providers more sophisticated options

Study explores center volume and outcomes using the STS-Pedimacs database

Cleveland Clinic series supports its feasibility, especially with HeartMate 3

Guidance on the often-fatal condition through an interventional cardiology lens
An innovative approach to protecting patients during breast and lung radiation therapy

Using alternative modalities to help patients with post-surgical pain

One pediatric urologist’s quest to improve the status quo