TKA outcomes calculator to help counsel patients, manage expectations
By Alison K. Klika, MS and Nicolas S. Piuzzi, MD
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Total knee arthroplasty (TKA) has proven to be a safe, long-lasting solution to treat patients with knee joint disease. Despite the vast majority (90%) of patients reporting improvements in pain, function, and quality of life, there are some patients who show no improvement or may even decline.1
Data suggest that up to 20% of patients express some level of dissatisfaction following TKA, commonly associated with factors such as socio-demographic factors and baseline mental and physical health status.2 Adverse events have been linked to patient-specific factors such as comorbidities and high BMI.3
Altogether, implementation of care pathways have focused on standardizing the way patients are optimized preoperatively for many of these risk factors in an effort to minimize postoperative complications and readmission.4
As personalized medicine continues to evolve and impact how we deliver care, a data-driven approach using predictive analytics to understand specifically how an individual may or may not benefit from TKA in terms of pain and function is valuable to the physician and the patient in the shared-decision making process. The ability to predict how changes to a modifiable factor (like BMI or smoking) may impact a patient’s outcome facilitates these meaningful conversations.
Our adult reconstruction research team, with a multidisciplinary composition of physicians, data analysts, statisticians and research professionals, has built a personalized outcome prediction tool for TKA patients to be administered preoperatively.5 This effort utilized the Outcomes Management and Evaluation (OME) system, a prospective cohort database to collect demographic and perioperative outcomes (length of stay, readmission within 90 days). The team collected data on 5,958 TKA patients from July 2015 to June 2018 and patient-reported outcome measures (PROMs) at both baseline and 1-year postoperative on a subset of this cohort (N = 2,391). Specifically, these PROMs measured pain (Knee Injury and Osteoarthritis Outcomes Score [KOOS] pain subscore), function (KOOS physical function shortform [PS]), and quality of life (KOOS knee-related quality of life [QoL] subscore).
Advertisement
These data were used to construct regression models for each outcome, which were assessed for accuracy, cross-validated within the initial dataset, and then assessed for accuracy using a separate dataset from 3,750 TKA patients from July 2018 to June 2019 (1-year PROMs were collected from 2,095 TKA patients ending in June 2018 to allow for 1-year outcomes).
| Outcome | AUC |
|---|---|
| Length of stay (days) | 71.5 |
| 90-day readmission | 65.0 |
| 1-yr KOOS pain | 71.7 |
| 1-yr KOOS function | 72.6 |
| 1-yr KOOS quality-of-life | 70.5 |
| Outcome | |
| Length of stay (days) | |
| AUC | |
| 71.5 | |
| 90-day readmission | |
| AUC | |
| 65.0 | |
| 1-yr KOOS pain | |
| AUC | |
| 71.7 | |
| 1-yr KOOS function | |
| AUC | |
| 72.6 | |
| 1-yr KOOS quality-of-life | |
| AUC | |
| 70.5 |
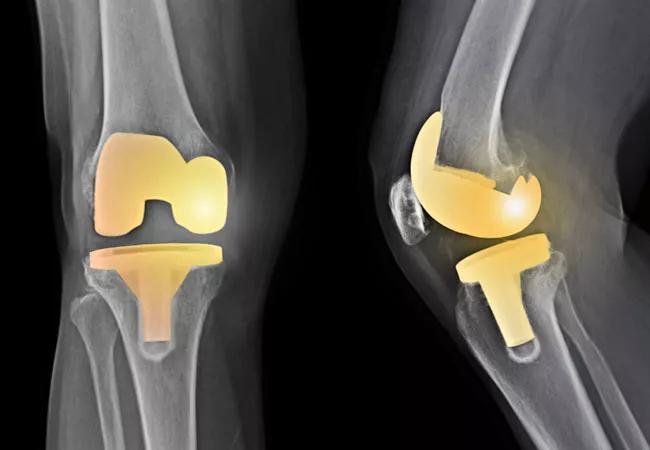
The models were programmed into an online calculator, as shown in Figure 1. This tool provides a visual display of the patient’s predicted outcomes of their surgery, which is easily interpreted.
The patient’s own outcomes are put into context by including benchmark achievements for the “typical” TKA patient. Additionally, suggestions for changes to modifiable factors can be made in real-time to show the potential for improved outcomes to the patient.
We believe that using this tool to counsel patients and set accurate patient expectations for surgery will be highly valued by physicians and their patients with the potential to positively impact patient’s lives. It was our honor to receive the 2020 Current Concepts in Joint Replacement/Orthopaedic Research and Education Foundation clinical practice award for this work.
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/02a806bf-66e5-49e2-a81c-61068523b9e0/20-ORI-1958833-CQD-Personalized-Outcome-Prediction-Knee-Arthro-Inset-300x187_jpg)
Figure 1. Predicted outcomes calculator following total knee arthroplasty. The left panel shows the information that is input into the calculator, the right panel is the output information. The patient’s predicted scores (+ or – improvement in parentheses) are shown alongside the “average” CC patient scores (blue).
Advertisement
The patient’s scores are shown in one of three colors: green, yellow, or red indicating improvement, no change, or decline, respectively. At the bottom are “Recommendations” specific to the patient regarding his/her opportunity to modify factors that may improve outcomes.
About the authors
Dr. Piuzzi is a staff orthopaedic surgeon who serves as the Director of the Adult Reconstruction Research Team, with a focus on hip and knee replacements as well as orthobiologics and joint preservation.
Ms. Klika is the Research Program Manager for adult reconstruction in Ohio as well as orthopaedics in Cleveland Clinic Florida.
Additional individuals to acknowledge for this work are Carlos Higuera, MD; Robert Molloy, MD; Kurt Spindler, MD; and Greg Strnad, MS.
References
Advertisement
Advertisement
Advertisement

How it’s similar but different from the direct anterior approach

Collaboration must cross borders and disciplines

Systematic review of MOON cohorts demonstrates a need for sex-specific rehab protocols

Should surgeons forgo posterior and lateral approaches?

How chiropractors can reduce unnecessary imaging, lower costs and ease the burden on primary care clinicians

Why shifting away from delayed repairs in high-risk athletes could prevent long-term instability and improve outcomes

Multidisciplinary care can make arthroplasty a safe option even for patients with low ejection fraction

Percutaneous stabilization can increase mobility without disrupting cancer treatment