Fibromyalgia and headache/migraine are the best-supported applications
The atypical antipsychotic (AA) olanzapine is a promising adjunctive agent for the management of certain types of chronic pain, according to the most comprehensive review of the subject to date. “The evidence is preliminary, but it is consistent,” reports psychiatrist Xavier Jimenez, MD, Medical Director of Cleveland Clinic’s Chronic Pain Rehabilitation Program, who conducted the systematic review with two colleagues.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Opioids are the first-line treatment for pain syndromes, but their long-term use is not associated with efficacy, and there is a risk of significant side effects,” says Dr. Jimenez, who also serves as Director of the Chronic Pain Rehabilitation Section in Cleveland Clinic’s Center for Neurological Restoration. “Thus, we chose to look at the AA class of medications, which haven’t been widely researched for chronic pain but have been used for decades as adjunctive, off-label therapies.”
In the systematic review, published in the Clinical Journal of Pain, the Cleveland Clinic team reviewed 20 published studies of five AAs: aripiprazole, olanzapine, quetiapine, risperidone and ziprasidone.
The best-studied AA was olanzapine, for which there were 11 studies, including one randomized, controlled trial. “These studies showed that olanzapine has efficacy in chronic pain syndromes characterized by central sensitization and/or psychiatric comorbidities, such as fibromyalgia and headache/migraine,” Dr. Jimenez notes.
The team also found six low-quality studies of quetiapine, half of which showed efficacy in pain syndromes (typically headache/migraine). There was little evidence for the other three AAs in chronic pain conditions, largely due to restricted sample sizes and/or a lack of a robust study design.
Although it is unclear whether AAs have intrinsic analgesic properties, they appear to relieve pain through a variety of mechanisms, Dr. Jimenez says.
For instance, the drugs demonstrate receptor heterogeneity, touching on dopaminergic, histamine, adrenergic and serotonergic receptors (among others) in a way similar to tricyclic antidepressants, which have long been shown to be effective in managing chronic pain. AAs also appear to reduce central sensitization, particularly in pain-processing areas of the brain such as paralimbic structures. Additionally, the AAs’ established efficacy in managing psychiatric disorders that often co-occur with chronic pain conditions (e.g., anxiety, depression, insomnia) may also contribute indirectly to pain relief.
Advertisement
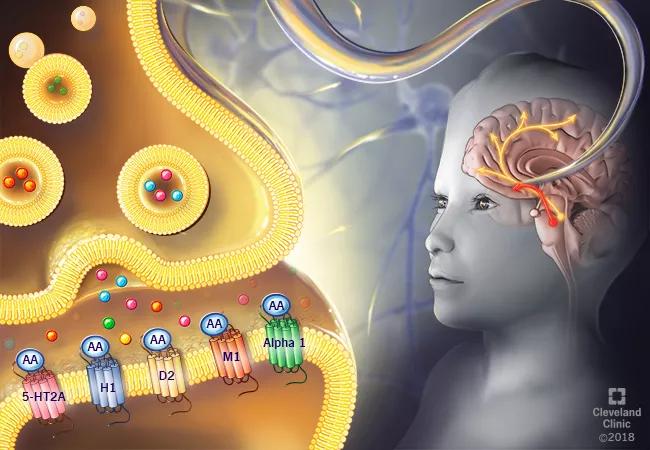
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/70502552-5e25-4742-b224-bf9df790fbcf/AAs_ChronicPain_135629_650x450_wLabels_jpg)
Atypical antipsychotics (AAs) feature receptor heterogeneity in the central nervous system (CNS) and likely impact central sensitization and chronic pain syndromes through their action on CNS areas such as mesolimbic and mesocortical pathways as well as the pain neuromatrix in general.
AAs offer many advantages over opioids, according to Dr. Jimenez, most notably a lack of addictive and abuse potential. Since they are not controlled substances, there is no state-level prescription drug-monitoring requirement. AAs tend to act rapidly, in contrast to tricyclic antidepressants and serotonin-norepinephrine reuptake inhibitors, which can take weeks to improve symptoms. They also don’t contribute to worsening pain or central sensitization, and of course they can treat psychiatric comorbidities.
Disadvantages of AAs are their side effects — including sedation, weight gain, metabolic effects and cardiac QTc prolongation — which require monitoring. “When compared with opioids’ risks of addiction or overdose, however, the medical monitoring with AAs can be a much better tradeoff,” says Dr. Jimenez. Additionally, there is stigma attached to use of AAs, given their primary labeling for treatment of schizophrenia and bipolar disorder.
Dr. Jimenez offers the following advice to clinicians for use of AAs in chronic pain syndromes:
Advertisement
Despite the potential utility of AAs, Dr. Jimenez reports that he is not aware of any ongoing pharma-sponsored trials of AAs for chronic pain conditions, and he notes that his systematic review was funded internally by Cleveland Clinic.
“Still, there is potential for AAs,” he says, adding that they may ultimately be shown to have additional applications for conditions such as chronic back pain, whiplash, diabetic neuropathy, musculoskeletal pain, postherpetic neuralgia and cancer pain.
Advertisement
Advertisement
Despite safety concerns and mixed trial results, experts see potential for this indication
Experts endorse a push to improve prevention and treatment following repetitive head injury
A population with very high lifetime risk presents care challenges and pathophysiologic insights
Two Cleveland Clinic neurologists review biomarker advances, targeted therapies and unresolved clinical challenges
Data-driven segmentation approach shows promise for seizure characterization with utility for clinical decision making
Alzheimer’s studies delve into preventing and modifying the disease’s trajectory and impact
Study finds broadly similar outcomes between MIS and open surgical approaches
System uses clinical data routinely collected at clinical visits