Partial resection plus radiation leads to good outcome from an unpredictable tumor
A 46-year-old man presented in 2016 with progressive weakness and back and leg pain. MRI revealed a tumor completely filling the spinal sac from L3 to the sacrum (Figure 1). Due to its presumably intradural location and bulging appearance, a myxopapillary ependymoma was suspected.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
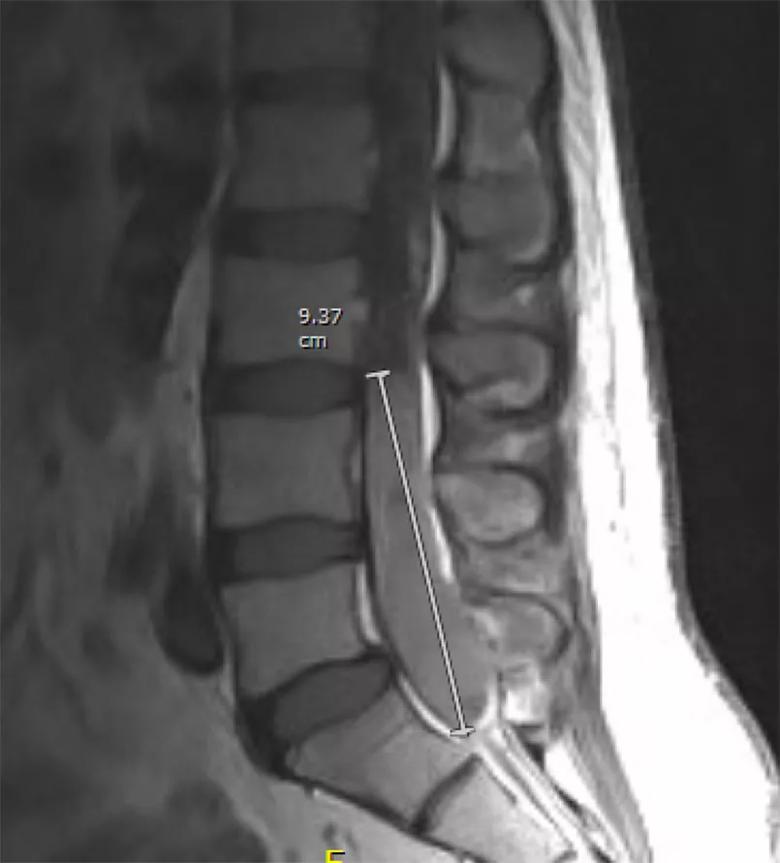
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/d55a6433-81bc-4892-87b2-bde4330deba4/20-NEU-1892172-spinal-ependymoma-on-MRI_jpg)
Figure 1. The patient’s preoperative MRI showing a tumor that completely fills the thecal sac from L3 to the sacrum.
Surgery was performed by Cleveland Clinic Center for Spine Health neurosurgeon Edward Benzel, MD. “When we got inside and saw the tumor, we were shocked by how extensive it was,” he says. “It had invaded into the cauda equina, completely surrounding the nerves, and had violated the dural sac with an accompanying extensive extradural component.”
During the six-hour operation, Dr. Benzel and his team tried to remove as much of the tumor as possible, but it could not be completely resected, as tumor adhered to the dural wall and nerves. Nerves with tumor attached that appeared nonfunctional by intraoperative neuromonitoring were resected.
Histology confirmed the diagnosis of ependymoma, classified by the WHO system as anaplastic grade III, the most malignant type. The tumor exhibited prominent cellularity, necrosis, vascular proliferative changes and identifiable mitotic activity.
Surgery was followed by radiation to the area.
At his most recent follow-up in late 2019, the patient was able to walk with minimal deficit and maintained good function. He was being managed by Cleveland Clinic’s Chronic Pain Neurorehabilitation Program.
MRI monitoring has been performed every six months since surgery. He has evidence of extensive scar tissue at the operative site, as well as a small tumor within the dural space below L1, above the area of the primary tumor (see Figure 2). Because these findings have remained stable, Dr. Benzel plans to consider reducing the frequency of MRI monitoring to every 12 months after discussion with the patient.
Advertisement
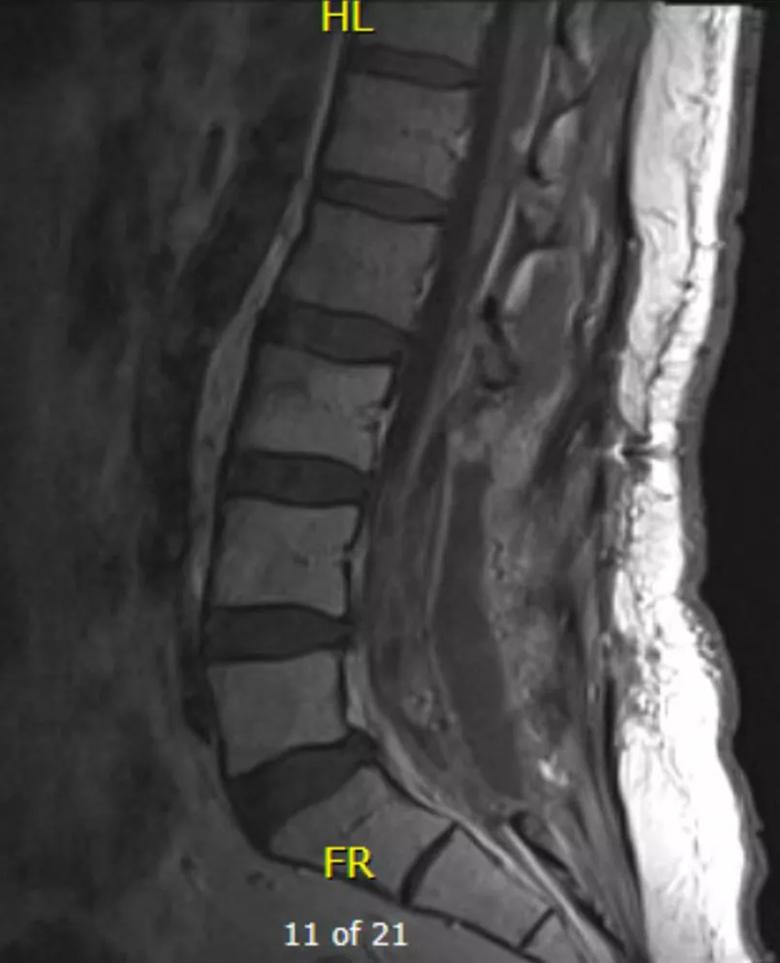
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/11bcd626-858d-4895-a5fc-68b5b95f44b6/20-NEU-1892172-postop-spinal-ependymoma_jpg)
Figure 2. A postoperative monitoring MRI from 2018. Extensive scar tissue is evident where the tumor was resected. A small white lesion is visible just below L1. Of note, it is higher than the location of the original tumor and is likely a result of seeding. Findings have not changed over serial monitoring MRIs.
Ependymomas are rare primary central nervous system tumors, constituting about 2% of such cancers in adults and 5% in individuals younger than 20. Dr. Benzel notes that he has operated on just a small handful of malignant ependymomas in his 40 years as a busy spine surgeon. In this case, he said, the tumor appeared so large and aggressive on the preoperative MRI that it gave him pause about whether the potential benefit would outweigh the surgical risk.
He highlighted a few takeaways from this case, outlined below.
Ependymomas are unpredictable. Because these tumors are so rare — and so varied — evidence is inadequate to reliably predict their behavior, and extrapolating experience from other tumors can be misleading.
“If an astrocytoma displayed such aggressive characteristics as this patient’s tumor did, I would not have expected his disease to be neurologically and radiographically stable nearly four years after subtotal resection,” says Dr. Benzel, Emeritus Chair of Neurosurgery at Cleveland Clinic. “The good long-term outcome in this case surprised us all.”
A few prognostic trends have been reported in the literature. Five-year survival is very good (likely above 95%) for adults with ependymomas in general and about 55% for adults with anaplastic ependymomas. A spinal location tends to have a more favorable prognosis than a brain location.
Advertisement
Standard treatment is surgery, with radiation for some cases.Surgery is the most established therapy, and because total resection can be curative, experts recommend conducting an MRI within a day or two after surgery so that a second operation can be considered to immediately address any residual tumor found that could be resectable. Radiation is indicated especially for patients for whom full resection is impossible. The role of chemotherapy is unclear, although some have suggested its use for young children instead of radiation therapy to avoid radiation-induced harm to the nervous system.
“We will consider all options if we see signs of progression, because there is no recipe for this and we need to treat each case individually,” says Dr. Benzel.
Focus on quality of life.Continued pain, which is typical following an extensive tumor resection in the central nervous system, should be addressed.
“A chronic pain management clinic that emphasizes a comprehensive approach can be invaluable for such patients to optimize function,” concludes Dr. Benzel. “A good program combines physical and cognitive behavioral therapy, lifestyle techniques and judicious use of medications.”
Advertisement
Advertisement

Aim is for use with clinician oversight to make screening safer and more efficient

Rapid innovation is shaping the deep brain stimulation landscape

Study shows short-term behavioral training can yield objective and subjective gains

How we’re efficiently educating patients and care partners about treatment goals, logistics, risks and benefits

An expert’s take on evolving challenges, treatments and responsibilities through early adulthood

Comorbidities and medical complexity underlie far more deaths than SUDEP does

Novel Cleveland Clinic project is fueled by a $1 million NIH grant

Tool helps patients understand when to ask for help