Operation in 21-year-old is the institution’s first total face transplant
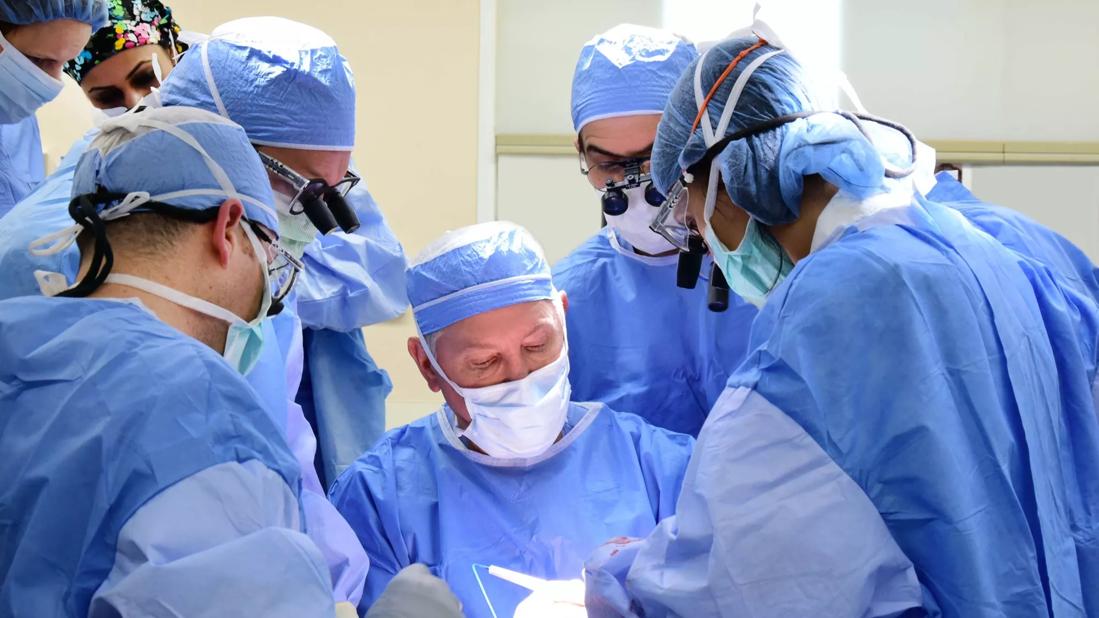
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/3c426e16-b035-4a1c-b360-c7f4e9facc34/ft_janine-sot_321-scaled-jpg)
Face-transplant
Cleveland Clinic has performed its third face transplant — and its first total face transplant to date.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The surgery was performed in May 2017 on a 21-year-old female who suffered severe facial trauma and other complications from a gunshot wound as a teenager. To protect the privacy of those involved, no further personal details about the transplant recipient or donor are being released at this time
The 31-hour procedure involved replacement of effectively 100 percent of the patient’s facial tissue, including transplantation of the following:
Patient recovery has been good, as she is walking and talking and is expected to soon begin eating orally. She will continue extensive rehabilitative therapy, including physical, occupational, speech and swallowing therapy.
The transplant is expected to give the patient the ability to speak more clearly, better express emotions via her face, and breathe, chew and swallow more effectively. Enhanced physiological, psychological and social function are expected to accompany these improvements in physical function.
The extensive surgical team was co-directed by Frank Papay, MD, Chairman of Cleveland Clinic’s Dermatology & Plastic Surgery Institute, and Maria Siemionow, MD, PhD. The team included the following Cleveland Clinic plastic surgeons: Brian Gastman, MD; James Zins, MD; Risal Djohan, MD; Mark Hendrickson, MD; Graham Schwarz, MD; Antonio Rampazzo, MD, PhD; Bahar Bassiri Gharb, MD, PhD; Raffi Gurunluoglu, MD; and Steven Bernard, MD.
Advertisement
Surgeons from this team performed multiple facial reconstructions on the patient prior to the transplant, but with the end goal of face transplantation in mind, as reconstruction alone would not correct her disfigurement or adequately improve her quality of life. They took great care during the reconstructive surgeries to safeguard any blood vessels that could potentially be used for the transplant.
“Plastic surgery is about restoring form and function,” says Dr. Papay. “Function comes before form, and prior to the face transplant, this patient had extremely poor function and form. Our job in reconstruction is to weigh the risk versus the benefit of doing face transplantation, and we felt the risk was well worth it to give this patient better function, better social form and, ultimately, a better life.”
“With a new nose and new lips, palate, eyelids and jaw, our patient now has the full opportunity to reintegrate into society and have a future just like any other young adult,” says Dr. Gastman. “This surgery can give her back the self-esteem and confidence she lost.”
He and other surgeons on the team used surgical rehearsal, 3-D-printed models and virtual reality as their primary platforms for preoperative planning to enhance the accuracy of the procedure and ensure optimal aesthetic and functional outcomes.
The plastic surgeons were joined by specialists in anesthesiology, bioethics, dentistry, ophthalmology, endocrinology, infectious disease, psychiatry, pharmacy and transplantation medicine in the comprehensive care of this complex case.
Advertisement
“This case is a prime example of how we are much more capable together than we are individually,” says Dr. Papay. “I’m extremely proud of this team for their commitment to making a difference in this patient’s life.”
That teamwork has been central to Cleveland Clinic’s leadership in face transplantation, as the first U.S. hospital to perform a face transplant (in December 2008, as detailed here) and one of only six U.S. institutions that have performed the procedure to date. It has now performed three of the fewer than three dozen face transplants conducted worldwide (see this post for details on the second of the three Cleveland Clinic cases).
This most recent face transplant was supported by the Armed Forces Institute of Regenerative Medicine I (AFIRM I) grant program from the U.S. Department of Defense. Cleveland Clinic is involved in AFIRM through the Rutgers-Cleveland Clinic Consortium (RCCC), which was formed to support advances in regenerative medicine to improve the treatment of wounded U.S. service members. Through the RCCC, Dr. Siemionow, former director of Cleveland Clinic’s Department of Plastic Surgery Research, has served as the primary investigator of this clinical trial. Now with the University of Illinois at Chicago College of Medicine, Dr. Siemionow acted as a consultant and advisor on the most recent transplant.
“I see this surgery as an important result of the investment made by the U.S. government aimed at advancing therapies for some of the nation’s most seriously injured patients,” said RCCC Director Joachim Kohn, PhD, Board of Governors Professor at Rutgers, The State University of New Jersey, in a release. “Looking ahead, the pioneering work done at Cleveland Clinic will contribute to making this important new treatment option available to other patients with devastating facial deformities.”
Advertisement
Advertisement
Family history may eclipse sun exposure in some cases
Consider secondary syphilis in the differential of annular lesions
Persistent rectal pain leads to diffuse pustules
Two cases — both tremendously different in their level of complexity — illustrate the core principles of nasal reconstruction
Stress and immunosuppression can trigger reactivation of latent virus
Low-dose, monitored prescription therapy demonstrates success
Antioxidants, barrier-enhancing agents can improve thinning hair
A hybrid approach