Syphilis resurfaces as a major concern
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
A 39-year-old man presented to the emergency department reporting several weeks of generalized weakness, headache, nausea, and migratory arthralgia. The patient had exclusively had sex with men, had participated in condomless anal insertive and receptive intercourse, and had been in a monogamous relationship during the past 6 months.
Physical examination revealed a painful ulcerated plaque on the upper lip, a macular rash with three crater-like scarred painless lesions (considered to be healing chancres) on the glans, a nonpruritic hyperkeratotic maculopapular palmar rash and bilateral submandibular lymphadenopathy. No alopecia, gummas, neurologic deficits or ocular or cardiovascular abnormalities were noted.
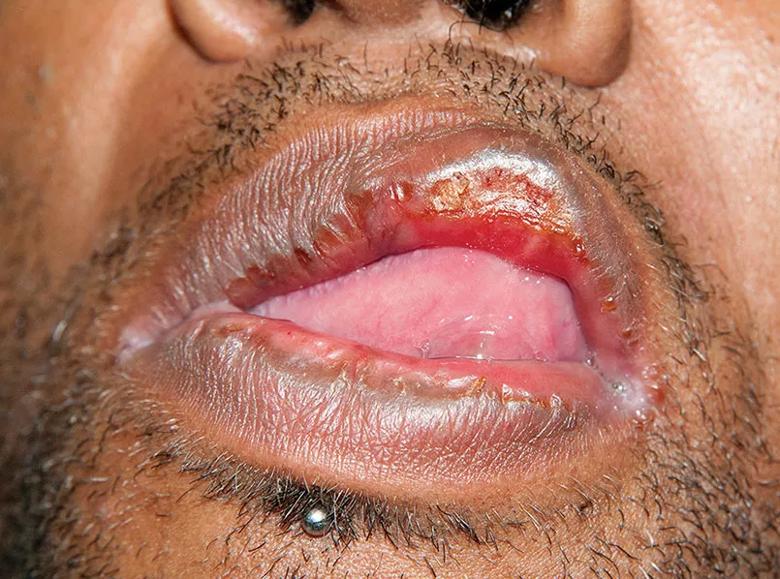
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/792702a0-394a-45dd-b98e-7d3e36e35609/805x-Inset-1-Secondary-Syphilis_jpg)
Ulcerated plaque on the upper lip.
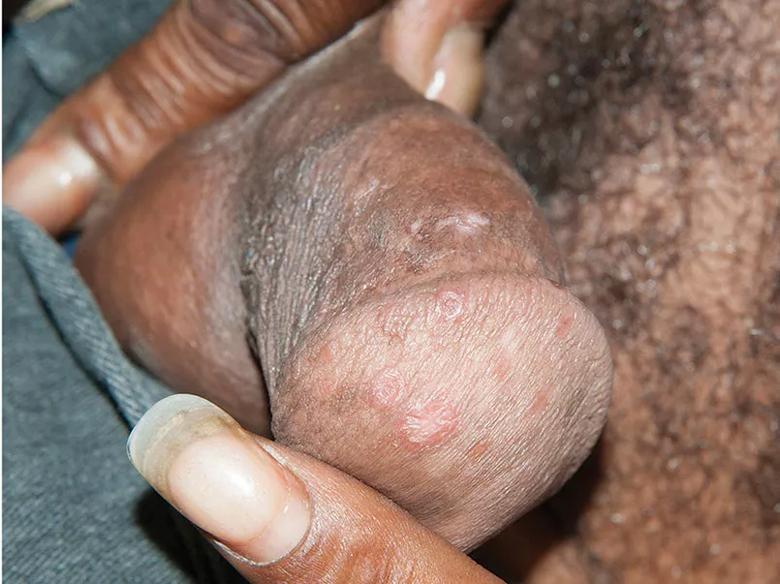
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/e1e90aad-436c-493d-b1e0-0f85b3d500aa/805x-Inset-2-Secondary-Syphilis_jpg)
Macular rash with painless scarred lesions.
Results of laboratory testing included a positive reactive syphilis immunoglobulin G (IgG) enzyme immunoassay and a positive rapid plasma reagin (RPR) test (titer 1:256). Human immunodeficiency virus (HIV) testing was negative, and serologic testing demonstrated prior immunization to hepatitis B virus. Given the clinical presentation and laboratory findings, secondary syphilis was considered the most probable diagnosis.
The patient was treated with benzathine penicillin G 2.4 million units intramuscularly.
The rate of reported primary and secondary syphilis cases in the United States has risen since 2001. Most cases occur in men who have sex with men. Additional risk factors include condomless intercourse and drug use.
Primary syphilis begins two to three weeks after inoculation of a mucosal surface. This stage is marked by one or more painless chancres and, in some cases, local nontender lymphadenopathy. Secondary syphilis presents four to eight weeks later with systemic symptoms including rash, classically involving the palms or soles, lymphadenopathy, myalgia, fever and weight loss. Untreated primary and secondary syphilis may progress to latent or asymptomatic disease.
Advertisement
Tertiary syphilis, defined by the US Centers for Disease Control and Prevention (CDC) as gummas or cardiovascular syphilis, occurs 15 to 30 years after an untreated exposure. Neurosyphilis can present at any stage of the disease.
The diagnosis of syphilis involves a nontreponemal test such as RPR or Venereal Disease Research Laboratory (VDRL) to screen for disease, followed by a treponemal antibody test such as fluorescent treponemal antibody-absorption, Treponema pallidum particle agglutination assay or syphilis IgG to confirm the diagnosis. There is no screening test for tertiary disease in patients previously diagnosed with primary or secondary syphilis, but a cerebrospinal fluid (CSF) examination is recommended if neurologic or ocular manifestations are present.
Treatment of primary, secondary and early latent syphilis is a single dose of 2.4 million units of benzathine penicillin G given intramuscularly. The treatment of late latent and tertiary syphilis is less well defined by the current literature but generally includes penicillin.
Patients with primary and secondary syphilis undergo serologic and clinical evaluation at six and 12 months to be assessed for treatment failure or reinfection. Patients with latent disease require serologic follow-up at six, 12 and 24 months. Additionally, CSF analysis should be done if baseline high titers do not fall within 12 to 24 months of treatment or if symptoms suggest syphilis. Patients with neurosyphilis often require CSF evaluation every six months. Follow-up for patients with tertiary syphilis is less well defined.
Advertisement
Sexual contacts of patients with syphilis deserve evaluation. Exposure within 90 days of a patient’s diagnosis with primary, secondary or latent disease requires treatment regardless of the results of serologic testing. Persons exposed more than 90 days before diagnosis may undergo serologic testing; however, if results are not immediately available or follow-up is unlikely, the individual should be treated for early syphilis. If serologic testing results are negative, no treatment is required.
Dr. Brateanu is staff in the Department of Internal Medicine.
This article originally appeared in Cleveland Clinic Journal of Medicine. To view the original version, click here.
Advertisement
Advertisement

Emerging evidence suggests a patient-specific approach

Not if they meet at least one criterion for presumptive evidence of immunity

Essential prescribing tips for patients with sulfonamide allergies

Confounding symptoms and a complex medical history prove diagnostically challenging

An updated review of risk factors, management and treatment considerations
OMT may be right for some with Graves’ eye disease

Perserverance may depend on several specifics, including medication type, insurance coverage and medium-term weight loss

Abstinence from combustibles, dependence on vaping