Case illustrates how easily condition can mimic preeclampsia
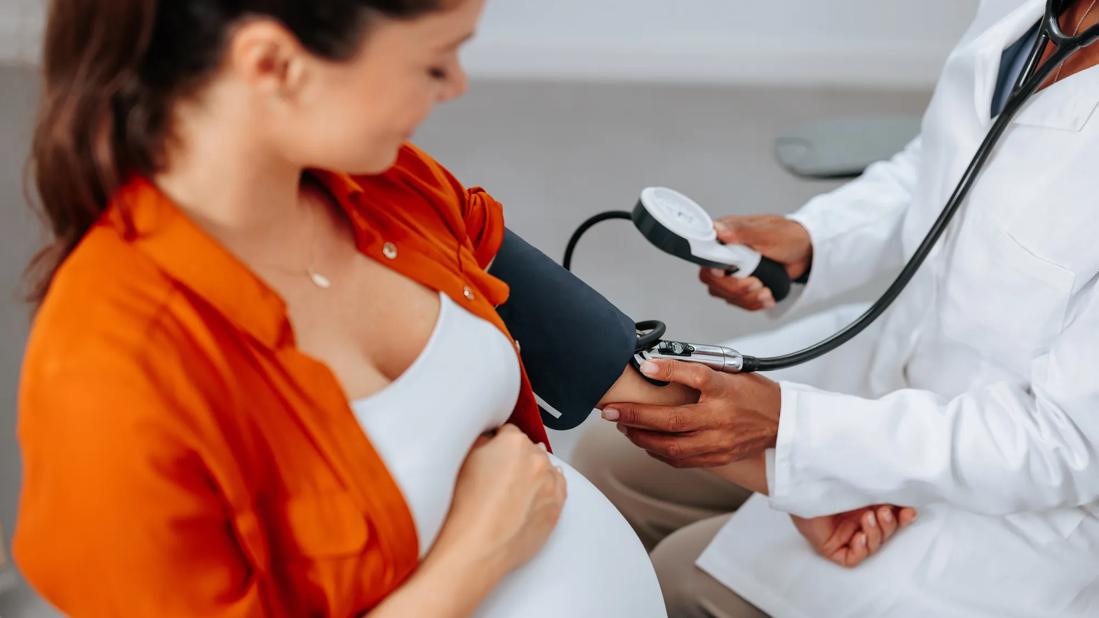
When an otherwise healthy patient in her 20s developed symptoms of severe hypertension 34 weeks into her third pregnancy, she was diagnosed with preeclampsia. An urgent C-section was performed and she delivered a healthy baby.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Six weeks later, however, the patient sought outpatient medical care for continued episodes of fluctuating high blood pressure along with headaches, palpitations and nausea. She had been prescribed twice-daily 100 mg labetalol, but it had little effect.
Although preeclampsia can emerge in the days and weeks postpartum, that diagnosis did not fully explain her symptoms. The patient’s care team ordered bloodwork. While awaiting results, the patient began to experience severe headache, tinnitus and blurry vision, and she presented to the emergency department.
Results of further lab tests included elevated plasma normetanephrine: 19,950 pg/mL (18–101 pg/mL) and norepinephrine: 13,752 pg/mL (80–520 pg/mL).
Magnetic resonance imaging (MRI) and a full-body positron emission tomography (PET) scan revealed multiple para-aortic and liver masses – one measuring 7.38 × 5.39 cm. The patient was diagnosed with metastatic paraganglioma (PGL). Genetic testing revealed a pathogenic variant of the SDHB gene, which is associated with PGL and a higher likelihood of metastases.
Pheochromocytoma (PCC) and PGL are rare neuroendocrine tumors that develop from chromaffin cells. Patients diagnosed with PCC/PGL are typically between age 30 and 50, although the diseases can present at any age. Malignancy occurs in 10% to 15% of cases.
The patient was referred to Cleveland Clinic, where her endocrine care was managed by Pratibha Rao, MD, MPH.
Dr. Rao underscores how easily a PGL diagnosis may be mistaken for preeclampsia. Preeclampsia is one of the most common complications of pregnancy, and PCC/PGL in pregnancy is rare; the incidence is estimated to be only one in 15,000-54,000 pregnancies.
Advertisement
“Our patient was young and seemingly healthy, and had had two prior conceptions with uncomplicated, term deliveries,” says Dr. Rao. “She had not expected any complication in her third pregnancy. She had no family history of pheochromocytoma or paraganglioma, but she turned out to be the index case.”
The case illustrates how easily PCC/PGL can be missed in the setting of pregnancy – beginning with the impracticality of screening every pregnant patient with hypertension. Yet the PCC/PGL in pregnancy presents significant risk.
Although Dr. Rao’s patient delivered a healthy baby and her symptoms were controlled during labor and delivery, good outcomes are far from guaranteed. The fetal mortality rate for untreated PCC/PGL is 29%. Surges in catecholamines can cause vasoconstriction resulting in uteroplacental insufficiency, placental abruption and fetal death. Maternal mortality in uncontrolled PCC/PGL also is 29%. Hypertensive crises can cause myocardial infarction, cardiomyopathy, arrhythmia and stroke.
With treatment, however, those risks can be reduced to about 12% and around 0%, respectively, so an accurate and timely diagnosis is crucial.
To improve the likelihood of identifying PCC/PGL in a pregnant patient, Dr. Rao highlights the importance of three tools:
Advertisement
“Paying close attention to symptomatology and good history-taking is very important,” says Dr. Rao. “If someone has palpitations, you definitely check the thyroid. But in the setting of hypertension with palpitations, headaches and diaphoresis, we should think of pheochromocytoma paraganglioma.”
If PCC/PGL is diagnosed in pregnancy, management depends upon an awareness of medications that can be delivered without risking a catecholamine surge and a hypertensive crisis, says Dr. Rao. Patients with PCC/PGL should receive alpha-adrenergic blockade treatment for a few days before a beta-adrenergic blockade is started.
Surgical removal of tumors may be feasible in the second trimester or may be postponed until after delivery.
In most cases, fetal delivery should be done via cesarean section to avoid higher risk of hypertensive crisis associated with vaginal delivery.
Finally, genetic testing should be performed on all patients with PCC/PGL so that risks associated with specific gene mutations can be assessed. The malignancy rate for pathogenic variants in SDHB is estimated at 50% to 90% in various studies.
Three years after her PGL diagnosis, the patient’s symptoms are well controlled with phenoxybenzamine, an alpha blocker and a beta blocker.
“Her Cleveland Clinic endocrine surgeon had offered her surgical option, but the patient declined because she was feeling well at the time,” says Dr. Rao.
With the known genetic mutation, continued monitoring is essential. That includes a 24-hour urine and/or plasma metanephrine testing annually as well as imaging every two years, or sooner if symptoms emerge.
Advertisement
“We would scan the base of the skull, including the neck, so we can monitor the paraganglioma, as well as the chest, abdomen and pelvis,” says Dr. Rao. “To reduce radiation exposure, every two to three years we would alternate MRI and CT scans.”
There are numerous functional imaging modalities that can be used, says Dr. Rao: 123I-MIBG, 18F-DOPA PET, 18F-FDG PET and 68Ga-DOTATATE PET-CT.
“We would have an expert, multi-disciplinary team discuss optimal treatment options and take the patient’s preferences into consideration,” she adds. “Typically, with any neuroendocrine tumors, resection of metastatic lesions is considered to reduce tumor burden, even the primary cancer has not been identified. Targeted radiotherapy or radiofrequency ablation of the liver also could be considered.”
Advertisement
Advertisement

Awareness of this symptom manifestation can reduce risk

Biomarkers can predict who is at risk for severe disease

Specially appointed room serves as safe space for families
Reproductive health specialists discuss tough-case abortion care

Prescribing eye drops is complicated by unknown risk of fetotoxicity and lack of clinical evidence

Rare pregnancy complication can lead to fetal demise

Research may offer family-planning insights for those with the condition

Largest study examines factors affecting asthma exacerbations during and after pregnancy