A surgeon’s perspective: three patient groups
For spine surgery to succeed, the procedure must work and the hardware must function. Success requires that the surgery itself goes well, yet the mechanics are just part of the equation.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The successful management of pain also determines whether spine surgery improves a patient’s quality of life. From a surgeon’s perspective, odds are greatly enhanced by a nuanced understanding of the patient’s pain history, partnering with colleagues in pain management, and the use of Enhanced Recovery After Surgery (ERAS®) techniques. This approach has the best chance of minimizing opiates, maximizing patient satisfaction, expediting recovery and preventing surgeries from being done on those unlikely to benefit, says Michael Steinmetz, MD, Chairman of Cleveland Clinic’s Department of Neurosurgery.
This more holistic approach is relatively new — a result of the national opioid crisis and the introduction of revised regulations.
“It used to be that you’d operate on somebody and give them enough pain pills afterward so that they were comfortable,” Dr. Steinmetz says. “With the new regulations, we were able only to give small amounts of opiates, even after surgery, and for very specific reasons. We had to refocus our approach.”
Physicians’ concerns that reducing reliance on opioids would lead to patient suffering and dissatisfaction have not been borne out, and the turn toward multimodal pain treatment has yielded positive outcomes.
“We’ve started to see that things have changed,” Dr. Steinmetz adds. “We don’t have as many patients coming in (for surgeries) on chronic opioids, although they still come in, and our goal is to get them off fairly quickly afterward. It’s been a frame shift in the surgical approach to these patients. We are much more thoughtful about the process today than we’ve ever been.”
Dr. Steinmetz identifies three spine patient groups that call for distinct approaches.
Advertisement
Group 1 patients typically are suffering acute events, such as a herniated disk or pain from stenosis, and have never taken opioids.
“We’ll operate on them and try to get them back to their lives,” says Dr. Steinmetz. “We should be able to give them a small amount of opiates and get them off them fairly quickly.”
Opioid-minimizing efforts begin during the preoperative period. “Before these patients come up to surgery, they’re getting a bolus of Tylenol and gabapentin,” says Dr. Steinmetz. “The anesthesiologists try to use agents outside of opiates, like epidural blocks, in and around the time of surgery to try to prevent pain afterward. We inject liposomal bupivacaine. We do everything we can before surgery, during surgery and after surgery using multimodal, opiate-sparing strategies.”
Group 2 patients also tend to have common lower-back pathologies, but they have been taking opioids.
“I might see somebody who has had lumbar spinal stenosis and leg pain for six months, and their primary care doctor has put them on low-dose opioids,” says Dr. Steinmetz. “This is not somebody who truly has a psychological chronic pain disorder, but because they’re coming in on opioids, this is a challenging patient.”
Opioid history is an independent predictor of poor outcomes after all types of spine surgery, says Dr. Steinmetz. Often the drug is treating or masking depression, anxiety or other life stressors – conditions that can complicate pain management and hinder recovery. And if opiate use is not carefully handled, this patient risks developing ongoing drug dependency.
Advertisement
“We have to deal with that patient differently than the first patient,” he says.
ERAS protocols help. They include preoperative education for the patient and family, physiological and psychological optimization, multimodal analgesia, limited postsurgical use of narcotics, and training in nonpharmacological methods for managing pain. “ERAS is a multidisciplinary, multimodal approach to reduce surgical stress response, length of hospital stay and complications, all while improving the patient’s time to get out of the hospital and into rehab and recovery,” says Dr. Steinmetz. “ERAS is not specific to spine or pain management, but it has been shown to be cost-effective, safe and beneficial, and we apply that in the spine world.”
Pathologies among members of this group are likely to be more complicated and include failed back surgery syndrome, previous back surgeries and perhaps deformities, such as scoliosis. “These are people who have had back pain every day, all day long, and can’t get away from the pain. They have a psychological issue with this,” he says. “They’re often on high-dose opiates, they aren’t able to work, and they tend to be heavy smokers. Their life is pain.”
The profile can also include young people who have had multilevel fusions. “Never for one minute of the day did they get better from these operations,” he says. “And then they had four other surgeries since then.”
Yet often these patients often show up with the hope that just one more surgery will fix their pain.
Advertisement
Psychological distress is a defining factor in group 3 patients. And while these patients also may well have a problem that can be addressed with surgery, says Dr. Steinmetz, they may not be ideal candidates for surgery unless they can be physically and psychologically optimized. “Everything is more challenging with them, such as treating their pain afterwards,” he says. “They need much higher dosages. We’ve got to partner with our pain management colleagues, and these patients need some psychological treatment ahead of time as well.”
All three patient groups benefit from presurgical optimization, including management of expectations about postsurgical pain. A two-hour, clinician-led online class for spine patients, called TREK for Surgical Success, is based on ERAS principles, and is designed specifically for spine-surgery patients.
But for those experiencing depression, anxiety and other psychological issues, the best opportunity for good outcomes depends on a multimodal approach that begins with specialists in pain psychology.
“You can’t just throw painkillers at someone who has psychological distress and expect them to be happier with their hospital care,” Dr. Steinmetz says. “We need to use things like music therapy and physical therapy. We can reduce opiates and keep patients satisfied, and in fact throwing opiates at them does not make them happier.”
Cleveland Clinic’s Back on TREK program tailors such care for patients with chronic pain. Back on TREK can take up to 10 weeks, depending on patient variables.
Advertisement
“In the past, we might see these patients and say ‘I’m a surgeon, and you have chronic pain. I’m sending you to pain psychology,’ and that was it,” says Dr. Steinmetz. “Now we say, ‘Maybe you do need surgery. But let’s partner with pain management and with psychology. We going to optimize you for a successful surgery.’ So it’s a true partnership.”
Setting appropriate expectations is essential, he adds.
“We try to steer away from saying, ‘I’m going to make you pain free.’ The goal is to try to get the patient back into a functional existence again. With the help of pain management and surgery, we can make that happen.
“When all of that comes together, I think we can do a pretty good job on these patients when we choose to operate,” says Dr. Steinmetz.
Advertisement

Add AI to the list of tools expected to advance care for pain patients
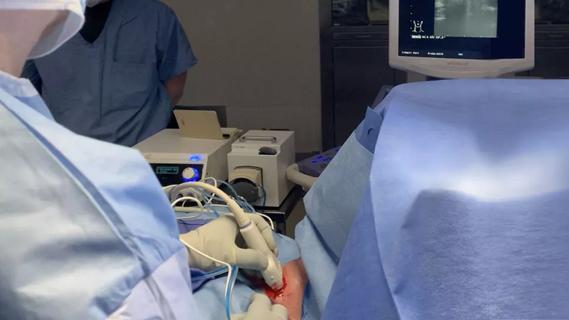
Radiofrequency ablation significantly reduces symptom severity, shrinks nodules

Telehealth aids in treatment of fibromyalgia and median arcuate ligament syndrome
Program enhances cooperation between traditional and non-pharmacologic care

Compassion, communication and critical thinking are key

Cleveland Clinic study investigated standard regimen

Despite the condition’s debilitating, electric shock-like pain, treatment options are better than ever

Success for these complex operations requires judicious patient selection and presurgical patient optimization