COVID-19 pandemic offers insights for a nimble nursing workforce.
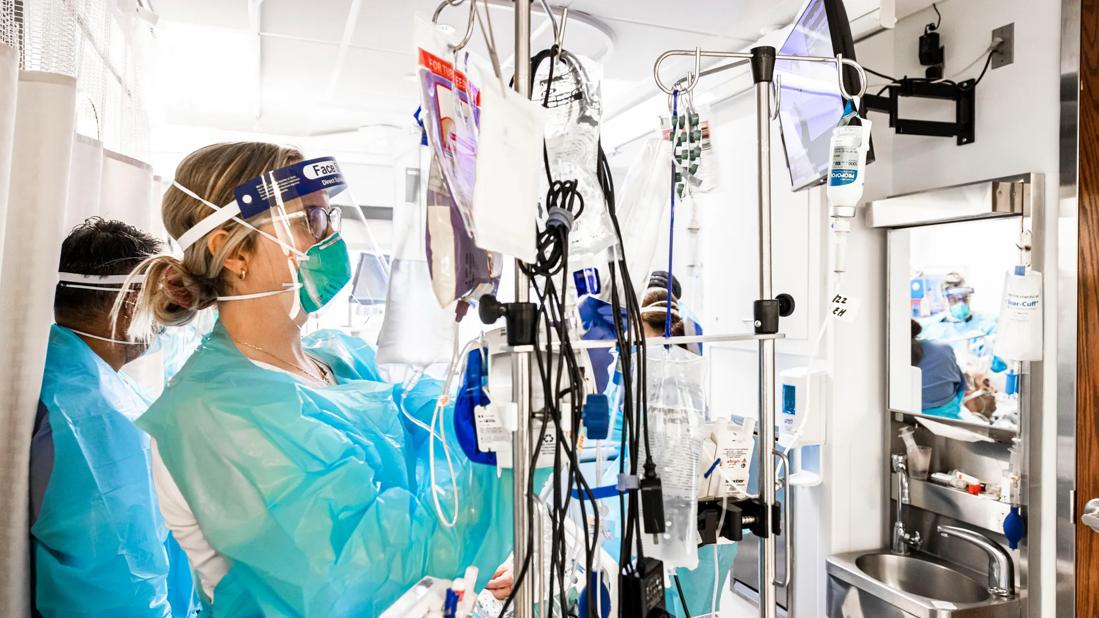
When nursing caregivers at Cleveland Clinic Marymount Hospital began treating COVID-19 inpatients in the spring of 2020, teams quickly learned that they could preserve personal protective equipment (PPE) by allowing one nurse to remain at the patient’s bedside in gown, mask and shield while others worked as runners, staying outside the room to retrieve supplies and personnel.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
That protocol sounds simple, but it had not been standard procedure before the pandemic created a supply shortage that extended around the world. Using runners to support gowned caregivers is just one of the resource management adaptations to emerge from the COVID-19 crisis. As the pandemic stretches on, nursing leaders and educators are reviewing what the pandemic has taught them about managing time, skills, equipment and personnel in a changing healthcare landscape.
At Cleveland Clinic and other hospitals, numbers of COVID-19 cases have swelled and receded, but the development of strategies for a new era is ongoing. Among those at the forefront have been Carol Pehotsky, DNP, RN, NEA-BC, ACNS-BC, CPAN, Associate Chief Nursing Officer, Surgical Services, and Senior Director of Surgical Nursing at the main campus; Kristine Adams, MSN, CNP, Associate Chief Nursing Officer, Care Management and Ambulatory Services, and Senior Director of Chronic Disease Clinics at the main campus; and Barbara Zinner, DNP, RN, NE-BC, CENP, Chief Nursing Officer at Marymount Hospital.
In early 2020, Cleveland Clinic nursing leaders began rethinking almost every assumption about how to leverage the health system’s nursing talent for a patient surge.
“At that time, we were building the Hope (surge) Hospital and asking ‘How do you staff another 1,000 beds without adding any new nurses?’” Adams says. “We discussed how nurses in some areas might be more easily reassigned, and where best to use their individual skill sets. For example, a nurse may now be focused on work in the field of quality, but formerly the nurse was clinically competent in the field of emergency department care. The question became: What do we need to do to prepare nurses to be reassigned to a previous role or work environment, should we need to do so?”
Advertisement
The plan identified a centralized group of decision-makers who could quickly triage the needs of individual hospitals and decide where to focus nursing caregiver support. Early on, Marymount Hospital was to be a hub for COVID-related care. At its peak, Dr. Zinner says, COVID-19 patients occupied 25 of the community hospital’s 28 open ICU beds and another 70 medical-surgical beds. When case numbers quickly overwhelmed capacity, Marymount nurses shared their experiences and practices (including the use of runners) to help caregivers as other Cleveland Clinic hospitals began treating pandemic patients.
As hospital leaders managed bed placement and care for a wave of patients, they also began to manage a shrinking nursing workforce.
Before COVID-19, “We had a lot of nurses working past their retirement age,” Adams says. The first wave of nurses who left their positions, she adds, were those who could have retired years ago, based on age alone. Another subset of people who had planned to retire in 2020 or 2021 decided to leave earlier than planned.
Some nurses left after contracting the virus, including a few who became seriously ill and suffered as COVID-19 “long-haulers.” As caregiver shortages hit hospitals, travel nurse agencies began offering monetary incentives, including signing bonuses, to newly graduated nurses who might otherwise have started their careers as clinical nurses on a hospital unit.
In the face of these workforce challenges, Cleveland Clinic’s Nursing Institute became a “shining star” by creating classes to train experienced nurses for new assignments, Dr. Pehotsky says. When elective surgeries were temporarily canceled because of the pandemic, OR nurses became available for other assignments.
Advertisement
“We did our very best to send nursing caregivers to training classes before sending them to a nursing unit or ICU,” Pehotsky says. “Caregivers were matched with clinically experienced nurses as soon as possible after the class, and whenever possible, to gain experience with oversight. In my specialty [perioperative nursing], some nurses had never worked in an ICU or on a medical-surgical unit before.”
Nursing Education expanded class availability to accommodate a variety of schedules so training could be completed in a short period of time. “Train-the-trainer” practices increased the number of people who could share information, Pehotsky adds, and became a practice that is expected to continue.
For nurses and managers, flexibility has become an indispensable tool. Nurse managers plan to extend help to newly cross-trained caregivers as if they were recent graduates who had to learn from the bottom up. Further, students and new nurse graduates are educated with flexibility in mind.
“Hyper specialization may not be sustained for the long term, especially if the workforce landscape continues to reflect high vacancy rates,” Adams says.
The pandemic has also provided lessons about the need for vigilance with supplies. Cleveland Clinic developed a process to sterilize and reprocess N95 masks so that they could be reused if mask supplies dwindled. Although the reprocessed masks have not yet been needed, they remain in storage for a “rainy day,” Pehotsky says. Early in the pandemic, surgery teams sent their disposable gowns to COVID-19 units and switched to cloth gowns that are sterilized and reused.
“We got creative around what could be used where,” Pehotsky says. “Our Supply Chain department worked closely with us to find acceptable substitutes for hair coverings — not just in terms of covering, but in terms of infection prevention. It will be important to maintain communication with supply chain experts as the pandemic continues so that we can be ready for a future crisis.
Advertisement
Nursing leaders expect many of the changes wrought by the pandemic to continue. New models of care could include systems in which non-nurse caregivers provide clinical support under the direction of licensed nurses. Telehealth and telemedicine solutions might expand remote care options, but only if the novel technology can be easily accessed and used by patients and providers. In ambulatory home care, sending a nurse to 10 homes a day will not help, Adams says.
“But we can monitor people remotely, Adams adds. “And we can leverage unlicensed, non-nursing personnel to deliver equipment and supplies. The goal is to facilitate efficient and effective healthcare that promotes improved clinical patient outcomes.”
In addition, leaders are learning from hospitals that are often in the paths of natural disasters. These facilities continually invest in training so that special teams can be deployed as needed during a crisis.
“We are committed to ensuring that our nurses are able to maintain training,” Pehotsky says. “We’ve learned that regular updates and repeat training are necessary to ensure that nurses are ready to shift roles when needed. It is easy to attend training and then lose content details if training is not followed by actual clinical experience. Regular retraining promotes development of core competencies that can be expanded on when necessary.”
Advertisement
Advertisement

Planning continues with critical, patient-focused input from nursing teams

Strengthening care through targeted resources and frontline voices

Embracing generational differences to create strong nursing teams

CRNA careers offer challenge and reward

An unexpected health scare provides a potent reminder of what patients need most from their caregivers

Cleveland Clinic Abu Dhabi initiative reduces ICU admissions and strengthens caregiver collaboration

Veteran nurse blends compassion, cutting-edge transplant training and military tradition to elevate patient care

Embrace coaching and other tips to be a stronger leader