Dysphagia and SUVmax are predictive, but other suspected factors are not
Esophageal cancer is an aggressive malignancy that is on the rise. It is especially difficult to diagnose at the early T2N0 stage, which can make it hard for physicians to know whether the patient should go directly to surgery or undergo chemo- and radiotherapy first. Now a new Cleveland Clinic study has identified key features for improving diagnosis and guiding treatment decisions.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Specifically, the researchers found that the presence of preoperative dysphagia and a maximum standardized uptake value (SUVmax) for the tumor of 5 or higher on PET scan predict upstaging — indicating that the patient would benefit from multimodal treatment.
“If we can recognize these high-risk markers for upstaging preoperatively, we can offer patients neoadjuvant therapy,” says Sadia Tasnim, MD, a Cleveland Clinic thoracic surgery research fellow and first author of the study, which was presented at the 2023 annual meeting of the Society of Thoracic Surgeons.
The findings are important because esophageal cancer rarely presents at the T2N0 stage, when it is most treatable.
True T2N0 patients should undergo up-front surgery, whereas patients who have underlying advanced disease beyond T2N0 benefit more from multimodal therapy, notes Cleveland Clinic thoracic surgeon Monisha Sudarshan, MD, MPH, the study’s principal investigator.
“It’s important to accurately diagnose the stage,” Dr. Sudarshan explains, “because if we believe someone is T2N0 and they undergo surgery, and we find out later that they’re actually beyond T2N0, then we have not given them the advantage of chemotherapy and radiation preoperatively. That impacts their overall survival.”
However, she adds, physicians currently have few reliable tools to accurately diagnose a T2N0 esophageal cancer, due to limitations in endoscopic staging.
Some small retrospective studies have previously looked at this issue, but Dr. Sudarshan notes that no prior study comprehensively analyzed preoperative factors that can predict pathologic upstaging of cT2N0M0 esophageal cancer.
Advertisement
The Cleveland Clinic study identified 60 patients who underwent up-front surgery for clinical T2N0 esophageal cancer between 2000 and 2020. Patients who received chemotherapy and radiation were excluded. The researchers looked at the relationship between different variables and tumor upstaging.
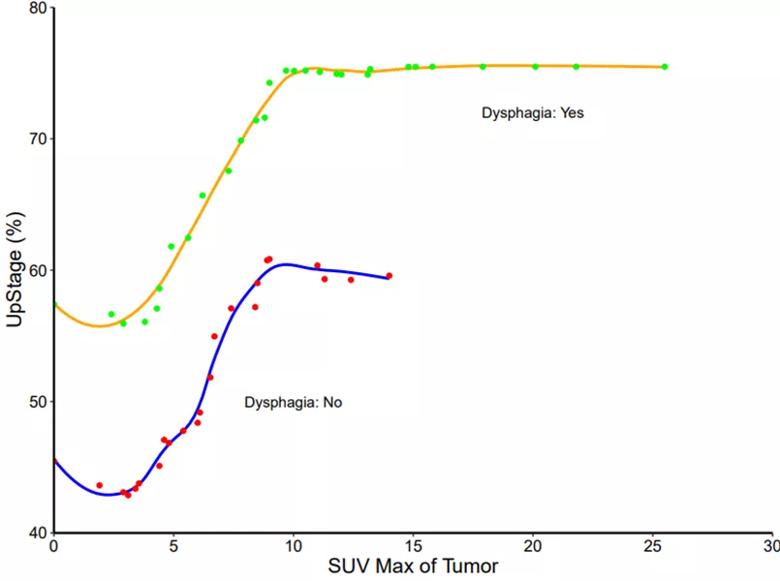
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/f42956ea-f933-4501-a213-6ba218e41743/23-HVI-3555159-CQD-Inset_jpg)
Figure. Partial dependence plot predicting upstaging by SUVmax stratified by the presence of preoperative dysphagia.
Dr. Tasnim says they expected that dysphagia and higher SUVmax would be predictors of upstaging (see Figure). They were surprised, however, that other factors — including tumor size and the presence of strictures on endoscopy — were not predictors.
This could be a limitation of the sample size, Dr. Sudarshan points out, but she adds that this is actually one of the larger studies of the subset of patients who have this rarely diagnosed stage of cancer. “T2N0 is a stage at which you can still do quite a bit of good for these patients, as it is so early,” she says. “So these patients are a small but important group.”
Next, the team plans to continue its research by gathering more data to gain better insights.
“For example,” Dr. Sudarshan notes, “the presence of ulcer showed a trend toward upstaging, but this trend was not statistically significant. We wonder if that is just because we didn’t have enough patients, so we plan to recruit more patients and do a follow-up investigation.”
“In the meantime,” she continues, “this study’s findings have impacted the way we manage patients with T2N0 esophageal cancer. If we see patients with this stage of cancer who have difficulty swallowing or a high SUVmax, they will likely get preoperative chemoradiotherapy.”
Advertisement
“As we continue to understand and appreciate the nuances of esophageal cancer presentation,” adds study co-author Sudish Murthy, MD, PhD, Section Head of Thoracic Surgery at Cleveland Clinic, “the era of personalized esophageal cancer care becomes a clear target for patients.”
Advertisement
Advertisement

Microvascular “supercharging” is a critical newer step to promote favorable outcomes

Long-acting antiemetics and high-dose steroids key to minimizing acute nausea

Radiation therapy helped shrink hand nodules and improve functionality

Standard of care is linked to better outcomes, but disease recurrence and other risk factors often drive alternative approaches

Phase 1 study demonstrates immune response in three quarters of patients with triple-negative breast cancer

Multidisciplinary teams bring pathological and clinical expertise

Genetic variants exist irrespective of family history or other contributing factors

Study shows significantly reduced risk of mortality and disease complications in patients receiving GLP-1 agonists