Telehealth for inpatients and outpatients
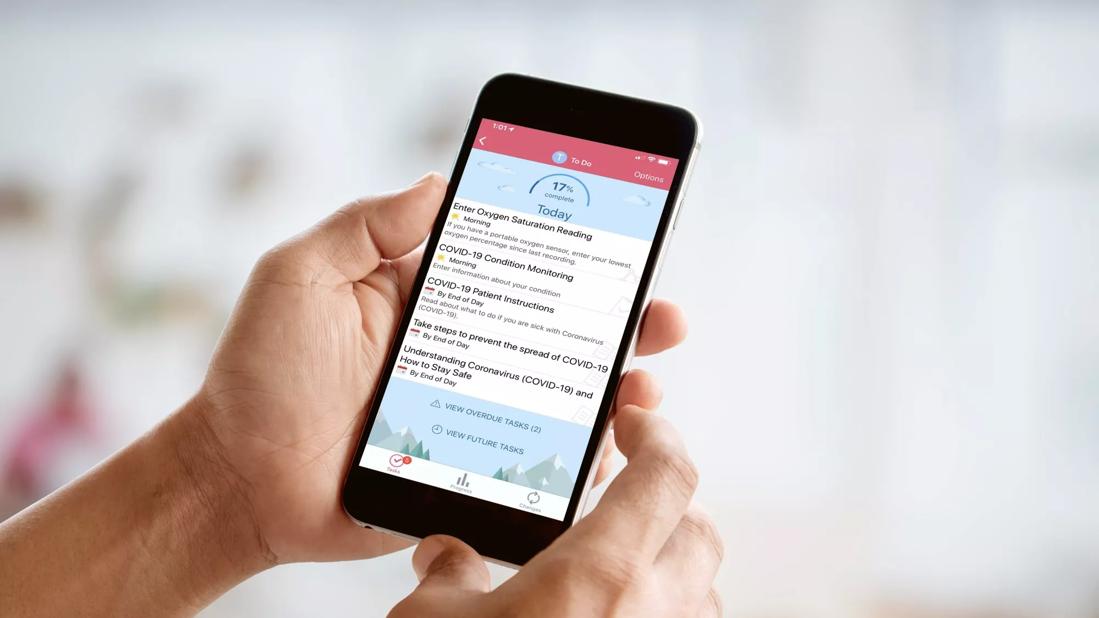
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/30d67177-4983-418a-8425-64dd2a3b9d8d/Epic-scaled-jpg)
Communication
In an attempt to lessen the impact of coronavirus/COVID-19 cases, Cleveland Clinic and other healthcare organizations across the globe are rapidly increasing the use of telehealth technology.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Telehealth is enhancing patient access to care, improving safety of patients and caregivers, and helping conserve personal protective equipment. Additionally, the sudden increase in telehealth technology is also igniting a redesign of the current healthcare system and the way care is provided.
For more than 7 years, Cleveland Clinic has been incorporating telemedicine into its care models. But, like many health organizations, the progression of use has been fairly slow and steady.
That is no longer the case. Today, in the midst of the COVID-19 crisis, 80% of patient visits at Cleveland Clinic are being done via telehealth technology. And telehealth visits are offered first – instead of in-person visits.
Nurses specifically, have adapted amazingly well to the increased use of telemedicine. In fact, the nursing leadership team at Cleveland Clinic notes several significant changes in the way nurses are caring for patients.
In the inpatient setting, nurses and care managers have started communicating with patients via telephone. Caregivers call patients from outside patient rooms to tell them they will be entering their room and asking the patient what their needs are so the nurse can be prepared to respond upon entry.
The phone calls help minimize the number of times caregivers enter patient rooms, reduce the risk of infection and improve care efficiency as more caregiver needs are met with one interaction. Care managers are also finding out the patient discharge needs via phone and setting up post-discharge services electronically. Cleveland Clinic has also been conducting plan of care visit rounds virtually, instead of in-person, using mobile iPhone technology. Typically, plan of care rounds include a team of five to six caregivers visiting patient rooms in person.
Advertisement
In the primary care setting, telehealth technology is allowing patients to meet with advanced practice registered nurses and other care providers and nurses for medical services without face-to-face interaction. At Cleveland Clinic, patients can meet with caregivers via call-in/phone visits or through scheduled or 24/7 on-demand virtual visits via Cleveland Clinic’s Express Care® Online platform.
Additionally, specifically for the care of COVID-19 patients, Cleveland Clinic recently built a new patient registry into its EPIC healthcare software. Every day, roughly 200 registered nurses use the registry to help care for COVID-19 patients who were previously hospitalized or who are being treated remotely.
The nurses provide telephonic care to help patients manage their symptoms, answer patient and family member questions, and more. Since implementation of the COVID-19 nurse phone calls, Cleveland Clinic has learned:
Advertisement
In addition, Cleveland Clinic COVID-19 patients who are being managed at home are using an app that prompts them to upload symptoms and temperature readings throughout the day. Nurses are alerted of any ‘red flags’ in a patient’s condition, allowing them to follow up in real time.
The COVID-19 patient phone calls have unveiled unexpected increases in both efficiency and productivity of nursing care. Nurses making the COVID-19 phone calls are often doing so remotely. Because these nurses aren’t commuting or getting ready to go into the traditional workplace setting, on average, Cleveland Clinic is achieving at least three more patient touches per day per nurse. A quick phone call is a great way to keep tabs on lots of patients.
Prior to the COVID-19 pandemic, much of the feedback Cleveland Clinic received from patients was that they didn’t want to talk to their caregivers on the phone and preferred in-person health visits to online or virtual health visits. Now, patients are looking forward to the phone calls, they are texting with caregivers and they are getting online and asking questions via virtual forums.
Although hands-on care is often irreplaceable, now more than ever, it is apparent that telehealth will be an important part of the future of healthcare.
In just a few weeks of increased telehealth practices at Cleveland Clinic, telephonic and virtual medicine approaches have proven to create value by saving time, improving efficiencies and productivity, increasing patient touches and enhancing clinical care.
Advertisement
Advertisement
Patients report improved sense of smell and taste
Clinicians who are accustomed to uncertainty can do well by patients
Unique skin changes can occur after infection or vaccine
Cleveland Clinic analysis suggests that obtaining care for the virus might reveal a previously undiagnosed condition
As the pandemic evolves, rheumatologists must continue to be mindful of most vulnerable patients
Early results suggest positive outcomes from COVID-19 PrEP treatment
Could the virus have caused the condition or triggered previously undiagnosed disease?
Five categories of cutaneous abnormalities are associated with COVID-19