Endoluminal surgery provides new treatment options
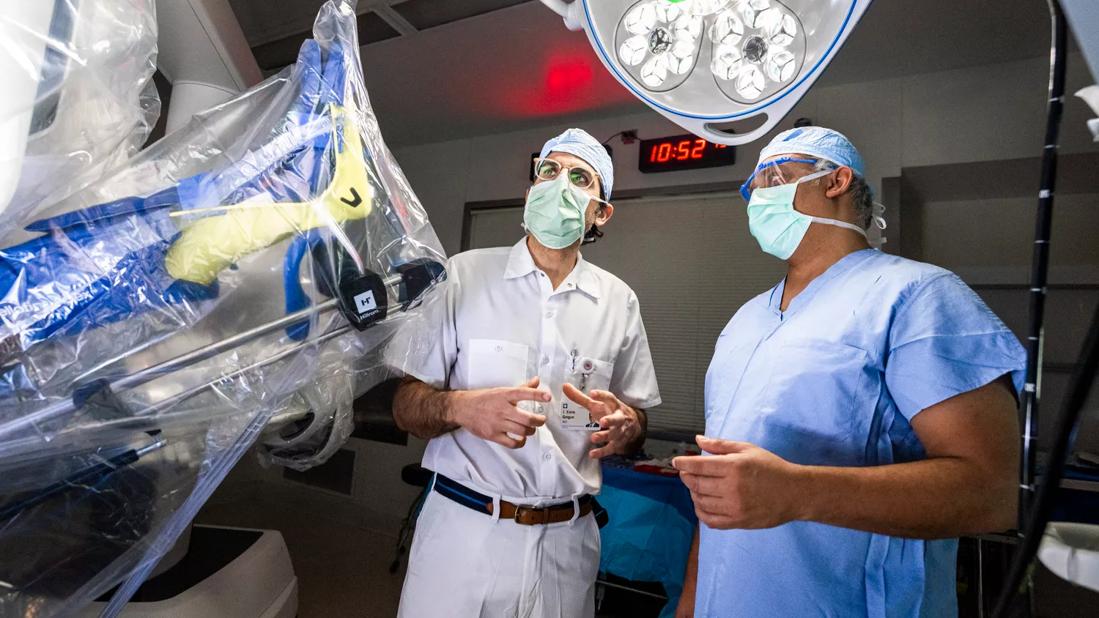
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/0d53d4fa-106f-48ae-b5c2-a2af613e4886/Gorgun-surgery-DDI)
Emre Gorgun, MD
A 59-year-old woman received a positive result on a self-administered at-home screening test used to detect neoplasia-associated DNA markers and occult hemoglobin in patients’ stool. She had no significant medical or surgical history, was not taking antiplatelets or anticoagulants, and reported no family history of colorectal malignancy.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Cleveland Clinic colorectal surgeon Emre Gorgun, MD, Director for Lower GI of the Digestive Disease & Surgery Institute’s Endoluminal Surgery Center, performed a full colonoscopy, which is recommended for patients with positive self-test results. The procedure identified a large 10-cm by 9-cm multilobulated, frond-like polypoid lesion in the patient’s ascending colon, 7-10 cm from the ileocecal valve. The polyp was nonobstructive but occupied approximately two-thirds of the luminal circumference.
Importantly, the lesion was not affixed or tethered to the underlying bowel wall, a finding that suggested a benign condition; however, Dr. Gorgun was concerned that the interior portion of the lesion could contain an invasive cancer. A biopsy revealed fragments of a benign tubulovillous adenoma polyp with malignant potential. An abdominal CT was unremarkable and did not demonstrate a colonic lesion or any evidence of metastatic cancerous spread.
The patient was presented with two treatment options: endoscopic excision using advanced resection techniques or formal surgical bowel resection.
Recent technological advances have made it possible to remove precancerous, cancerous and complex polypoid lesions of the gastrointestinal tract endoscopically, rather than using traditional surgical bowel resection. This new field of endoluminal surgery, which is only available at advanced tertiary care centers such as Cleveland Clinic, avoids extensive surgery and allows patients to keep their native organs and have an improved quality of life. Endoluminal surgery involves procedures such as endoscopic submucosal dissection, complex endoscopic mucosal resection, endoscopic full-thickness resection and submucosal tunneling endoscopic resection.
Advertisement
Video content: This video is available to watch online.
View video online (https://www.youtube.com/embed/RIhPA4tAjD8?feature=oembed)
Cleveland Clinic Quick Case: Endoluminal Surgery (Graphic)
Dr. Gorgun’s patient chose to undergo endoscopic submucosal dissection (ESD) of the lesion. Following full bowel preparation, the patient was administered preoperative intravenous antibiotics for infection prophylaxis and subcutaneous heparin to reduce the risk of a thromboembolic event. The patient was placed under general anesthesia with complete muscle relaxation, which is standard for ESD.
“The first step in the procedure involves creating a ‘lift’ of submucosal tissue around the lesion by injecting the submucosal layer with a gelatin-based colored dye solution,” explains Dr. Gorgun. “In this case, we used a proximal-to-distal approach to inject 30-40 mL of a viscous submucosal gel that separates the lesion from the underlying muscular layer of the bowel wall and allows full endoscopic excision of the entire specimen with layers deep enough for full pathological assessment.”
Working distally to proximally — at times with the endoscope in the retroflexed position — Dr. Gorgun excised the lesion en bloc using a 2-mm electrosurgical knife. The tool’s pin-tip point enabled accurate dissection between the layers of the bowel wall. “It is important in dissection to achieve adequate margins around the specimen,” Dr. Gorgun says.
The 10-cm by 10-cm lesion was retrieved using an endoscopic net device and sent for histopathological analysis. Dr. Gorgun inspected the resected margins for hemostasis and any full-thickness or muscular-layer breaches requiring repair. Three 17-mm hemoclips were applied apposed to the underlying muscular layer.
Advertisement
The patient was discharged to home on the day of the procedure and subsequently could tolerate a full diet. She recovered without complications and experienced no abdominal pain or rectal bleeding.
Final histopathology of the specimen showed a tubulovillous adenoma with clear margins and no evidence of underlying dysplasia. The patient did not require further treatment and was scheduled for a repeat colonoscopy in 6 months for surveillance.
Figure 1. Frond-like polypoid lesion in the ascending colon.
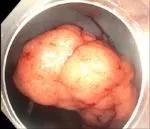
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/a03bf830-ade3-4723-8160-511cceb744f1/ESD1-150x129_jpg)
Figure 2. Non-obstructive lesion occupying more than two-thirds of the luminal circumference.
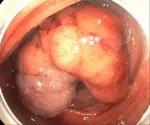
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/de716dbe-abb1-4e08-8f29-067f9d9dbd29/ESD2-1-150x125_jpg)
Figure 3. Endoluminal surgery using a 2-mm electrosurgical knife.
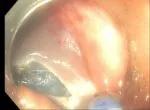
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/9bd2f8f7-809f-485a-a1bf-9198f0190a0b/ESD3-150x110_jpg)
Figure 4. Submucosal dissection with the endoknife.
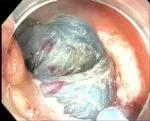
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/ce772961-ead0-4e91-9cf1-0946f7e3516f/ESD4-150x121_jpg)
Figure 5. Retrograde view of the lesion.
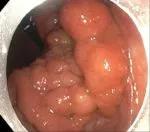
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/c33217af-5241-48f8-a663-ca82640704f5/ESD5-150x132_jpg)
Figure 6. View of the completely resected lesion site.
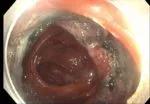
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/2b8f139e-2c96-45a5-8dce-fdbd11638504/ESD6-150x104_jpg)
Figure 7. Endoscopic clip closure of the resection site.
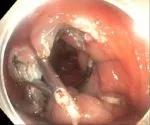
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/46e226f1-0692-4ac3-917c-e87784b44709/ESD7-150x125_jpg)
Figure 8. En-bloc removed specimen pinned on a cork board for histopathology analysis.
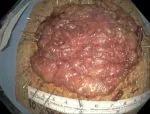
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/8a12d3b3-e69e-4f64-9a08-fa2f8a6441c4/ESD8-150x114_jpg)
Slide 1/8
Advertisement
Advertisement
Pivotal Studies Guide Treatment Decisions in Muscle-Invasive Bladder Cancer
Reflections from an oncology provider and communications educator on new ASCO Guidelines on Patient-Clinician Communication
Phase 1 trial outcomes offer encouraging news for developing targeted therapy for solid tumors
Cleveland Clinic to administer first-of-its-kind T-cell therapy
Heavily pretreated patients experience improved progression-free survival and quality of life with CD20xCD3 therapy
Innovative procedure reduces scarring, recovery time and nipple sensation
Best practices for supporting patients with honesty and compassion
Goal-of-care discussions drive earlier hospice access