Robot scores better in length of stay and home discharge; manual scores better in flexion and operative time
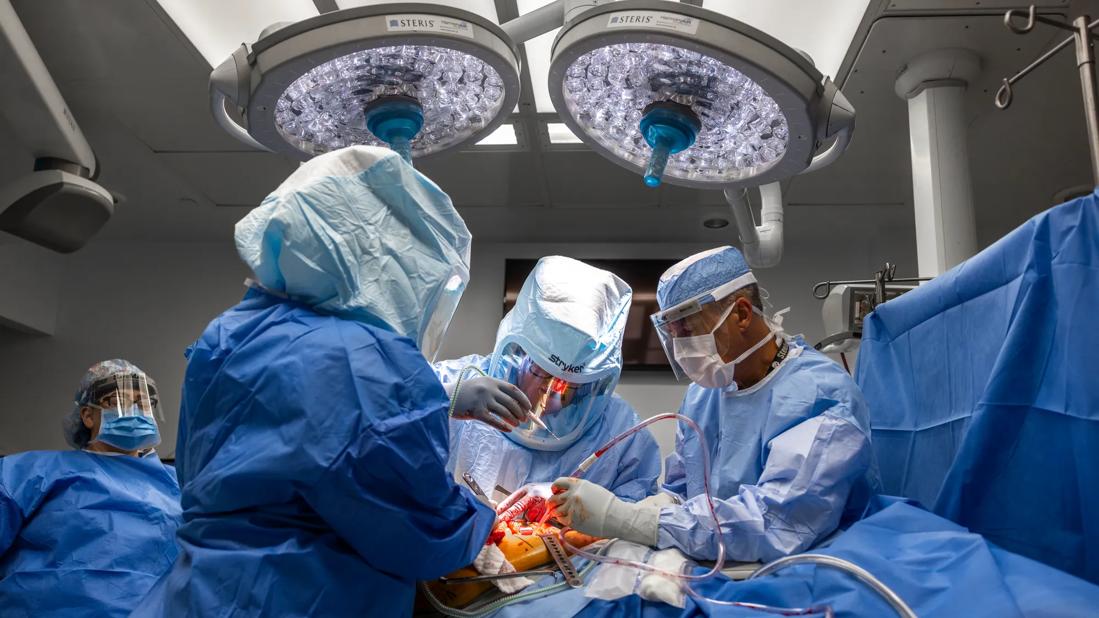
Robotic arm-assisted total knee arthroplasty (TKA) currently has some advantages over manual surgery, although either technique is effective. With time, though, robot-assisted surgery is expected to emerge as the procedure of choice for TKA.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A group of Cleveland Clinic orthopaedic surgeons recently analyzed 12 categories of data from 340 patients who had either robot-assisted or manual TKA. Results were mixed — the robot scored better on length of hospital stay and home discharge, but operative times were shorter with manual surgery. The two procedure types were the same in regard to postoperative complications.
“Robot assistance is new technology that we want to be successful,” says study coauthor Kim Stearns, MD, Chief of Surgery at Cleveland Clinic Lutheran Hospital. “So far, in the early use of the robot, it’s not substantially better than the way we’ve always done it, at least for many of the 12 things we measured. I still think that in the long run we’re going to show that the robot is better technology, and that implants will last longer and patients will do better.”
Dr. Stearns and colleagues analyzed the records of 895 Cleveland Clinic patients who had either robotic arm-assisted or manual TKA from January 2017 through August 2018. Lutheran Hospital was the first Cleveland Clinic hospital to acquire the robot, in 2016.
Using 3:1 propensity score matching for underlying baseline characteristics that could affect outcomes, the researchers were able to match 255 patients who had manual TKA with 85 patients who had robot-assisted TKA.
There were no significant differences between the two groups in perioperative pain scores, opioid use, 90-day complications or reoperations. At one year, there were no significant differences in several patient-reported outcomes, including pain and quality of life.
Advertisement
The robot proved advantageous for shorter length of stay (0.48 vs. 1.2 days, P < .001) and home discharge (98.8% vs. 96.8%, P < .001).
However, manual TKA came out ahead for maximum flexion at 90 days (120.3 degrees vs. 117.8 degrees, P = .043), shorter operative time (105 minutes vs. 113 minutes, P < .001), and fewer postoperative physical therapy visits (median 10.0 vs. 11.5, P = .014).
Which procedure to choose for a given patient depends on clinical factors, as well as patient and surgeon preference. Dr. Stearns currently uses the robot for about one in three of his TKA patients, usually those with more complicated deformities. Robotic bone cuts allow him to balance ligaments better than when done manually. Anecdotally, he has seen less pain and less opioid use in patients who have had robot-assisted surgery compared to patients who have had conventional surgery.
With just one robot at Lutheran Hospital, Dr. Stearns and his colleagues were limited to performing about three robot-assisted procedures per day. However, the hospital recently obtained a second robot, bringing the total throughout Cleveland Clinic health system to seven. This will greatly increase the capacity for robot-assisted TKAs at Cleveland Clinic.
It should make a difference in outcomes as well, says Dr. Stearns.
“We’re going to continue to evaluate every one of these surgeries that we do,” he says. “As the robot is used more widely, I think we’ll see shifts in some of the outcomes. When we start using the robot for the majority of knees and not just the complex knees, I think we’ll see that using the technology is more favorable than not using it.”
Advertisement
For now, he says, the study demonstrated that using the robot for TKA is safe, effective and noninferior to the manual procedure.
“It’s great technology,” says Dr. Stearns. “We’re still learning its benefits and when we most need to use it. For people with challenging knees, it’s better than anything we’ve had before.”
Advertisement
Advertisement

Self-care may be just as effective for some patients

Most return to the same sport at the same level of intensity

More report a clinically meaningful change in function at 90 days compared to patients with lower BMI
How to diagnose and treat crystalline arthropathy after knee replacement

Special glasses allowed surgeon to see 3D models and anatomic data superimposed on surgical field

When procedure is performed by high-volume surgeons, outcomes are comparable to total knee replacement

Study findings warrant caution in patients at risk for DVT, cardiovascular issues and more
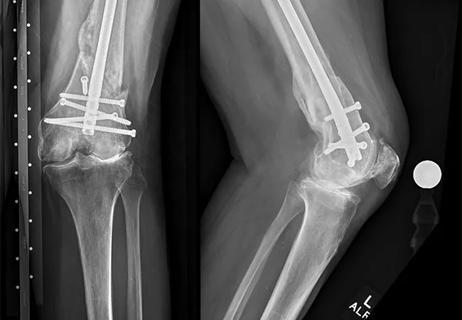
Robot assistance turns two-stage surgery into a single procedure