More on the procedure and the institutional experience
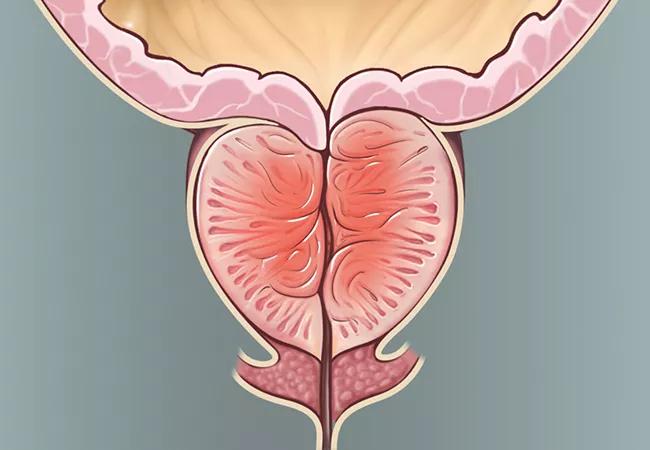
BPH, or benign prostatic hyperplasia, causes enlargement of the prostate and is the most common prostate issue for men, affecting the majority as they age.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Common symptoms include difficult urination and incontinence. Without treatment, BPH can result in further blockage of the urethra and worsening symptoms, such as urinary tract infections, bladder stones, blood in urine and kidney damage.
There are currently a variety of treatment options for this condition, including medications and surgery. Water jet ablation, also known as Aquablation® — a minimally invasive modality that received FDA clearance in 2017 — has been gaining momentum in recent years. This approach has shown to provide long-term relief, even among men with larger prostates, with a low rate of complications.
“This procedure is indicated for men with BPH who require more than medication to relieve their lower urinary tract symptoms,” says Dennis Bentley, MD, Department of Urology. “It’s designed to remove tissue with fewer side effects because everything is mapped out with an ultrasound and important structures are maintained."
Dr. Bentley, alongside his colleague Brian Canterbury, MD, spearheaded efforts at Cleveland Clinic to integrate this procedure into clinical practice. To date, they have collectively performed water jet ablation on more than 80 BPH patients.
This resective procedure uses a heat-free waterjet that is controlled by robotic technology to remove the prostate tissue causing lower urinary tract symptoms in men with BPH.
Water jet ablation, which is indicated for prostates of any size and shape, combines a cystoscope with ultrasound imaging. This allows the surgeon to see the entire prostate in real time, enhancing the precision of the procedure.
Advertisement
Patients undergo an initial evaluation to assess the size and shape of the prostate as well as urine flow, explains Dr. Bentley.
“The procedure is either done under general or spinal anesthetic,” says Dr. Bentley. “Unlike any other BPH-related surgery, water jet ablation is an image-guided procedure allowing for increased precision and ensuring all of the important structures, such as the sphincter muscle, bladder, and ejaculatory ducts, are identified and maintained.
“Additionally, there is no heat dissipation since this procedure uses a waterjet,” he continues.
There is limited downtime for patients who undergo this procedure, according to Dr. Bentley, who notes that bleeding is expected for a short period of time and there is the possibility of a urinary tract infection.
“However, the typical complications of urine leakage, retrograde ejaculation problems with erection, and erectile dysfunction are much lower with water jet ablation than with other treatments,” he says. “Specifically, this approach enables us to map out and maintain ejaculatory function for patients.”
Compared with medications and other minimally invasive treatments that don’t remove tissue, BPH patients who receive water jet ablation have much better long-term symptom control due to the resective nature of this procedure.
“This minimally invasive procedure is safe with long-term durability and a low-side effect profile,” Dr. Bentley says, while noting that water jet ablation should be considered for BPH patients who fail medication or those who prefer a surgical approach. “This procedure is also an option for men with larger prostates who might not be candidates for more traditional approaches that have size limitations.”
Advertisement
Water jet ablation has been available at Cleveland Clinic since early 2023, and a growing number of patients continue to benefit from the procedure. Given the positive outcomes to date, there are plans to expand its use and availability across the network.
After the procedure, Dr. Bentley typically conducts follow-up visits at two and six weeks. At that time, urine flow is evaluated and compared to pre-procedure assessments. Additionally, the American Urological Association (AUA) symptom score is also measured.
“The outcomes we have observed so far have been excellent,” Dr. Bentley notes. “There has been a marked improvement in urine flow and more than a 16-point reduction in AUA symptom score. This procedure has also resulted in a definite preservation of sexual function for our patients.”
Advertisement
Advertisement

Medical management remains the starting point for most symptomatic patients seeking treatment
Review the advantages and disadvantages of newer interventions

Applications, outcomes and untapped potential

Transperineal ultrasound a viable, non-invasive option for monitoring intra-fractional prostate motion

Using novel robotic approaches for a difficult-to-access prostate

Pediatric urologists lead quality improvement initiative, author systemwide guideline

Fixed-dose single-pill combinations and future therapies

Reproductive urologists publish a contemporary review to guide practice