Transplantation in this setting requires extensive resources, experience and recovery time
A 56-year-old physician contracted COVID-19 while caring for patients. He was diagnosed in late March and treated with a five-day course of hydroxychloroquine and azithromycin. After worsening at home, he was admitted to his local hospital on the East Coast in early April. Despite treatment with steroids, tocilizumab and anakinra, he continued to decline and was transferred six days later to a regional tertiary care center, where he was intubated, placed on a mechanical ventilator and given the experimental treatment of convalescent plasma.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
In spite of convalescent plasma, as well as inhaled nitric oxide and proning, his pulmonary status continued to deteriorate and in mid-May (hospital day 45) he was placed on veno-venous extracorporeal life support (VV-ECLS). While on this support, he suffered numerous complications including bacteremia, a bradycardic arrest and a gastrointestinal bleed, but he and his team persevered. His lungs showed no improvement on ECLS and began to manifest signs of irreversible damage, so his medical team reached out to Cleveland Clinic’s lung transplant program.
“After assessing his potential suitability for transplantation, and knowing that certain aspects of his clinical status (such as deconditioning) would need to improve prior to transplant, we decided to transfer him to Cleveland Clinic,” says Kenneth McCurry, MD, Surgical Director of Lung and Heart-Lung Transplantation at Cleveland Clinic. He explains that in addition to standard criteria to determine candidacy for lung transplantation, patients with COVID-19-related acute respiratory distress syndrome (ARDS) must also be free of the virus and otherwise have intact organ systems. Exceptions are sometimes made to accept young patients if they have one other failing organ system.
The patient was admitted to Cleveland Clinic in early June (hospital day 66) and kept in COVID-19 precautions while he underwent PCR-based testing of nasopharyngeal swabs and bronchoscopy specimens. When the results came back negative for COVID-19, he was placed in the lung transplantation ICU. Evaluation for bilateral lung transplantation was then completed and rehabilitation started (Figure 1). (Details of the Cleveland Clinic experience with ECLS as a bridge to lung transplantation were recently described in Annals of Thoracic Surgery [2018;106(1):192-198].)
Advertisement
“We place a strong emphasis on having our patients who are on ECLS as a bridge to lung transplant awake and ambulating before transplantation,” says Dr. McCurry. “Our protocolized approach has led to very good outcomes.”
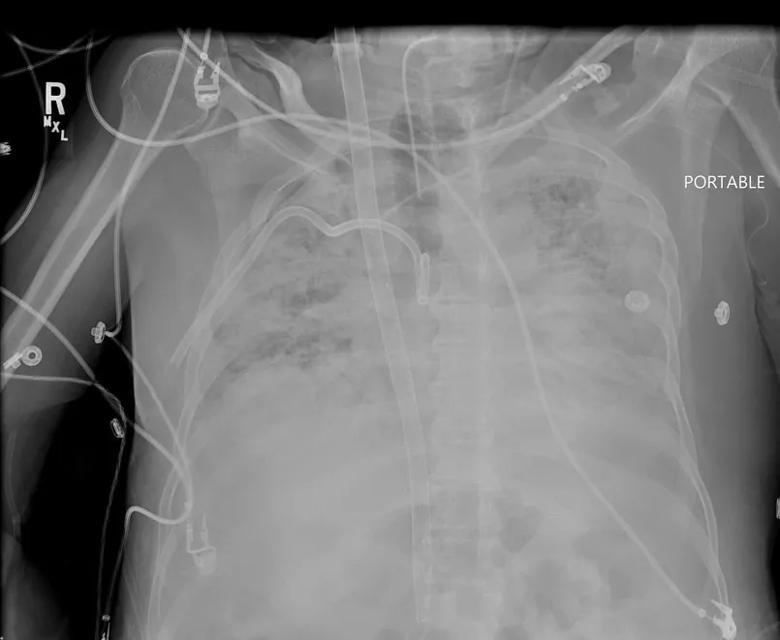
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/58c274e8-8343-4f82-9a46-9d2e2573df05/20-HVI-1965991-Inset-1_jpg)
Figure 1. A chest x-ray taken shortly after transfer to Cleveland Clinic demonstrates the extensive bilateral air space disease typical of COVID-19-related ARDS. The patient’s course had also been notable for a right pneumothorax requiring pigtail placement (seen in right chest). The dual-lumen ECLS cannula that was providing access to blood for gas exchange on the ECLS circuit is also visible. This cannula allows single-site upper body access for ECLS, facilitating mobilization.
At this point, the patient had been in bed for many weeks, often while heavily sedated and under intermittent chemical paralysis. He was flaccid and on many medications. The ICU team began the process of weaning the medications to allow him to be more alert and start physical therapy.
During this time, a few complications developed, including pulmonary hypertension with evidence of right ventricular failure that required conversion to veno-arterio-venous ECLS, a form of ECLS that supports the lungs as well as the right ventricle.
He gradually became alert enough to start to participate in his treatment plan, in collaboration with his wife, the referring medical team (who maintained contact) and the transplant team. During this time, the team discussed the patient’s situation with him directly and confirmed his desire to proceed with lung transplantation, if feasible. By mid- to late July, he was able to ambulate and was placed on the transplant list. Due to the severity of his illness and the required mechanical cardiopulmonary support, he had a very high lung allocation score, which is used to determine priority for lungs in the U.S.
Advertisement
In late July (hospital day 116), bilateral lung transplantation was performed. The patient’s lungs were densely consolidated (Figure 2), with a texture and feel that Dr. McCurry describes as more resembling liver rather than lung tissue.
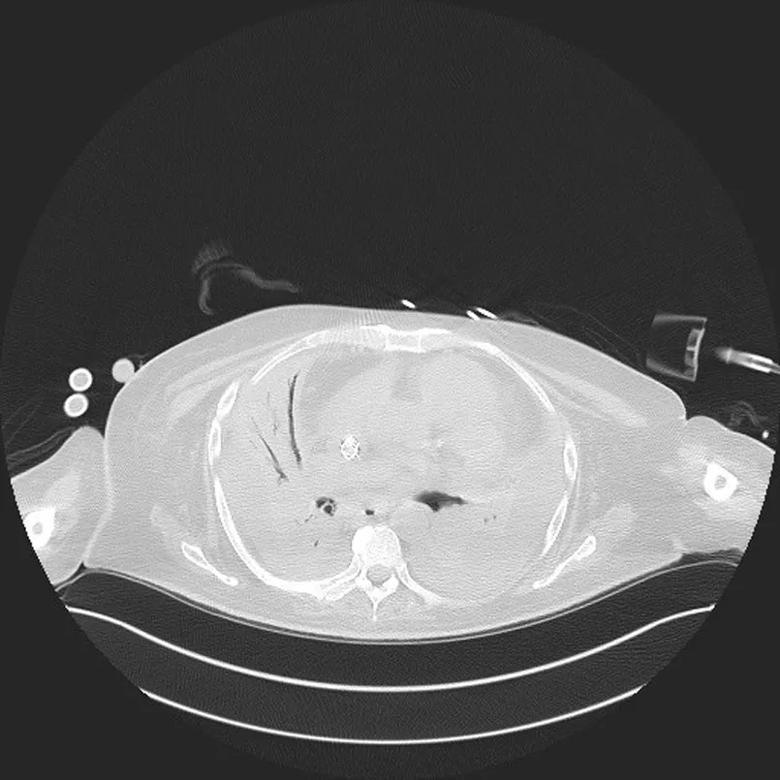
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/39905ac8-3691-468e-af52-ae820daab4fc/20-HVI-1965991-Inset-2_jpg)
Figure 2. A chest CT taken a few days before transplantation shows densely consolidated lungs with air bronchograms, volume loss in the lungs and bilateral pleural effusions. Also seen is the dual-lumen ECLS cannula that courses through the superior vena cava and right atrium into the inferior vena cava.
Dr. McCurry emphasizes that considerable effort is taken to protect staff caring for patients with COVID-19, particularly surgical and operating room personnel who work directly with the airway, such as in lung transplantation. “Although we require that patients test negative for the virus before transplantation, we are still concerned that virus might harbor deep in the lungs or that residual viral RNA may pose a risk,” he explains, noting that N95 masks are worn. “There are many unknowns with COVID-19, so continued precautions are warranted.”
After transplantation, the patient was returned to one of the COVID-free transplant units, which were established at Cleveland Clinic a few months ago for all transplant patients. Patients must first be tested for COVID-19, and no visitors are allowed. The rules are the same even for patients with previous COVID-19 infection, as there is no way to know if they are immune.
The patient’s recovery has been slow but unremarkable, with good lung and heart function, Dr. McCurry reports. Not unexpectedly, the patient has had psychological ups and downs. While very motivated at first, he has lapsed into depression at times. His transplant team, along with his wife and referring colleagues, have helped him overcome these periods.
Advertisement
At this writing, six weeks after transplantation, Dr. McCurry is optimistic that the patient will recover, with anticipated discharge in another six weeks if he continues to progress without major setbacks. He is removed intermittently from the ventilator, as part of the weaning process, and while he remains weak, his strength and ambulation are improving.
Between five and six weeks after transplant, he was moved out of the COVID-free unit so that his wife could visit and help with rehabilitation. According to Dr. McCurry, risk of catching the virus must be weighed against the many benefits of family support.
About a dozen cases of bilateral lung transplant for COVID-19-related ARDS have now been reported in the literature worldwide. “These patients are all extremely complex and can be expected to be very sick for a long time,” Dr. McCurry notes.
He recommends considering lung transplantation when a patient with COVID-19 is not responding to therapy and is either approaching or at the point of irreversible lung damage and is unlikely to recover. Early consultation with a lung transplant program is advised and can be highly beneficial.
“Extensive resources are required for transplanting and caring for patients with COVID-19-related ARDS, and only transplant programs that are experienced in working with very high-risk patients should be considered for referral,” he advises.
Advertisement
Advertisement
Patients report improved sense of smell and taste
Clinicians who are accustomed to uncertainty can do well by patients
Unique skin changes can occur after infection or vaccine
Cleveland Clinic analysis suggests that obtaining care for the virus might reveal a previously undiagnosed condition
As the pandemic evolves, rheumatologists must continue to be mindful of most vulnerable patients
Early results suggest positive outcomes from COVID-19 PrEP treatment
Could the virus have caused the condition or triggered previously undiagnosed disease?
Five categories of cutaneous abnormalities are associated with COVID-19