Study assesses utility of patient-reported outcomes measures in uveitis and scleritis
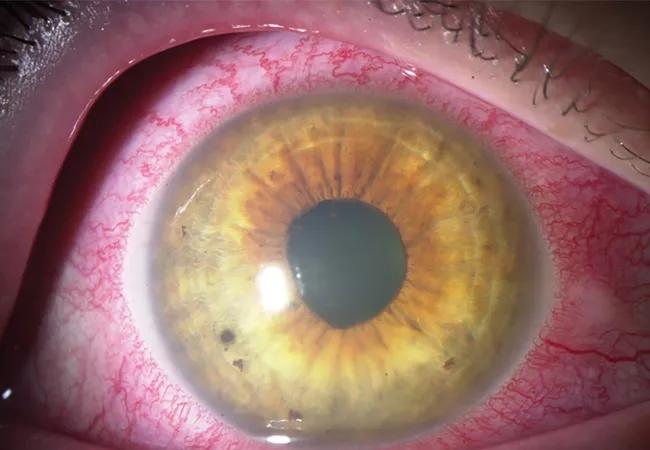
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/609df357-2906-4366-8cc9-09ab719a0914/16-RHE-1503-Hajj-Ali-Hero-Image-650x450pxl_jpg)
Redness in the eye caused by anterior chamber inflammation
Uveitis is a potentially blinding inflammatory eye disease (IED) that requires close interdisciplinary care, with ophthalmologists assessing disease activity and rheumatologists adjusting systemic, potentially toxic, therapies based on exam findings visualized by ophthalmologists. Patient reported outcomes measurement information systems (PROMIS) may aid in medical decision-making in IED, according to the results of a study presented at the 2019 American College of Rheumatology Annual Meeting, which was held November 8-13 in Atlanta.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“PROMIS data have been used to influence medical decision making in other chronic medical conditions, including rheumatic diseases,” says Sunil Srivastava, MD, an ophthalmologist in Cleveland Clinic’s Cole Eye Institute. “However, their utility has not been assessed in patients with inflammatory eye disease.”
The study included 87 patients with a diagnosis of uveitis (N = 74) or scleritis (N = 13), who were seen two or more times by specialists in IED over a 30-month period, and for whom PROMIS data was collected within two weeks of ophthalmologic exam. Demographics and disease characteristics were documented for each patient’s initial and each subsequent encounter.
There were no statistically significant differences in PROMIS scores in patients with uveitis vs scleritis, nor in patients on biologic vs nonbiologic therapies. Extent of anterior chamber inflammation negatively correlated with physical health PROMIS scores. The presence of vascular leakage on fluorescein angiography was associated with worse physical health PROMIS scores at 1-year follow-up, though the association was not seen at other time points.
“We evaluated the use of PROMIS data in tracking ocular disease activity and response to therapy in patients with IED in an effort to better understand the patient experience between office visits,” says first author Joshua Hedrick, MD, a rheumatologist who practices at Cleveland Clinic Florida. “Our evaluation did find some significance to patients perceiving their physical health to be worse when inflammation was seen in the anterior chamber of the eye on assessment by ophthalmology. This may be because anterior chamber inflammation is sometimes associated with redness in the eye. Patients can see for this symptom themselves, thus resulting in the perception that their health is worse.”
Advertisement
Treating IED is of utmost importance to prevent blindness and complications of a systemic rheumatic disease when present, according to Rula Hajj-Ali, MD, a rheumatologist in the Center for Vasculitis Care and Research and a co-author author on the study. Uveitis has been listed as the cause of blindness in 10% of cases of blindness in the western world. Additionally, Dr. Hajj-Ali notes, “ocular disease can be the first manifestation of multiple diseases and can potentially lead to a systemic diagnosis.”
“Through this pilot project, we found correlation between PROMIS data and some aspects of IED. Our findings validate patient symptoms in anterior uveitis and will enhance our understanding and recording of disease activity among patients,” Dr. Hajj-Ali says.
Additional, larger studies are warranted to further investigate how PROMIS data can assist in monitoring ocular disease activity outside the exam room, according to the authors.
Uveitis is characterized by inflammation of the uvea and is anatomically classified into anterior, intermediate, posterior and panuveitic types. Uveitis has a variety of etiologies, including infections, systemic inflammatory conditions and autoimmune inflammatory disease confined to the eyes. Although 30-40% of uveitis patients have an associated systemic immune-mediated disease, a large number of uveitis cases do not fit into any well-defined diagnostic category and are labeled idiopathic with no etiology.
Rheumatologists most commonly see uveitis in patients with ankylosing spondylitis, juvenile rheumatoid arthritis, Behçet’s disease and any of the HLA B-27 associated seronegative spondyloarthropathies. Even for patients without a systemic inflammatory diagnosis, co-management with rheumatology is of high importance to manage the very aggressive immunosuppressive agents sometimes required to prevent vision loss.
Advertisement
At Cleveland Clinic, a multidisciplinary team composed of rheumatologists and ophthalmologists has facilitated a fast-track approach to evaluate and treat these patients in a timely manner to prevent vision loss. Utilizing this team-based approach allows advanced evaluations and treatment plans for these complex patients. This established relationship between the team members has led to accurate ocular and systemic diagnoses, which can facilitate favorable outcomes.
Advertisement
Advertisement
The drug does not provide lasting disease control for most patients
New service for patients with diabetes will make annual screening more convenient
Gonioscopy can help determine next steps in reducing IOP
Similarly, patients with noninfectious uveitis have a higher risk of being diagnosed with an autoimmune disease within five years
A review of pathophysiology, risk factors, clinical presentation and treatment options
How computational tools and personalized biomechanics can improve keratoconus detection, ectasia risk assessment and surgical outcomes
Motion-tracking Brillouin microscopy pinpoints corneal weakness in the anterior stroma
Registry data highlight visual gains in patients with legal blindness