Managing recurrent head and neck paragangliomas
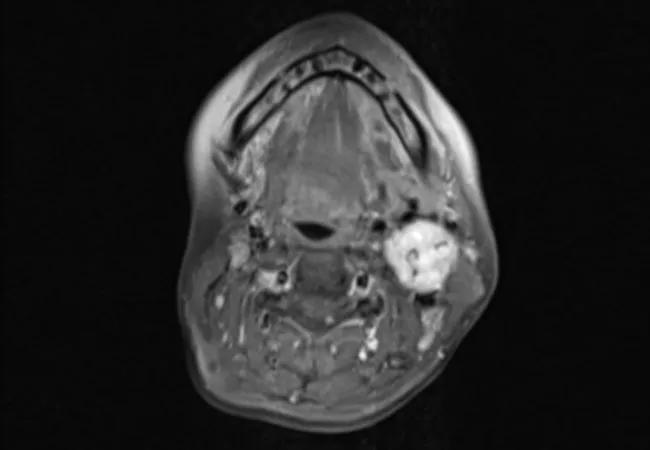
In one of the largest cohort studies of head and neck paragangliomas, study authors characterize the incidence of tumor recurrence after treatment. The study provides new insights about the risk of disease progression and offers new surveillance recommendations.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The study authors, Robert Lorenz, MD, MBA, otolaryngologist and Kevin Contrera, MD, MPH, fourth-year resident, both in Cleveland Clinic’s Head & Neck Institute, presented these findings at the American Academy of Otolaryngology-Head and Neck Surgery Annual Meeting in New Orleans on September 15.
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/ba2a062b-828c-4860-94de-453d05075160/19-ENT-4229-OTO-Conference-inset-322x440-1-220x300_jpg)
“There is an absence of evidenced-based guidelines on how patients should be followed after being treated for head and neck paraganglioma, leaving many clinicians to rely on overuse of imaging,” says Dr. Contrera, the study’s first author. “We hoped to change that with this study.”
The retrospective cohort study examined 173 adults with 189 paragangliomas (41.3% carotid body, 47 29.1% glomus jugulare, 19.0% glomus tympanicum, and 10.6% glomus vagale) who received treatment between 1990 and 2010.
Results showed that glomus jugulare tumors were more likely to recur after initial treatment (HR = 3.69, 95% CI: 1.70-8.01, P < .001), while carotid body tumors were comparatively less likely to occur (HR = 0.44, 95% CI: 0.21-0.97, P = .041). Importantly, the study also found that carotid body tumors had lower risk of recurrence with surgery compared to radiation, while globus jugulare tumors showed a lower risk of recurrence with radiation compared to surgery.
Dr. Lorenz, senior author on the study, notes, “It’s insight that may direct providers on how to best manage these specific tumors in the future.”
This study dovetails with the authors’ recently published study in Head and Neck, which offers clinical guidelines for head and neck paraganglioma surveillance. Both studies aim to develop new understandings about reoccurrence and reduce frequency of patient imaging.
Advertisement
“We are getting closer to standardizing follow-up for this patient population,” he says. “Large cohort studies like this provide evidence-based data that inform responsible imaging practices and help clinicians manage expectations with patients about recurrent tumors.”
Advertisement
Advertisement

Analysis of HNSCC patients shows HPV status to be predictive of higher abundance of oncobacteria within the tumor

Case study illustrates the potential of a dual-subspecialist approach

Evidence-based recommendations for balancing cancer control with quality of life

Study shows no negative impact for individuals with better contralateral ear performance

HNS device offers new solution for those struggling with CPAP

Patient with cerebral palsy undergoes life-saving tumor resection

Specialists are increasingly relying on otolaryngologists for evaluation and treatment of the complex condition

Detailed surgical process uncovers extensive middle ear damage causing severe pain and pressure.