Studies investigate two potential risk-prediction methods
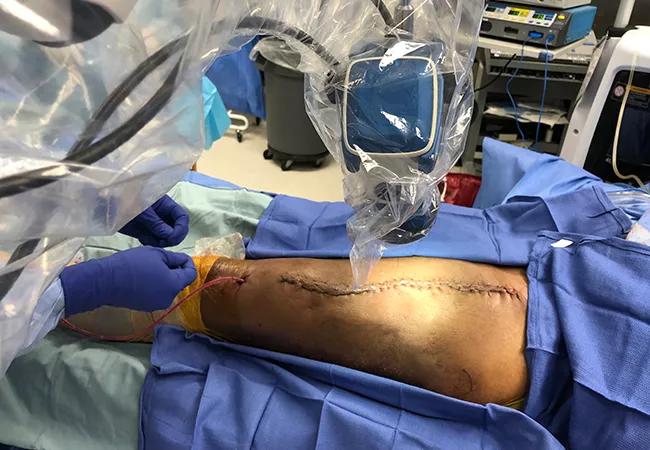
Soft tissue sarcomas are serious but potentially treatable cancers. Radiation therapy and limb-salvage surgical resection can be curative if the disease is localized.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Radiation therapy can be given either before or after surgery. Typically, it is done first in order to kill microscopic disease around the tumor to make removal safer around critical structures. Preoperative radiation therapy uses a smaller dose compared to postoperative treatment and results in better overall limb function.
“Unfortunately, radiation can cause collateral damage, which can lead to wound healing complications after surgery,” says orthopaedic surgeon Lukas Nystrom, MD, who specializes in orthopaedic oncology at Cleveland Clinic.
In one study, such complications occurred in about 35% of all cases and 43% with lower extremity tumors, compared to just 17% of patients who received postoperative radiation.
“Patients who experience complications have a significantly diminished quality of life as measured by our patient-reported outcome instruments,” says Dr. Nystrom. “The situation can persist for many months. We can manage it, but it involves multiple trips to the operating room, a ton of extra medical visits, increased pain and a lot of psychological distress.”
To reduce wound healing complications following resection of soft tissue sarcoma, Dr. Nystrom is leading a team at Cleveland Clinic that is exploring methods for identifying patients who may be at greater risk.
“If we can determine up front which patients are going to have trouble with wound complications, then we can potentially take steps to avoid it and improve their experience,” he says.
Techniques to reduce the risk of wound healing complications potentially include altering the timing of surgery, vacuum-assisted closure, hyperbaric oxygen therapy and using surgical flaps in areas where healing potential is compromised.
Advertisement
There currently are no reliable laboratory or clinical criteria to predict which patients are more likely to develop wound healing complications.
Dr. Nystrom and his colleagues are investigating two methods to help with that prediction: transcutaneous oxygen (TcO2) measurement at the surgical site to determine skin perfusion, and near-infrared fluorescence imaging with indocyanine green (ICG).
The team has already completed a prospective study of transcutaneous oximetry in 39 patients, finding a trend toward decreased TcO2 in those who had wound healing complications, although it was not statistically significant. Dr. Nystrom hypothesizes that this may be related to sampling a very limited area of the surgical resection. These data were presented at the 2021 Musculoskeletal Tumor Society Annual Meeting and are currently being prepared for publication.
Potentially more informative is ICG, a fluorescent biomarker that has been used for intraoperative assessment of perfusion in plastic reconstruction surgery, for identification of lymph nodes and in assessment of cardiac function.
A recently launched prospective study aims to enroll 50 patients with biopsy-proven soft tissue sarcoma of the upper or lower extremity to be treated with limb-salvage surgical excision. It is the first investigation trying to quantify tissue perfusion and relate it to post-surgical wound healing in this patient population, says Dr. Nystrom.
Advertisement
Advertisement

Radiation therapy helped shrink hand nodules and improve functionality

Standard of care is linked to better outcomes, but disease recurrence and other risk factors often drive alternative approaches

Phase 1 study demonstrates immune response in three quarters of patients with triple-negative breast cancer

Multidisciplinary teams bring pathological and clinical expertise

Genetic variants exist irrespective of family history or other contributing factors

Study shows significantly reduced risk of mortality and disease complications in patients receiving GLP-1 agonists

Structured interventions enhance sleep, safety and caregiver resiliency in high-acuity units

Addressing rare disease and challenging treatment course in an active young patient