Clinically significant lesions detected in nearly half of patients with no lesions on 3T MRI
In the largest study to date assessing the value of in vivo structural 7-tesla (7T) MRI for epilepsy presurgical evaluation, 7T MRI revealed subtle focal cortical dysplasia in about half of patients who had no lesions detected by 3T MRI; moreover, complete resection of these lesions was significantly associated with postoperative seizure freedom. The study’s findings were reported in a Dec. 7 platform presentation at the American Epilepsy Society’s 2019 annual meeting.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Information gleaned from the superior resolution of 7T MRI can lead to better outcomes in patients with focal epilepsy who do not have apparent lesions seen on 3T MRI,” says lead author and Cleveland Clinic Epilepsy Center staff scientist Irene Wang, PhD, who presented the study results.
Although 7T MRI was first approved by the FDA for clinical diagnostic use in October 2017, Cleveland Clinic had used its 7T MRI system for research purposes starting in 2014. 7T field strength offers increased signal-to-noise and contrast-to-noise ratios, resulting in sharper images with potentially better detection and visualization of cortical malformations.
“Because of the expense of 7T MRI scanners and the short time they have been used clinically, data assessing their utility are especially important,” Dr. Wang observes.
To that end, between 2014 and 2018 Dr. Wang and colleagues prospectively selected 100 patients with focal drug-resistant epilepsy seen at Cleveland Clinic to undergo 7T MRI. All were also assessed with 3T MRI.
Post-processing of the 7T T1-weighted MP2RAGE sequence was done using the morphometric analysis program (MAP), with images compared to a database of 7T MRI images obtained from 50 healthy controls. In addition to studying 7T MRI in the largest cohort of epilepsy patients to date, this investigation represents the first report of MAP post-processing of images from a 7T MRI scanner (more information on MAP can be found here).
7T images were reviewed by an experienced board-certified neuroradiologist, and the clinical significance of 7T findings was evaluated in terms of overlap with ictal onset as indicated by intracranial EEG (ICEEG) as well as surgical findings, postoperative seizure outcomes and histopathology.
Advertisement
Key findings included the following:
Dr. Wang expects the full study results to be published in 2020.
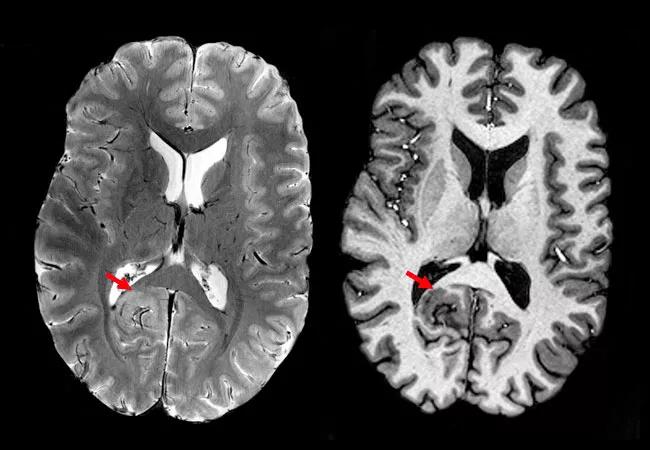
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/1c698216-a471-4dfd-aafa-f4a95c1a8112/19-NEU-6520-Wang-7T-study-at-AES_CQD-650x450_Hero_1_jpg)
Figure 1. 7T images from a patient whose 3T MRI revealed no epileptogenic lesion. With the increased signal-to-noise and contrast-to-noise ratios of 7T, small focal cortical dysplasia with thickened cortex was seen at the depth of the right parieto-occipital sulcus (arrows). Detection of this lesion played a crucial role in the patient’s presurgical evaluation.
Advertisement
According to Dr. Wang, the Cleveland Clinic experience demonstrates that 7T MRI can play an important role in epilepsy presurgical evaluation.
“Findings from 7T MRI and MAP guidance, when consistent with a patient’s electro-clinical profile, should be incorporated into plans for ICEEG implantation and resective or ablative surgery,” concludes Dr. Wang. “7T MRI could particularly benefit patients with drug-resistant epilepsy without lesional findings on 3T MRI.”
She adds that the Cleveland Clinic team will next be focusing on making 7T sequences more efficient in order to reduce scan time. The team also intends to better adapt MRI post-processing techniques to 7T images in order to further increase the yield for detection of focal cortical dysplasia.
Advertisement
Advertisement

Aim is for use with clinician oversight to make screening safer and more efficient

Rapid innovation is shaping the deep brain stimulation landscape

Study shows short-term behavioral training can yield objective and subjective gains

How we’re efficiently educating patients and care partners about treatment goals, logistics, risks and benefits

An expert’s take on evolving challenges, treatments and responsibilities through early adulthood

Comorbidities and medical complexity underlie far more deaths than SUDEP does

Novel Cleveland Clinic project is fueled by a $1 million NIH grant

Tool helps patients understand when to ask for help