Suicidal ideation elevated in American Indian/Alaska Native and Black populations

Monitoring of minority children with epilepsy should be a priority, given their high rates of suicidality, according to a Cleveland Clinic study presented at the American Epilepsy Society annual meeting. The results show that American Indian/Alaska Native and Black patients are the populations most at risk for serious mental health issues.
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“We found that children with epilepsy were four times more likely to report suicidal thoughts than other pediatric patients,” says the study’s senior author, Tatiana Falcone, MD, MPH, a psychiatrist with Cleveland Clinic’s Center for Behavioral Health and Epilepsy Center. “We think that is because, over the long term, their symptoms of depression are going unrecognized and untreated.”
The problem was particularly pronounced in minority populations, who were more likely to report symptoms of depression than their white counterparts.
“Lack of access to mental health services and stigma about mental health conditions may have contributed to the results in minority patients,” says Dr. Falcone. “That is in keeping with data showing a higher incidence of suicide among African American and Hispanic children during the COVID-19 pandemic.”
The researchers compared mental health screening results from 2,542 pediatric patients with epilepsy against results from 21,134 patients in the general pediatric population at Cleveland Clinic. The Patient Health Questionnaire for Adolescents A (PHQ-A) was used to screen the patients with epilepsy from September 2019 through July 2022. The Patient Health Questionnaire-9 (PHQ-9) was used to screen the general pediatric population between January 2020 and the beginning of September 2020.
The PHQ-9 is a nine-item survey about a person’s mental health over the prior two weeks. The symptoms described range from having little interest or pleasure in doing things (question 1) and trouble with sleep and appetite (questions 3 and 5) to thoughts of being better off dead or hurting oneself (question 9). Each answer is scored from 0 to 3, resulting in a severity score from 0 (no positive responses at all) to 27 (all symptoms experienced nearly every day). The PHQ-A is a modified version of the PHQ-9 for adolescents.
“If a patient is having trouble sleeping or eating because they are depressed, they might forget to take their medication and then have more seizures,” notes Dr. Falcone. “That, in turn, could worsen their epilepsy. The longer the depression persists, the harder it is to treat and the more likely that a patient will develop suicidal thoughts.”
Among the general pediatric population at Cleveland Clinic, 4% of patients aged 12 to 21 reported suicidal thoughts on the PHQ-9, compared with 16% of the pediatric patients with epilepsy screened with the PHQ-A.
Among the patients with epilepsy, 9.57% of females and 4.76% of males responded to question 9 with a score of 1 or higher, meaning they screened positive for suicidality.
Assessing the association between race and suicidality, the researchers found that 16.67% of American Indian/Alaska Native pediatric patients with epilepsy gave a positive response to question 9, which was consistent with elevated rates in previous studies. Incidence of suicidal thoughts was also modestly increased among Black (8.10%) and multiracial (8.06%) patients with epilepsy compared with white patients with epilepsy (7.55%).
Analysis by age showed that the oldest patients in the pediatric epilepsy cohort (ages 21 to 24 years) were more likely than the five younger age groups to screen positive on question 9.
The researchers’ next step is to publish their results in manuscript form, which they expect to do in the spring of 2023. Currently underway is a project with the online mental health platform SilverCloud® through which pediatric patients at Cleveland Clinic use a mobile app to increase their skills for coping with depression. Outcomes will be compared between cohorts with epilepsy and depression and diabetes and depression versus those with depression alone.
“An illness that affects the brain like epilepsy does may put patients at elevated risk of worsening depression and suicidal thoughts,” observes Dr. Falcone. “Mental health is a vital sign for which we should be screening each time a child with epilepsy presents so that we can provide better care.”

Consultation service provides comprehensive care to patients with anxiety, PTSD, schizophrenia, and other high-risk disorders

Characterizing genetic architecture of clinical subtypes may accelerate targeted therapy

Patients who score lower than 40 on the VR-12 Mental Component Summary need more care after surgery
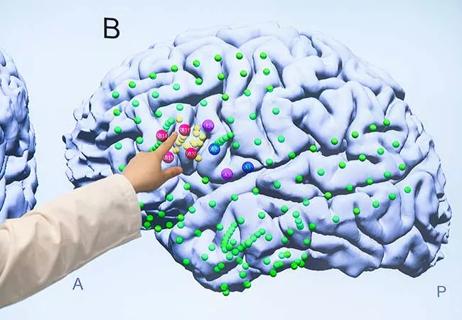
‘Cleveland Clinic Epilepsy Update’ offered as hybrid in-person and online CME event
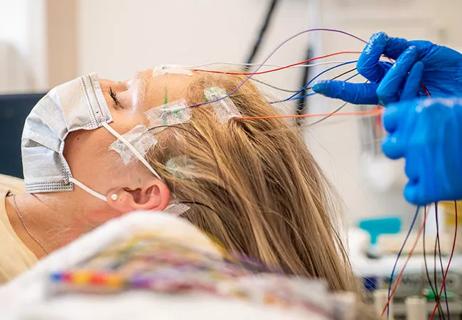
ILAE advises emphasizing options for patients with drug-resistant epilepsy
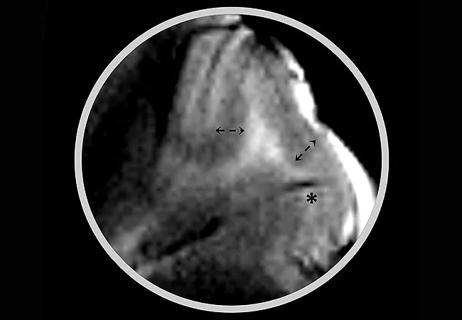
Mounting support for the newly described microstructure from a 7T MRI and electroclinicopathologic study

Study shows a growing openness to the clinical potential of psychedelic treatments

Urine test strips and point-of-care testing may be key to slowing opioid epidemic