How can we use them to our advantage?
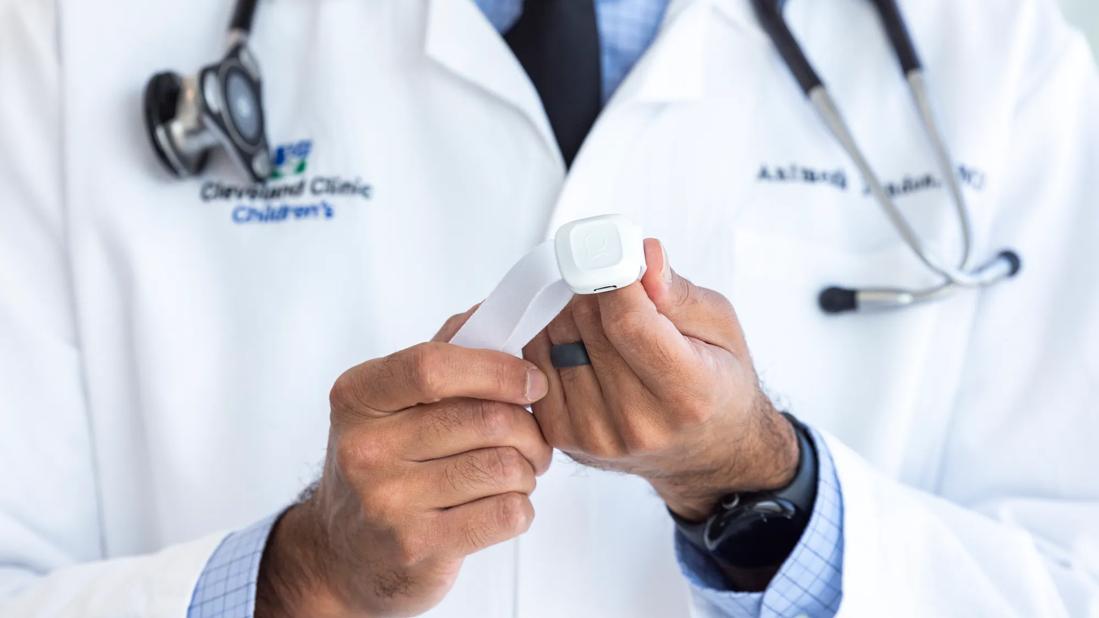
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/e6865826-f69c-498c-a819-b5d5e36189b1/CHP_4966058_06-21-24_1010_AMO)
Tandon, MD
By Animesh (Aashoo) Tandon, MD, MS
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Wearable and noninvasive biosensors, or wearables, are everywhere these days: on your wrist, in your shoes or clothes, or even just in the room. Many wearables are being used by consumers to help track and understand their health. What is not clear is exactly what we should be measuring, when, and for whom? How can we use wearables to our advantage to improve outcomes for children and patients with congenital diseases?
I have been interested in trying to answer these questions since I was a trainee at Cincinnati Children’s Hospital Medical Center and Emory University. In my prior position at Children’s Medical Center Dallas and University of Texas Southwestern Medical Center, our collaborative research group started designing some experiments to better understand how we should be using these wearable technologies for patients with congenital heart disease.1
At UT Southwestern, I formed a partnership with biomedical engineers, including Dr. Nanshu Lu at UT Austin and Dr. Omer Inan at Georgia Tech, to help investigate a new biological signal (biosignal) called seismocardiography (SCG), which, in essence, is measuring minute vibrations of the chest. This technology had never been used in children or in patients with congenital heart disease. In conjunction with the team at UT Austin, I helped think about a new form factor for measuring this biosignal.2
Dr. Inan’s group had already shown that their SCG wearable could help differentiate adults with heart failure who are doing better or worse.3 In the long run, we wanted to be able to see whether this technology would work in patients with congenital heart disease as well. Since the technology had never been used in congenital heart disease, we wanted to start by seeing whether we could use SCG to estimate stroke volume, which is the amount of blood the heart pumps every heartbeat.
Advertisement
In patients with congenital heart disease, the stroke volume can change depending on how hydrated the patient is, how well the heart is functioning, and because of progression of their disease. However, measuring stroke volume is difficult to do. Cardiac MRI is a gold standard measurement of stroke volume because we actually get to see the heart move through the cardiac cycle and can directly calculate how much blood is being pumped.
So in our recently published study with Georgia Tech and UT Southwestern,4 we put the SCG wearable on patients with congenital heart disease who were undergoing a cardiac MRI. Using the MRI, we measured stroke volume and then used the signals from the wearable to see if we could estimate stroke volume. We were able to do this very well, especially as compared to other noninvasive technologies and within the commonly accepted error of measurement.

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/cac45851-5c39-4f36-85f0-59ef459021b1/22-CHP-3274367-CQD-Perspectives-Second-Send-DrTandon-Article-cardiology650x450_jpg)
Figure. The UT Austin (top) and Georgia Tech (bottom) wearable SCG biosensors, applied to the chest of a 10-year-old patient undergoing a cardiac MRI.
I was recruited to Cleveland Clinic Children’s, in part, to continue expanding the science behind the use of wearable biosensors in congenital heart disease, and I was excited to partner with other clinicians and scientists, both in pediatric and adult medicine, to investigate these uses.
We are already designing a study that we will run here at Cleveland Clinic Children’s to use the SCG wearable biosensor to detect changes in cardiac output, or how much blood the heart pumps per minute in patients who have just undergone surgery for congenital heart disease. Given that the development of low cardiac output syndrome is one of the most common and most dangerous problems after heart surgery, this could really help us better manage patients after surgery.
Advertisement
In addition, our group is working on understanding how patients and parents interact with this technology when they’re at home. It is not clear now whether using a wearable will make parents and patients more anxious or less anxious, and what kinds of factors about the wearable itself make people more or less likely to actually keep the biosensor on. We are developing a method of measuring different aspects of the patient and parent experience.
We are also using wearable biosensors that measure heart rate and oxygen saturation to see if we can find ways to predict when babies with heart disease, who are at high risk of complications, might need extra help, and to see changes in heart rate and activity in patients who undergo heart valve replacement.
All of the studies our explicitly designed to take into account the potential different experiences of patients from different backgrounds and ethnicities.
We are excited to see what this work will lead to in the future.
About the author: Dr. Tandon is the Director of Cardiovascular Innovation at Cleveland Clinic Children’s and Clinical Innovation Lead for the Pediatric Institute. He has a joint appointment in the Imaging Institute and in Biomedical Engineering at the Cleveland Clinic Lerner Research Institute. He is also Adjunct Assistant Professor in the Department of Biomedical Engineering at the Case School of Engineering at Case Western Reserve University.
References
Advertisement

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/2cd26dab-ecb5-4637-8975-7d6a7aaad600/22-CHP-3431758-Pediatric-2022-Year-in-review-footer-2-2_jpg)
Advertisement
Advertisement
A new CME opportunity in Chicago, May 15-16
Innovative hardware and AI algorithms aim to detect cardiovascular decline sooner
Experts advise thorough assessment of right ventricle and reinforcement of tricuspid valve
Reproducible technique uses native recipient tissue, avoiding risks of complex baffles
A reliable and reproducible alternative to conventional reimplantation and coronary unroofing
Program will support family-centered congenital heart disease care and staff educational opportunities
Case provides proof of concept, prevents need for future heart transplant
Pre and post-surgical CEEG in infants undergoing congenital heart surgery offers the potential for minimizing long-term neurodevelopmental injury