First-in-man trial demonstrates safety, promising functional response rates
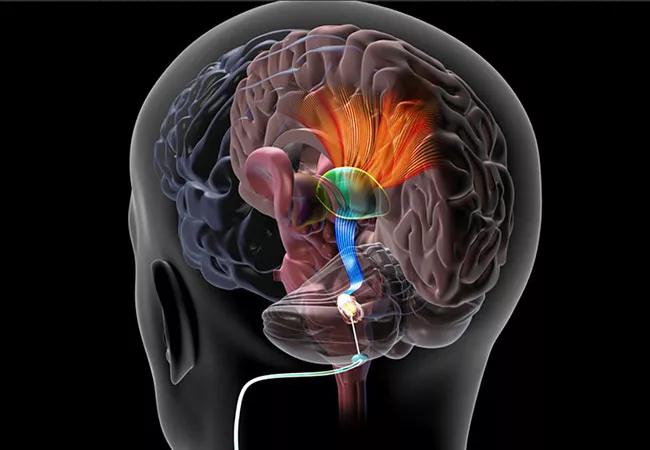
Targeting the dentate nucleus with deep brain stimulation (DBS) was safe and feasible for promoting post-stroke rehabilitation in a first-in-man study. So reported principal investigators Andre Machado, MD, PhD, and Kenneth Baker, PhD, in a late-breaking abstract presentation at the annual meeting of the Congress of Neurological Surgeons (CNS) on Oct. 20.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Treatment response in the phase I EDEN trial of dentate nucleus DBS for upper extremity hemiparesis from stroke was encouraging, enabling the procedure to advance to a phase II randomized controlled trial to evaluate safety and efficacy, the investigators concluded.
“We hypothesized that stimulating the dentatothalamocortical pathway, which connects the cerebellum and the cortex, would facilitate the spared perilesional cortex following ischemic stroke,” says Dr. Machado, Chair of Cleveland Clinic’s Neurological Institute. “We further proposed that this stimulation, when paired with physical training, would promote greater functional restoration than could be achieved with physical training alone. That is what we observed in this phase I study, as patients with even minimal residual distal function responded well.”
The findings build on more than a decade of preclinical work led by Dr. Machado and Dr. Baker (Neurosurgery. 2013;73:344-353) showing that DBS of the dentate nucleus enhanced perilesional excitability along with perilesional motor cortical reorganization and synaptogenesis. “These results show that the effects seen in our preclinical models appear to translate to humans. They argue for further investigation in larger patient samples.”
The EDEN trial (Electrical Stimulation of the Dentate Nucleus for Upper Extremity Hemiparesis Due to Ischemic Stroke) (NCT02835443) was a single-arm, open-label study conducted entirely at Cleveland Clinic. It enrolled 12 patients with chronic, moderate to severe hemiparesis of the upper extremity following unilateral middle cerebral artery stroke 12 to 36 months previously.
Advertisement
All patients began supervised physical rehabilitation — i.e., physical and occupational therapy — prior to implantation of a DBS lead at the dentate nucleus contralateral to their stroke lesion. After implantation, patients underwent physical rehabilitation for two months followed by a month of DBS programming over several sessions.
“All patients had three months of structured rehabilitation before the stimulation was turned on, to maximize the benefit to be achieved from rehabilitation alone,” Dr. Machado explains.
This was followed by at least four months of combined rehabilitation therapy and DBS. The study’s adaptive design allowed for extension beyond four months if patients continued to show month-over-month improvement.
Treatment response was defined as an improvement of 4.5 points or more on the Fugl-Meyer assessment of upper extremity function (FMA-UE). Additionally, the investigators evaluated event-related EEG and local field potentials perioperatively.
All 12 patients completed the study. There were no deaths, hemorrhages, infections or other major perioperative complications. The first three patients experienced DBS-related nausea in the first postoperative days. “This appeared to be related to how we placed the electrodes, so we changed that and subsequent patients had no nausea,” Dr. Machado notes.
Treatment response (≥ 4.5-point improvement on the FMA-UE) was achieved by nine of 12 patients. Mean FMA-UE improvement was 11.8 points (± 7.1 SD). Among the seven patients who entered the study with at least minimal distal motor function, the mean improvement was 16.4 points (± 3.9 SD) and was associated with significant improvement in activities of daily living (ADLs).
Advertisement
“This suggests that patients who have a bit of the neuronal pathway preserved offer us more to work with,” Dr. Machado observes. “There appear to be some neurons surviving that the stimulation and physical training can activate and boost.”
Follow-up continued for up to eight months for some patients, in order to capture cumulative functional improvement prior to plateauing.
Additionally, perioperative stimulation of the dentate nucleus combined with EEG revealed that DBS was associated with topography- and frequency-specific modulation of movement-related cortical activity, the investigators reported. They were also able to study the activity of the dentate nucleus during movement and movement planning. “This is the first reported direct investigation of movement-related local field potentials in the human dentate nucleus,” Dr. Machado notes.
The quality-of-life implications for study participants who responded to therapy have been significant. At the CNS meeting, Dr. Machado shared a video of a patient throwing a ball with her affected hand. “Prior to DBS and physical training, this patient was unable to unclench her hand and release a ball,” he explains. “Now she can coordinate all the movements needed to throw — extending and opening the fingers, extending the wrist and so forth — and execute them in an organized fashion.”
This ability has translated to ADL improvements for this patient such as the ability to put dishes away and tend to countless household tasks. Additional examples include a patient who has regained the ability to write messages using a marker and another who can buckle his pants again, enabling him to independently visit restrooms in public.
Advertisement

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/a588ee8b-a49e-4e45-9825-ef5bc485d041/21-NEU-2429063-CQD-Inset-800x580-1_jpg)
Photo of an EDEN study participant completing a grasping task with his affected arm during a follow-up assessment.
The degree of mean FMA-UE improvement achieved in the study — nearly triple the clinically meaningful threshold of 4.5 points — surprised the investigators. “We were not expecting this magnitude of functional recovery in phase I testing,” Dr. Machado says.
In the wake of these findings, Cleveland Clinic is planning a randomized, sham-controlled study of dentate nucleus DBS in up to 40 post-stroke patients. Dr. Machado says recruitment will be limited to patients with at least modest residual distal upper extremity function, in view of the superior response in this patient subgroup. He adds that the next study will also incorporate refinements in implantation techniques adopted over the course of the phase I study.
“About half of chronic stroke patients have a residual neurological deficit severe enough to require assistance with ADLs, even after extensive rehabilitative training,” Dr. Machado concludes. “We clearly need a tool that enhances the effects of physical training. DBS of the dentate nucleus shows encouraging promise to be such a tool. We are eager to investigate it further.”
The study was supported by the National Institutes of Health’s BRAIN initiative and funding from Enspire DBS Therapy.
Advertisement
Advertisement

Aim is for use with clinician oversight to make screening safer and more efficient

Rapid innovation is shaping the deep brain stimulation landscape

Study shows short-term behavioral training can yield objective and subjective gains

How we’re efficiently educating patients and care partners about treatment goals, logistics, risks and benefits

An expert’s take on evolving challenges, treatments and responsibilities through early adulthood

Comorbidities and medical complexity underlie far more deaths than SUDEP does

Novel Cleveland Clinic project is fueled by a $1 million NIH grant

Tool helps patients understand when to ask for help