Preserving resources and prioritizing patient and caregiver safety
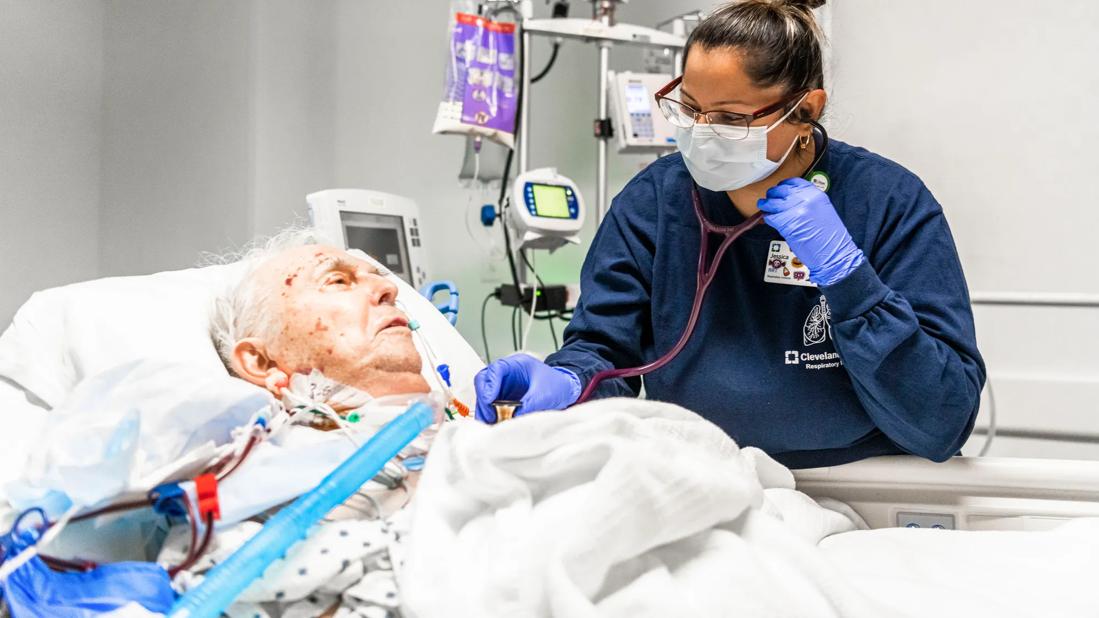
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/b29fbb3a-c684-491e-b561-7234f5433a58/HRC_2881047_04-26-22_261_MLC-jpg)
650×450-Repiratory-Therapist
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Respiratory therapy resources can be stretched to their limits during pandemics. Strong leadership is required to ensure judicious use of resources and implement standard practices while maintaining empathy for respiratory therapists who work at the front lines. Equally important is the dissemination of information through well-defined outlets (e.g. intranet sites, scheduled virtual meetings to improve procedures and shared new information). Managers should be visible on the floors supporting respiratory therapists with knowledge and understanding.
All processes have bottlenecks. In the context of SARS pandemics such as COVID-19, mechanical ventilators and, consequently, ICU beds have become the bottlenecks due to the relatively high ventilator length of stay (approximately 10 days in the case of COVID-19).
Naturally, accessories such as circuits, filters and humidification devices may become scarce commodities as the number of deployed ventilators increases. Further, when hospitals are built, engineers assume an average demand for air and oxygen flow. Therefore, there is an upper limit to the number of ventilators that can be deployed that is dependent on facility specifications. Under those circumstances, battery-run ventilators with internal compressors may become useful.
High flow nasal cannula devices are preferred over noninvasive positive pressure ventilation due to the lower likelihood of aerosol generation and, thus, less disease transmission potential. Multiplex ventilation (MpV) refers to the practice of ventilating more than one patient with a single ventilator. There is a potential for markedly different ventilation and oxygenation for patients with uneven respiratory system impedances who are paired during MpV.
Advertisement
There are three critical problems that need to be addressed to improve safety during MpV:
Multiplex ventilation is a last resort to temporize patients until additional mechanical ventilators become available.
Institutions should consider developing executive dashboards that provide daily updates on available invasive (ability to provide ventilation through an endotracheal tube) ventilator capacity. Noninvasive ventilators that can be adapted to invasive use could provide additional capability to meet surging demand.
Respiratory therapists are in the direct line of fire when dealing with SARS viruses. Any aerosol-generating procedure such as intubation, suction, bronchoscopy and nebulized treatments (due to the potential for inducing cough) requires donning N95 mask, goggles, gown and gloves. Controversy exists on the appropriate personal protective equipment (PPE) to be worn when taking care of intubated patients. Some argue for a simple face mask in place of an N95 mask, assuming a closed ventilator circuit with appropriate filters applied. However, the risk of circuit disconnection while working with an intubated patient is not trivial. Strong consideration should be given to wearing N95 masks while taking care of intubated patients. N95 sparing strategies, (e.g. disinfection of masks after use or reuse with careful donning and doffing) are highly recommended.
Advertisement
When respiratory therapists have documented exposure to the virus, they can continue to work unless symptomatic given the workforce shortages during pandemics. In the case of SARS-CoV-2, transmission by asymptomatic individuals has been strongly inferred from epidemiological studies. Consequently, a face mask should be worn at all times if work is continued.
The discipline of respiratory therapy is a North American invention that originated in the 1940s. Respiratory therapists have become an integral part of hospitals as providers of inhaled therapy, experts in evaluating and using respiratory equipment including oxygen delivery devices, airway maintenance tools, airway clearance and reinflation devices and mechanical ventilators. At no time is the value of a seasoned respiratory therapist at the bedside appreciated more than during a SARS pandemic.
About the author
Dr. Hatipoğlu is a staff member at Cleveland Clinic’s Respiratory Institute. He also serves as the Enterprise Medical Director of Respiratory Therapy and Section Head of Respiratory Therapy, Department of Critical Care Medicine.
Advertisement
Advertisement
Patients report improved sense of smell and taste
Clinicians who are accustomed to uncertainty can do well by patients
Unique skin changes can occur after infection or vaccine
Cleveland Clinic analysis suggests that obtaining care for the virus might reveal a previously undiagnosed condition
As the pandemic evolves, rheumatologists must continue to be mindful of most vulnerable patients
Early results suggest positive outcomes from COVID-19 PrEP treatment
Could the virus have caused the condition or triggered previously undiagnosed disease?
Five categories of cutaneous abnormalities are associated with COVID-19