Interventional pain management when conservative measures fail
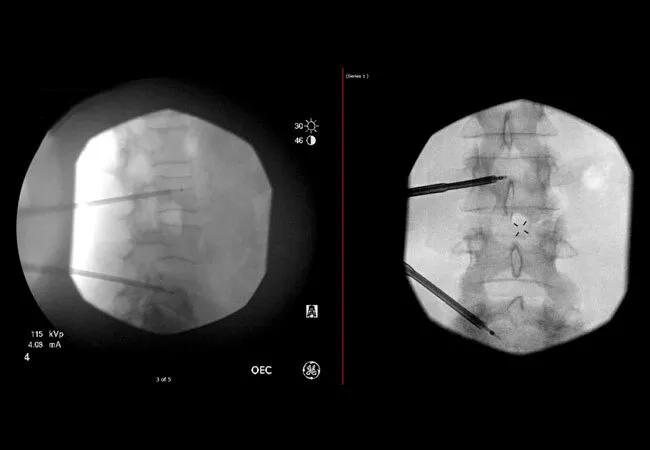
A 50-year-old woman with metastatic small cell lung cancer was referred to Cleveland Clinic’s Department of Pain Management in July 2019 with low and midback pain radiating to the right knee. She had been working with Kyle Neale, DO, staff in Cleveland Clinic Cancer Center’s Department of Palliative & Supportive Care, on pain control, but had failed palliative radiotherapy. MS contin, duloxetine and gabapentin offered some pain relief, but side effects left the patient unable to perform her daily functions.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Dr. Neale referred her to Sherif Costandi, MD, an interventional pain management specialist, for more effective treatment options. Lytic lesions had infiltrated her spine at L3 and L5. Dr. Costandi treated her with cooled radiofrequency ablation therapy (cRFA) to the affected vertebrae coupled with cementoplasty to stabilize the area using the same bone access channel. “She had been in pain for about six months, and our best noninterventional efforts hadn’t worked,” says Dr. Costandi. “We were able to drop her pain from an 8 or 9 out of 10 to a zero and improve her quality of life dramatically.”
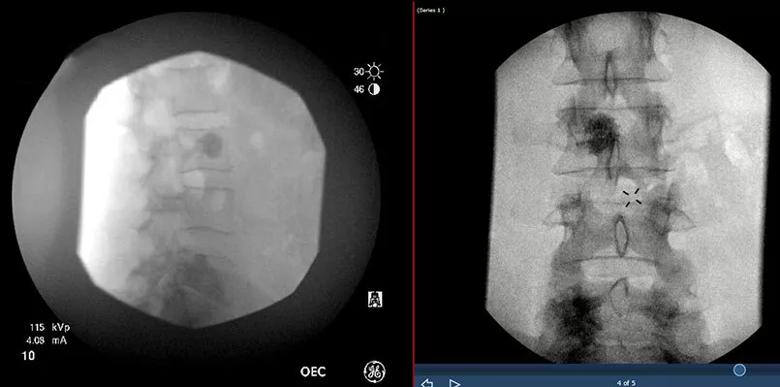
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/85607b70-30c5-4998-bcc3-68df2b14ba1a/20-PAI-2027862_Costandi_Correct_2-805x399-1-1_jpg)
Antero-posterior and lateral images of cooled radiofrequency ablation and cementoplasty of spinal metastases after pulling out the instruments.
Patients with isolated, painful spinal lesions can benefit from cRFA, a technique currently used for liver metastases that has been adapted for spine care. This unique approach is performed under deep sedation, and the cooling function increases the diameter of the ablation. Because cRFA causes necrosis, the cavity is filled with polymethylmethacrylate bone cement to prevent any potential fragility. Multiple studies have shown significant pain relief for patients treated with cRFA and subsequent bone augmentation.
Bone invasion occurs in 60% to 80% of patients with metastatic cancer and can significantly impact daily function, mental health and overall quality of life. “It’s really important to get ahead of fractures and other skeletal events for these patients, especially those with issues in axial loading areas, and to stabilize any existing issues,” says Dr. Costandi.
Advertisement
“This is a relatively new approach, but in the Cleveland Clinic’s pain management program we strive to offer our patient population the most innovative techniques for treating intractable pain,” Dr. Costandi continues. “I am continuing to learn and train more novel techniques to pursue my passion for helping cancer patients experience pain relief.”
Cleveland Clinic’s Department of Pain Management offers many safe, proven, effective treatments designed to eliminate or reduce chronic pain to more than 13,000 new patients each year. Its fellowship-trained specialists educate future specialists while researching and treating patients with the most effective and innovative conservative and interventional pain management techniques.
For palliative medicine specialists, working closely with interventional pain specialists allows them to offer their patients the widest range of supportive care. “For many of these patients with severely metastasized cancer, we can help them through other measures, from standard pharmacotherapy to palliative radiotherapy with hyperthermia,” says Dr. Neale. “For other patients, more intervention is necessary, and at Cleveland Clinic Cancer Center, we are fortunate to have easy access to specialists in these minimally invasive procedures.”
Advertisement
Advertisement

Researchers seek solutions to siloed care, missed diagnoses and limited access to trauma-informed therapies

Study participants also reported better sleep quality and reduced use of pain medications

Two-hour training helps patients expand skills that return a sense of control
Program enhances cooperation between traditional and non-pharmacologic care

National Institutes of Health grant supports Cleveland Clinic study of first mechanism-guided therapy for CRPS
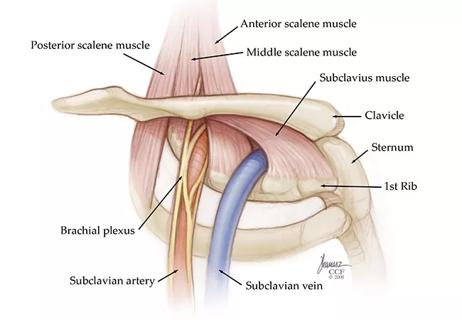
Pain specialists can play a role in identifying surgical candidates
Individual needs should be matched to technological features
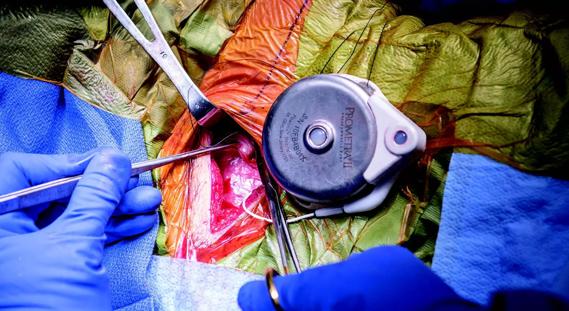
New technologies and tools offer hope for fuller understanding