Cleveland Clinic’s head of epilepsy surgery reflects on two decades of major progress
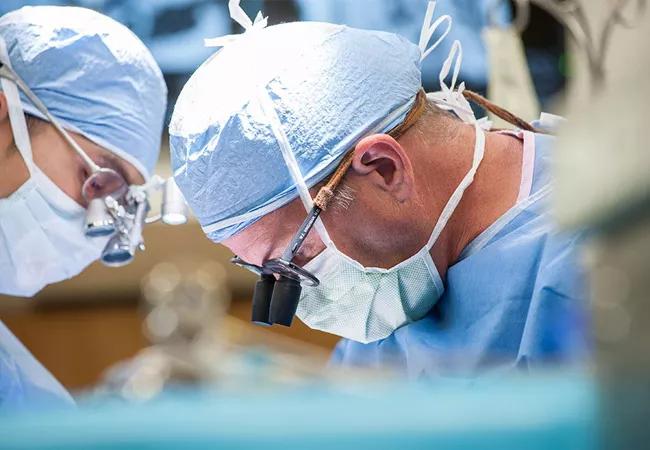
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/f98e4e45-0a4a-4920-8840-65bf367bdcf5/18-NEU-616-Bingaman-Career-Profile-650x450_jpg)
18-NEU-616-Bingaman-Career-Profile-650×450
The field of epilepsy neurosurgery has advanced dramatically in recent years, bringing a substantially greater chance of cure to the 1.2 percent of the U.S. population with this often devastating condition.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
William Bingaman, MD, Head of the Section of Epilepsy Surgery at Cleveland Clinic, has been in the forefront of the field since his appointment to Cleveland Clinic’s staff in 1997. Consult QD asked Dr. Bingaman (shown in surgery above) to reflect on the evolution of epilepsy neurosurgery and speculate on what may come next.
Q: Can you outline how neurosurgery for epilepsy has changed in your 20-plus years of practice?
A: I can go back way further than 20 years! Epilepsy surgery has been around since at least Neolithic times, when holes were drilled in people’s skulls with primitive tools to try to release evil spirits.
In modern times, epileptogenic scars and lesions potentially amenable to surgery could be identified by CT starting in the 1970s, and then more clearly by MRI a decade later. The 1.5-tesla (1.5T) MRI was the benchmark for MRI quality in the 1980s; since 2014, Cleveland Clinic has had the ultra-high-field 7T MRI scanner [detailed in a previous ConsultQD post], enabling visualization of ever more subtle lesions.
Capabilities increased enormously with the adoption of the subdural grid in the early 1980s, involving the internal placement of EEG electrodes. The technique has definite limitations — it requires a large incision, craniotomy and an often extended hospital stay — but it allowed physicians for the first time to identify epileptogenic foci not apparent by imaging.
In 2009, Cleveland Clinic became the first U.S. institution to start using stereoelectroencephalography, or SEEG, a minimally invasive technique to implant depth electrodes to localize seizure foci. SEEG has now largely replaced the use of subdural grids.
Advertisement
Today we have an array of anatomic and metabolic imaging capabilities at our fingertips, including SPECT, PET and MEG, to help determine the best management strategy and guide the neurosurgeon. There’s never been a single test that can definitively identify an epileptogenic focus; we need data from many tests combined with the clinical picture. Having the hospital resources to gather this information, as well as a team of experts to analyze the whole picture and the latest surgical capabilities, is critical to success. This involves large costs and a huge commitment. There are not many institutions other than Cleveland Clinic where all these components are in place.
Q: How does Cleveland Clinic’s epilepsy surgery program compare with those at other centers?
A: Cleveland Clinic has the largest epilepsy surgery practice in the world, performing more than 250 adult and 100 pediatric epilepsy surgeries annually. We are fortunate to have a large epilepsy team with national leaders in the field, helping us attract difficult cases from all over the world.
I am one of a handful of specialists in hemispherectomies, performing about 30 to 40 of them annually, with a career count of some 400. At Cleveland Clinic we have never had a pediatric death resulting from this procedure, which is reserved for the severest cases.
Thanks to the foresight of Dr. Toby Cosgrove during his tenure as Cleveland Clinic’s CEO and President, all of our institutes have gathered statistics for decades on surgical procedures and patient outcomes, and these are reported annually. We may well have the most complete and long-standing outcomes data on epilepsy anywhere [see examples here and here]. These data help us to continuously fine-tune our practices based on evidence.
Advertisement
Beyond that, I look around every day and see incredible people who are smart, dedicated and caring. Patient care is at the forefront at every level and step, from hospital greeters who help patients find their way around, to the support provided to families during the extended rehabilitation required for children. We offer a top-notch complete package, which is what makes Cleveland Clinic a world hub for epilepsy treatment.
Q: What’s the most important need for improvement in the field?
A: Epilepsy surgery is vastly underutilized in this country. Probably about 1 million patients who could benefit do not get the chance. After a patient fails two antiepileptic medications, he or she should be referred to a center capable of performing epilepsy surgery.
Q: What excites you about the future?
A: I envision a time when we’ll have more definitive tests that are completely noninvasive as well as a better understanding of neural networks to enable us to precisely pinpoint lesions. Maybe future surgeons will be able to cut one “wire” rather than take out a part of the brain.
If this seems pie-in-the-sky, let me tell you about the newest crop of residency candidates we just interviewed. I have never seen a brighter group. Their understanding of new technologies and information processing makes them speak a language that my generation can barely fathom! I predict that they will usher in a whole new era of epilepsy care.
Advertisement
Advertisement
Despite safety concerns and mixed trial results, experts see potential for this indication
Experts endorse a push to improve prevention and treatment following repetitive head injury
A population with very high lifetime risk presents care challenges and pathophysiologic insights
Two Cleveland Clinic neurologists review biomarker advances, targeted therapies and unresolved clinical challenges
Data-driven segmentation approach shows promise for seizure characterization with utility for clinical decision making
Alzheimer’s studies delve into preventing and modifying the disease’s trajectory and impact
Study finds broadly similar outcomes between MIS and open surgical approaches
System uses clinical data routinely collected at clinical visits