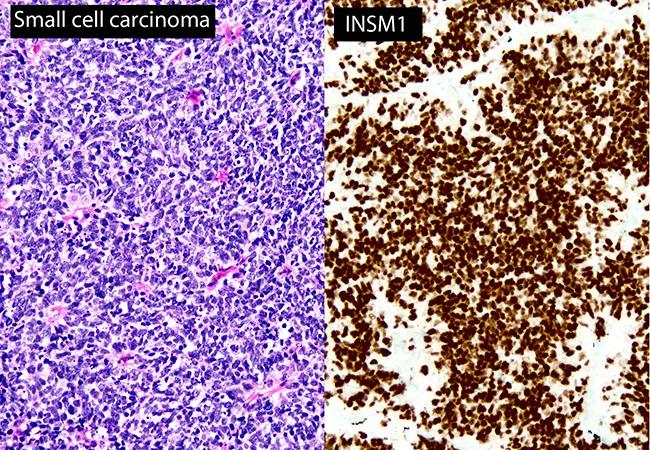
Largest series shows marker sensitive, highly specific
By Sanjay Mukhopadhyay, MD, Josephine Dermawan, MD, PhD, and Carol Farver, MD
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Neuroendocrine tumors of the lung range from low-grade malignancies (carcinoid tumors) to aggressive forms of lung cancer (small-cell lung carcinoma and large-cell neuroendocrine carcinoma). Accurate pathologic diagnosis of these tumors is essential because treatment and outcomes vary significantly depending on the precise diagnostic label. In order to diagnose this group of tumors, pathologists often rely on immunohistochemical markers of neuroendocrine differentiation (synaptophysin, chromogranin and CD56). These markers stain either the cytoplasm or the membrane of the tumor cells. Since none of these markers are perfectly sensitive or specific, there is a need for alternative markers to improve diagnosis.
In recent years, a new marker known as insulinoma-associated protein 1 (INSM1) has emerged as a potential addition to the armamentarium of the diagnostic pathologist. In contrast to traditional neuroendocrine markers, INSM1 stains the nucleus of tumor cells. Since there is only limited information regarding this marker in lung cancers (based mainly on tissue microarray data), our research team tested its performance in a wide variety of lung cancers and benign lung lesions using real-life samples, including whole-tissue sections of resected tumors, and small biopsies. We presented our findings in a platform presentation at the 2018 Annual Meeting of the United States and Canadian Academy of Pathology.
We stained 400 lung lesions with INSM1 (A8, Santa Cruz), including 60 small-cell lung carcinomas, 45 typical carcinoid tumors, 16 atypical carcinoid tumors, 24 large-cell neuroendocrine carcinomas, 130 adenocarcinomas, 33 squamous cell carcinoma and many other tumor types that had not been previously tested. We also stained benign lesions whose INSM1 status was previously unknown (20 carcinoid tumorlets and 30 meningothelial-like nodules). The samples tested included 347 resections, 38 biopsies and 15 tissue microarrays. For comparison, the same cases were stained with the traditional neuroendocrine markers synaptophysin, chromogranin and CD56.
Advertisement
INSM1 was positive in 59/60 (98 percent) small cell lung carcinomas, 45/45 typical carcinoid tumors (100 percent), 15/16 atypical carcinoid tumors (94 percent) and 18/24 large cell neuroendocrine carcinomas (75 percent). INSM1 expression was very uncommon in non-neuroendocrine tumors such as adenocarcinoma (4/130, 3 percent) and squamous cell carcinoma (1/33, 3 percent). For small-cell lung carcinoma, the sensitivity of INSM1 was comparable to the sensitivity of synaptophysin (100 percent) and CD56 (95 percent), and higher than the sensitivity of chromogranin (82 percent). Overall specificity for neuroendocrine differentiation was 97 percent for INSM1, 91 percent for synaptophysin, 98 percent for chromogranin and 86 percent for CD56. All carcinoid tumorlets of the lung were positive for INSM1, and all meningothelial-like nodules were negative.
This study is currently the largest series of lung lesions tested with INSM1. It shows that INSM1 is sensitive and highly specific for the diagnosis of neuroendocrine tumors of the lung, including small cell lung carcinoma.
Advertisement
Advertisement

Screen patients seeking care for chlamydia, gonorrhea
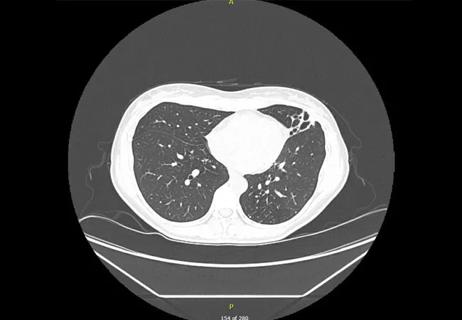
Lingulectomy removes infection when antibiotics fail

Researchers have developed immunoprofiles for an emerging disease with a mortality rate as high as 27%

Findings from one of the first published case series
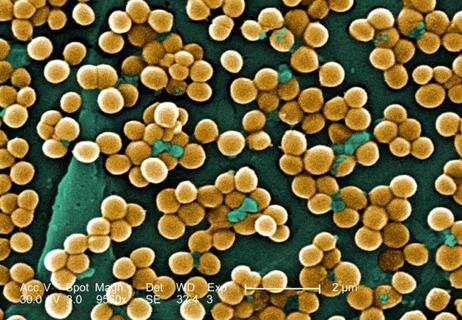
Don't discount this crucial step
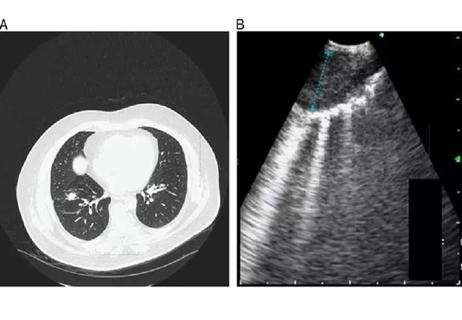
EBUS-TBNA found safe and effective
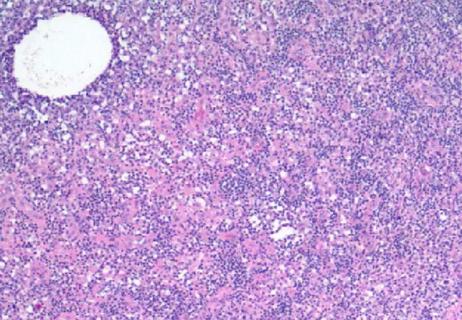
How to spot the rare infection
Not all lung nodules are malignant