Model distinguishes between conditions with 86% accuracy
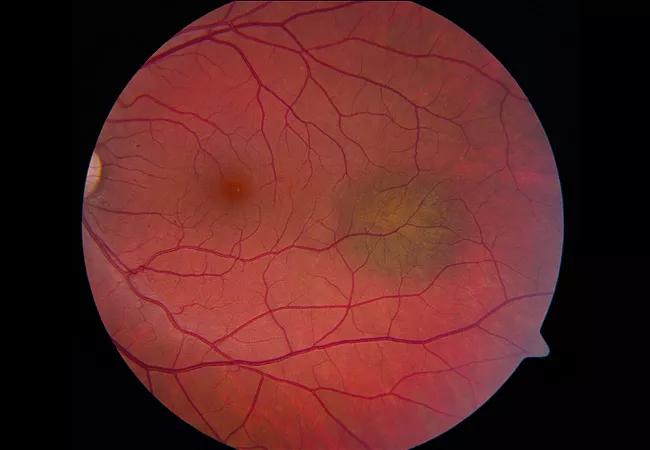
A novel machine learning-based model may help improve the diagnosis of choroidal melanoma, an aggressive ocular malignancy. A study recently published in Ocular Oncology and Pathology confirmed that the model can distinguish between a benign choroidal nevus and melanoma of the eye with a high 86% accuracy.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“This model has a direct implication on reducing the number of suspected cases of small choroidal melanoma and reducing overtreatment,” says study co-author Arun D. Singh, MD, Director of Ophthalmic Oncology at Cleveland Clinic Cole Eye Institute.
Dr. Singh explains that diagnostic uncertainty complicates the management of patients with suspected small choroidal melanoma. Distinguishing between a choroidal nevus and melanoma is difficult, especially when the lesion is small. This is because conventional imaging technologies, such as optical coherence tomography (OCT) and ultrasound, are not discriminative enough for small lesions, while biopsies of eye tissues carry significant risks.
“Choroidal nevi are very common, and choroidal melanoma is very rare,” says Dr. Singh. “But we know that some nevi will transform into melanoma. Also, some melanomas will arise de novo in the eye and will look like the nevus initially, but they’re actually evolving melanomas (Figure 1). So, when we look at something small, it’s hard for us to know if it’s a nevus that’s been there for a long time and we need to do nothing about it, or if it’s melanoma that’s evolving and we need to do something about it.”
Small choroidal melanoma is typically diagnosed based on an eye exam and clinical features.
“About 50% of cases of melanoma of the eye will metastasize over 15 years,” says Dr. Singh.
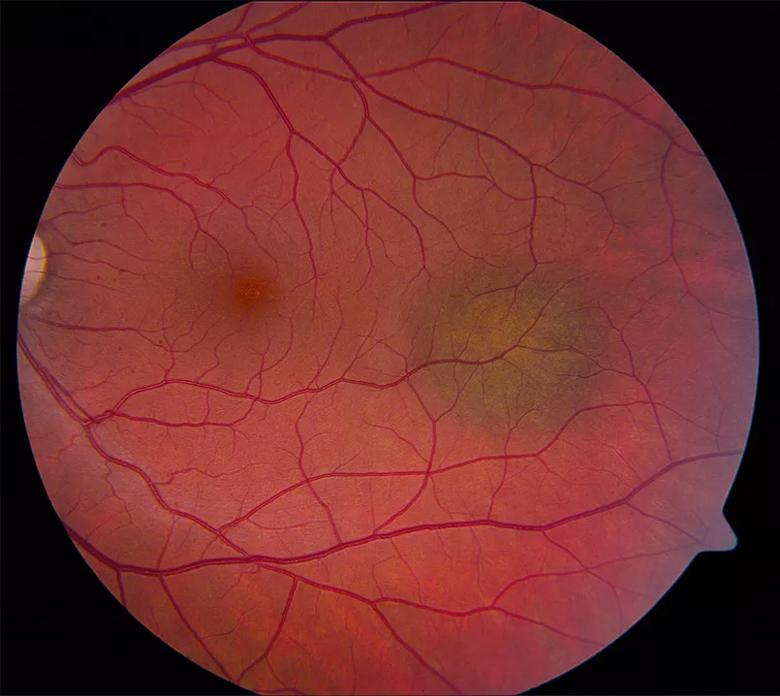
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/a8456aa5-0e88-4fe7-8a56-fa081893b1d8/22-EYE-2850011-Prediction-model-to-identify_Singh_805x718_inset_jpg)
Figure 1. A 33-year-old man was initially diagnosed with a choroidal nevus of the left eye and observed for three years. During this time, the lesion doubled in size, leading to a referral to the Cole Eye Institute. At presentation, the patient had no symptoms and had visual acuity of 20/20. Fundus examination of the left eye revealed a small choroidal melanocytic tumor (4.5 mm x 3 mm in basal dimension) with minimal elevation of about 1.0 mm. A presumptive clinical diagnosis of small choroidal melanoma was made, and he was treated with episcleral brachytherapy. He has remained free from local recurrence and metastasis for the last 10 years.
Advertisement
The current study aimed to develop and validate a machine learning model for diagnosing small choroidal melanoma. Data used to develop the model were collected from 123 patients diagnosed with a small choroidal melanocytic tumor based on Collaborative Ocular Melanoma Study criteria. Sixty-one patients with melanoma had documented growth or pathologic confirmation; 62 patients with stable choroidal nevi served as negative controls. The model was validated using an external validation dataset that included 240 patients with small choroidal melanocytic tumors. The study’s primary outcome was the model’s probability of predicting small choroidal melanoma.
Dr. Singh explains that his team used machine learning to integrate important features of small choroidal melanoma into a predictive algorithm.
“We looked at many parameters that are traditionally known to be significant for these tumors, such as the size, location, orange pigmentation, presence of drusen and height,” he says. “When you put the features into this model, you’re able to figure out mathematically the chance that a certain tumor is melanoma.”
The model’s predictive capability, validated on the external dataset, was 0.861. This means that the model can distinguish between a choroidal nevus and melanoma with a very high discrimination accuracy of 86%.
“The performance of this model is better than any other prediction tool available,” he says.
An additional advantage is that the model relies on data obtained from noninvasive diagnostic testing, such as exams typically performed in an ophthalmology office.
Advertisement
The predictive model is already being successfully implemented and used in research studies at Cleveland Clinic.
In a recent retrospective review of approximately 150 cases of suspected small choroidal melanoma, Dr. Singh’s team found that approximately 25% of cases potentially had been overtreated. This is because, at the time of evaluation, the patients erred on the side of caution and opted for treatment even though their diagnosis could not be confirmed.
Dr. Singh is optimistic that the new model’s highly discriminative ability will prevent the overtreatment of patients in the future.
“That is the whole idea,” he says. “When the diagnosis is more certain, then the overtreatment component will go down.”
In conclusion, he emphasizes that novel diagnostic techniques should continue to incorporate newer statistical methods, such as those employed in machine learning, because of their more accurate predictive ability.
Advertisement
Advertisement

Motion-tracking Brillouin microscopy pinpoints corneal weakness in the anterior stroma

Registry data highlight visual gains in patients with legal blindness

Prescribing eye drops is complicated by unknown risk of fetotoxicity and lack of clinical evidence

A look at emerging technology shaping retina surgery

A primer on MIGS methods and devices

7 keys to success for comprehensive ophthalmologists

Study is first to show reduction in autoimmune disease with the common diabetes and obesity drugs

Treatment options range from tetracycline injections to fat repositioning and cheek lift