An expanding field driven by compassion and innovation
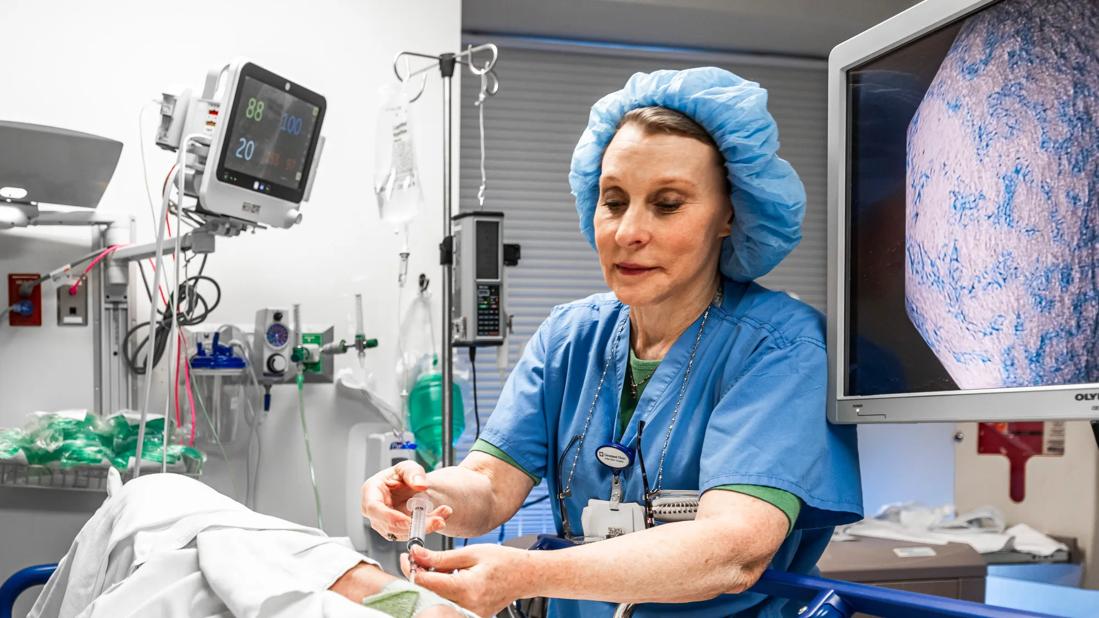
When asked about the footprint of gastroenterology nursing at Cleveland Clinic, Director of Nursing Debbie Brosovich, MA, RN, NE-BC, CCRN-K, admitted that before stepping into her current position even she was unaware of how large it really was.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“There are many different spheres of gastroenterology nursing within Cleveland Clinic and our team works across the entire health system – North, South, East and West,” says Brosovich, who has served in the director role for 3 years. “Additionally, we are an incredibly experienced team that includes APRNs, RNs, LPNs, PCNAs, scope technicians, secretaries, and more. The gastroenterology nursing specialty offers countless career opportunities.”
According to Brosovich, Cleveland Clinic’s main campus has four hospital floors dedicated to the Digestive Disease and Surgery Institute, including six inpatient gastroenterology units and several procedural areas. There are numerous gastroenterology-focused outpatient clinics and surgical centers, including three free-standing endoscopy centers and many physician offices in varying family health center and regional hospital locations.
Cleveland Clinic’s gastroenterology services cover the spectrum of patient care – from preventive screenings like colonoscopies to the most complex gastrointestinal (GI) diseases and conditions, such as cancer. And the care provided is top notch. In fact, Cleveland Clinic was recently named a 2019-2020 best gastroenterology and GI surgery program in Ohio by U.S. News and World Report.
Cleveland Clinic’s gastroenterology nurses typically work in one of three settings:
Advertisement
To be a nurse in the gastroenterology field, Irene Kato, BSN, CMSRN, says compassion is key. Kato is a registered nurse on Cleveland Clinic main campus’ inpatient colorectal surgery units. This year marks her 35th year as a nursing caregiver on the units.
“Since I became a nurse, I’ve had a passion for this patient population. This is where I started out and this is where I’ll always be,” Kato says. “Nurses in this specialty have to be genuine and caring. You have to understand that patients are often going through a chronic illness or cancer, but also a major body change. They may have to live the rest of their lives with an ostomy or a TPN (total parenteral nutrition). It can be devastating for patients and you have to assure them that it will be okay through kindness, compassion and encouragement.”
Gina Costanzo, BSN, RN, who has worked in the main campus inpatient endoscopy procedure area for the past 4 years, agrees. On her unit, which is a closed unit, Costanzo and her colleagues see as many as 60 to 80 patient cases per day throughout six procedure rooms – four of which are designed for full anesthesia procedures and two for conscious sedation procedures.
Costanzo says the reason she became a nurse is because she has Crohn’s disease and knew that if she worked in the gastroenterology field, she could help her patients on many levels.
“I’ve had the surgeries and the procedures, and I can personally relate to what my patients are going through,” Costanzo says. “I love caring for this patient population and I approach every situation the same way I would want my nurse to care for me or a member of my family. When a patient finds out that I truly know what they’re going through, they seem to let their guard down and become more relaxed. If I have to share my story to make a patient feel more comfortable and at ease, it’s worth it!”
Advertisement
LaTora Bristow, RN, shares the sentiments of Kato and Costanzo. With 12 years of experience in gastroenterology nursing, Bristow works as a colorectal surgery clinic nurse in the ambulatory facility at main campus.
“To work in this specialty takes patience and understanding – being loving and kind toward your patients while encouraging them is very important,” she says.
One of Bristow’s primary responsibilities is to support and guide her patients through procedures or exams. She says she often offers words of encouragement, tells them to take slow deep breaths, holds their hand, or gives them tissues when needed.
“You have to show a lot of compassion. Patients are generally nervous and scared because what they are having done is uncomfortable. They need a lot of support to help make them feel as comfortable as possible,” Bristow adds.
With ongoing practice advancements and innovations, new technologies and more, the gastroenterology nursing specialty is expanding – especially at Cleveland Clinic.
“From young to old, our patients often have very complicated histories that most other hospitals won’t take on,” Kato says. “We are very advanced in the GI field at Cleveland Clinic. For example, we have an entire group of stoma nurses who specifically see patients with ostomies and more than 20 wound, ostomy and continence (WOC) nurses throughout our hospital. We also have the Wound, Ostomy and Continence Nursing Education Program, which was established 60 years ago as the first WOC school in the world.”
Advertisement
Brosovich says Cleveland Clinic’s nursing caregivers greatly influence gastroenterology practice. If a tube holder is irritating a patient’s skin, for instance, she says nurses will research alternate options. Or, if a team member thinks there might be a better way of doing something, they will explore new possibilities, enlist the help of the Office of Nursing Research and Innovation, and more.
“Cleveland Clinic is at the forefront of changing the future of digestive disease care,” says Brosovich. “We do some really incredible things here, like what we call a ‘medical home,’ where the needs of chronic disease patients are closely followed at home so we can address potential issues before they happen. This care model includes social workers, psychologists, medical providers, nurses and other caregivers and follows the patient over the course of their disease.”
Costanzo says in the advanced endoscopy procedure area, she and her colleagues often introduce new innovations that reduce the need for surgery and prolonged anesthesia. Just last December, she assisted a physician partner with an endoscopic procedure that had never before been documented as being successfully done in the U.S. The team embolized an actively bleeding aneurysm through an ultrasound for a patient who was in the intensive care unit.
“Being an advanced endoscopy nurse at Cleveland Clinic means there will be a lot of ‘firsts’ and that’s really exciting,” Costanzo says. “We are placing stents, we are draining cysts, we are helping prevent patients from going to the operating room, we are removing cancer through an endoscope, and so much more. We do something new here every day.”
Advertisement
Kato agrees that there is a lot of opportunity for innovation in GI nursing at Cleveland Clinic. In fact, in 1996, she played a prominent role in the creation of a private procedural room for colorectal patients that is still used today. Kato says the room offers added privacy during physician exams or minor scope procedures and is very unique because it is located on the inpatient nursing unit.
Additionally, in 2016, Kato was actively involved in the development of a group class for patients with ostomies and, to date, has had more than 2,000 patients and family members in attendance. The hour-long class, which Kato leads, is offered two times per week in the inpatient setting and is designed to help patients better understand all that goes along with an ostomy. The class content follows a multi-disciplinary approach and includes key information about nutrition, hydration, medications, what to look for at home, and more.
However, just as important, Kato says the class offers patients the opportunity to engage with other patients who are experiencing the same thing and is a highly successful form of group support and therapy.
For those considering a career in gastroenterology nursing, there is much opportunity – from the varying patient populations to the wide variety of nursing care paths the specialty offers.
In celebration of the Society of Gastroenterology Nurses and Associates’ 7th annual GI Nurses and Associates Week (March 22-28), Cleveland Clinic proudly recognizes the hard work and dedication of gastroenterology nursing caregivers. Happy Year of the Nurse!
Advertisement

Planning continues with critical, patient-focused input from nursing teams

Strengthening care through targeted resources and frontline voices

Embracing generational differences to create strong nursing teams

CRNA careers offer challenge and reward

An unexpected health scare provides a potent reminder of what patients need most from their caregivers

Cleveland Clinic Abu Dhabi initiative reduces ICU admissions and strengthens caregiver collaboration

Veteran nurse blends compassion, cutting-edge transplant training and military tradition to elevate patient care

Embrace coaching and other tips to be a stronger leader