Insights from our Neurological Institute’s expanded use of the technology
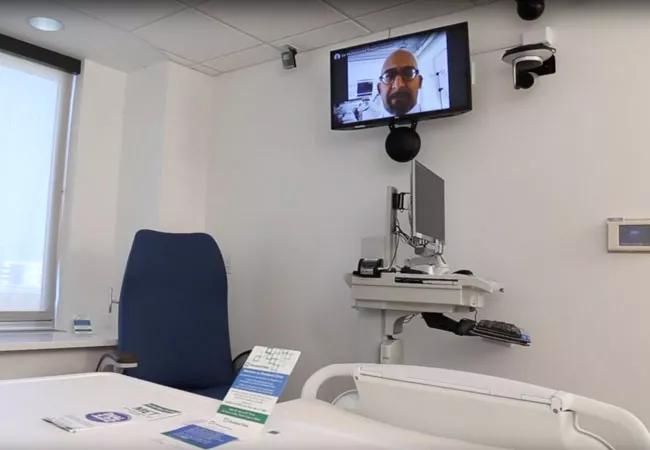
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/321b9a48-c750-4182-b3cc-9c23ad68771e/20-NEU-1876104-NI-virtual-rounding-covid-hero_650x450_jpg)
20-NEU-1876104-NI-virtual-rounding-covid-hero_650x450
While reports abound about how the COVID-19 pandemic is fueling a surge in virtual outpatient visits, it’s likewise accelerating the adoption and evolution of telemedicine use in inpatient settings.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“This public health crisis has given us a crash course in using telemedicine technology within the hospital,” says Imad Najm, MD, Vice Chair of Cleveland Clinic’s Neurological Institute and Director of its Epilepsy Center. “We are learning quite a bit, which we hope will allow us to make even better use of this technology in our routine care of hospitalized patients after the crisis is over.”
Cleveland Clinic’s Neurological Institute is no newcomer to telemedicine. It was among the nation’s early adopters of telestroke technology, which it has offered since 2011 via the Cleveland Clinic Telestroke Network, comprising hospitals within the Cleveland Clinic health system as well as external facilities in Ohio, Pennsylvania and Florida. It has likewise become a national leader in outpatient subspecialty teleneurology visits.
The Neurological Institute has also led the charge within Cleveland Clinic when it comes to telemedicine in inpatient settings. The centerpiece of its efforts is a neurological stepdown unit featuring hardwired telemedicine capabilities in each of the unit’s 17 patient rooms. Each room features a TV with a high-definition web camera, microphone and speaker to allow providers to do face-to-face video conferences and evaluations with patients from anywhere via phone, tablet or computer (see photos at top of post and below). Using their remote device, providers can move the camera to the right or left or zoom in or out as needed for evaluation.
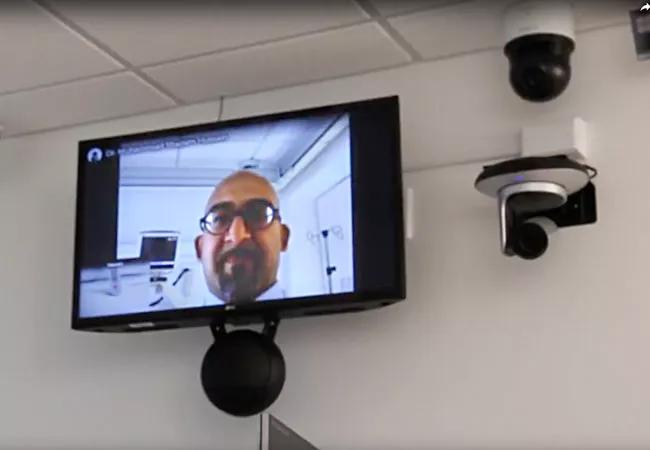
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/b238493a-1046-420c-a1c0-969b74c2c236/20-NEU-1876104-NI-virtual-rounding-covid-hero-close_650x450_jpg)
Photo showing key equipment components in a telemedicine-hardwired room on the neurological stepdown unit.
Advertisement
“Because this is a neuro stepdown unit, we put a priority on high-definition zoom capability to ensure the ability to do things like see patients’ pupils and assess gaze,” explains Neurological Institute Telemedicine Manager Dana Collins, MBA, who oversaw the unit’s technological upgrade.
The enhanced stepdown unit, which opened on Cleveland Clinic’s main campus in July 2019, is notable in that it provides these virtual evaluation capabilities for patients across multiple subspecialty areas in addition to stroke, which has been the mainstay application for inpatient telemedicine in neurological care. For instance, the unit includes four epilepsy monitoring beds, and each room is equipped with epilepsy monitoring units to track patients’ brain activity and video equipment to record movements during a seizure. The video and telemedicine equipment also provide the treating physician with patient data in real time.
Prior to the COVID-19 pandemic, the Neurological Institute supplemented the hardwired equipment on this unit with mobile telemedicine carts from the same vendor. These carts — complete with touchscreen interface, high-definition camera, speaker and microphone (see photos below) — provide essentially the same face-to-face video evaluation capabilities, says Collins, but with the added benefit of mobility.
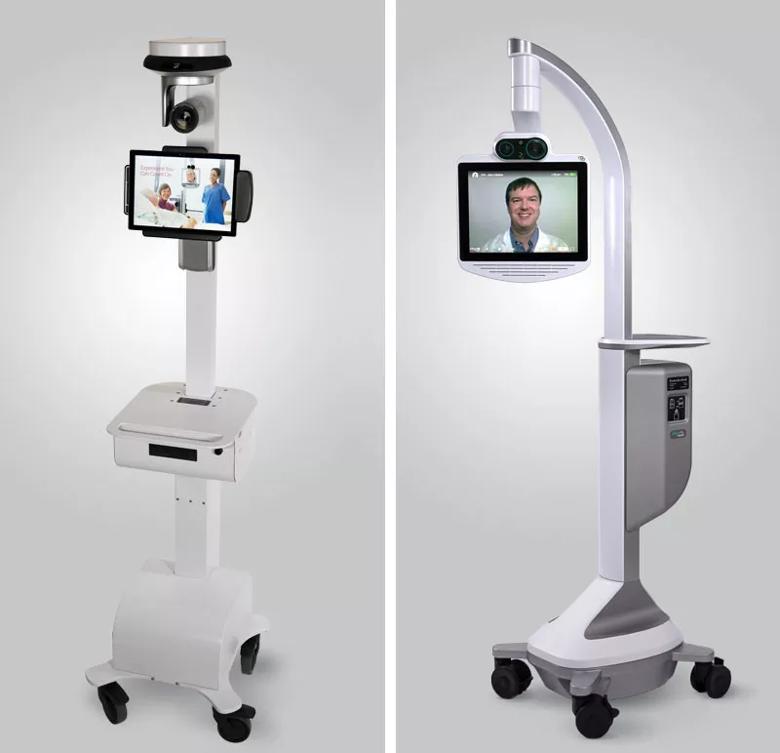
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/ddb338c5-983a-4f29-84cf-ad6958e43888/20-NEU-1876104-NI-use-of-virtual-rounding-covid-Inset_800x772_jpg)
Two types of robot carts used for Cleveland Clinic’s inpatient telemedicine. The cart on the left is used in various inpatient units, while the cart of the right is used in emergency departments. Photos courtesy of InTouch Health.
Advertisement
Before the pandemic, the Neurological Institute had 17 of these carts deployed across various Cleveland Clinic health system hospitals — mostly in emergency departments, with a few used to provide neurologist coverage at select times at a few regional hospitals, plus one in the neurological ICU.
“Our goal in expanding telemedicine has been to provide patients with access to Cleveland Clinic physicians and experts at any time, wherever they are,” notes Dr. Najm. “This objective preceded the pandemic.”
But as COVID-19 began to emerge in the U.S., the objective gained increased urgency and a broader rationale: maintaining access to care for Neurological Institute patients while protecting patients and providers from the bidirectional risk of virus transmission.
In response, Collins swung into action, ordering six additional mobile telemedicine carts in early March and six more shortly thereafter. Starting on March 16, new carts were deployed in locations including the adult and pediatric epilepsy monitoring units, several neurosurgery units, and next to the CT scanner where stroke patients are evaluated on Cleveland Clinic’s main campus. Others are being used to provide backup teleneurology coverage at regional hospitals.
Collins’ team swiftly trained over 130 additional Neurological Institute providers in how to use their phones and other devices to interact with patients via the telemedicine carts. Newly onboarded caregivers included those in the brain tumor, neurosurgery, and adult and pediatric epilepsy groups. Training has been given to providers ranging from physicians and surgeons to fellows and residents to advanced practice providers and social workers.
Advertisement
The technology and training has allowed care teams to virtually round on neurological inpatients without losing face-to-face contact — but while protecting patients and caregivers from risk of virus transmission. Typically one caregiver — usually a nurse or advanced practice provider caring for the patient — is with the patient during the virtual rounding or evaluation, to help with aspects of a neurological exam, for example. But the presence of the cart allows a host of other caregivers to visit with the patient as well, from the rounding staff physician to trainees, social workers and others.
“That’s part of the beauty of this approach — it can be very multidisciplinary,” says Dr. Najm, who has used this virtual rounding extensively in recent weeks. “When needed, we can bring together a team to collectively see a patient and discuss the care plan together, regardless of where the team members physically are.”
Dr. Najm and Collins identify a number of additional benefits of this deployment of inpatient telemedicine. Some are specific to the COVID-19 pandemic, such as the reduced bidirectional risk of virus transmission due to fewer in-person contacts between providers and inpatients. This, in turn, can help ensure adequate caregiver staffing during the pandemic by reducing chances that providers will be infected or need to self-quarantine. Another benefit is the reduced need for personal protective equipment with less direct patient-to-provider contact.
Other benefits predated the pandemic and will continue after it. These include:
Advertisement
Dr. Najm says he’s been struck by how well patients of all ages and backgrounds have embraced the telemedicine approach, particularly during the pandemic. “The patients I’ve seen have been extremely open to this,” he says. “They too are really concerned about exposure to the virus from healthcare workers, and they seem to like the access to their providers.”
At the same time, he acknowledges that telemedicine has its shortcomings, including the loss of the ability to touch the patient and occasional technical challenges, such as when the screen isn’t large enough for a patient to see all the team members who may be assembled on the other end of the video connection or the very rare glitch in internet connectivity.
These are the types of challenges that Collins, Dr. Najm and their colleagues will consider when they assess their expanded use of inpatient telemedicine after the pandemic eases. But both Collins and Dr. Najm are bullish on the future of this technology in neurological care.
“I think our ramp-up of telemedicine in response to COVID-19 will spur an awakening to the potential of this technology — and that’s exciting,” says Collins.
“Although this pandemic has been an undeniably tragic crisis,” notes Dr. Najm, “it may have one silver lining. It is likely to push us, as a community, to further adopt and refine this technology that can serve us well for decades to come. This pandemic may well make this a mainstream technology from which patients all over the world can benefit. That would be a silver lining we can all hope for.”
Dr. Najm can be contacted at najmi@ccf.org.
Advertisement
Patients report improved sense of smell and taste
Clinicians who are accustomed to uncertainty can do well by patients
Unique skin changes can occur after infection or vaccine
Cleveland Clinic analysis suggests that obtaining care for the virus might reveal a previously undiagnosed condition
As the pandemic evolves, rheumatologists must continue to be mindful of most vulnerable patients
Early results suggest positive outcomes from COVID-19 PrEP treatment
Could the virus have caused the condition or triggered previously undiagnosed disease?
Five categories of cutaneous abnormalities are associated with COVID-19