Locations:

Program's approach maximizes donor safety without compromising recipients' outcomes

Cleveland Clinic’s team reviews progress and offers guidance
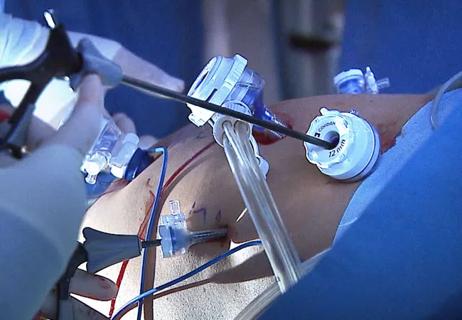
Technically demanding procedure reduces morbidity and recovery time for donors

Reduces waiting time and prevents morbidity and mortality
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy

A Q&A with Drs. Hashimoto and Kwon

Even the youngest, smallest patients can be recipients
Advertisement
Advertisement