Use of MRI adds to cost but remains cost-effective due to higher sensitivity
Population-wide screening of middle-aged adults for nasopharyngeal carcinoma (NPC) is cost-effective in southern China, where NPC is endemic. A two-step strategy first employing Epstein-Barr virus (EBV) serology, and if positive, followed by nasoendoscopy, magnetic resonance imaging (MRI) or MRI with nasopharyngeal polymerase chain reaction (PCR) for EBV are the most cost-effective strategies, according to research presented at the 2023 ASTRO annual meeting.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
These conclusions are derived from a secondary analysis of the Guangdong cluster-randomized controlled trial (NCT00941538), in which nearly 360,000 residents 30 to 69 years old living in 16 cities in southern China were randomly allocated to NPC serologic screening or a control group. This study showed that over a 10-year period, EBV serologic screening may reduce NPC mortality in high-risk populations.
In the current study led by Jacob Miller, MD, Assistant Professor of Radiation Oncology at Cleveland Clinic Taussig Cancer Institute, six high-risk populations living in two provinces in southern China (Guangdong and Guangxi) were assessed based on screening costs and quality-associated life-years (QALYs) gained associated with 12 different screening strategies, each of which were contingent on the results of anti-EBV IgA serology. For each strategy and population, the investigators evaluated the incremental cost-effectiveness ratio (ICER), defined as the incremental cost per incremental quality-adjusted life-years per screened subject. A willingness to pay (WTP) threshold of 1.5 times the per-capita gross domestic product (GDP) was used to assess cost-effectiveness.
“The incidence of nasopharyngeal carcinoma in southern China is the highest in the world, so it makes sense to screen for this cancer to try to detect it at an early stage,” says Dr. Miller. “We demonstrated that in these six cities, whose population is nearly the population of the United States, NPC screening is cost-effective in both men and women, and screening tended to be cost-effective from approximately age 40 until age 60, which is relevant because these are the ages of peak NPC incidence. We also observed that more cases could be detected using nasopharyngeal MRI. While MRI increases the cost of screening, it remains cost-effective.”
Advertisement
The result resulted in the following findings:
“Four screening approaches were most competitive,” says Dr. Miller. The least expensive approach was EBV serology plus endoscopy. More cases at a slightly higher cost could be detected by combining serology, endoscopy and MRI. MRI utilization could be reduced while maintaining screening effectiveness by reserving its use to individuals found to have EBV DNA on a nasopharyngeal swab.
Advertisement
“Each strategy performs very well in these populations within the local economic constraints,” Dr. Miller says. “They have differing advantages depending upon the public health perspective. For hospitals that may not choose to use MRIs for screening purposes, serology plus endoscopy is a good alternative. If the goal is to maximize the number of lives saved, MRI could be added to maximize sensitivity. Nasopharyngeal swabs can be used to triage MRI use.”
These results are applicable only to southern China. Further research is warranted to study high-risk populations in other regions, where incidence rates, available resources and public health priorities may differ, Dr. Miller believes.
Advertisement
Advertisement

Not if they meet at least one criterion for presumptive evidence of immunity

Findings challenge the current diagnostic criteria for congenital Zika syndrome, expanding the definition beyond skull or brain abnormalities

Chemicals in e-cigarettes weaken the epithelial barrier in airways
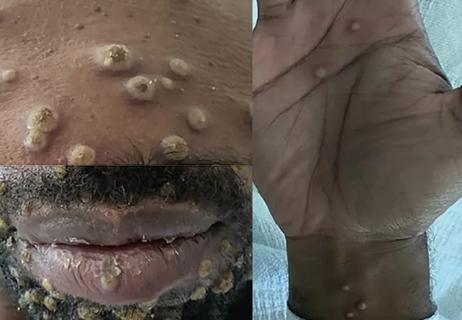
Persistent rectal pain leads to diffuse pustules
Anti-viral immunity identified a novel mechanism in necroptosis

Evidence-based recommendations for balancing cancer control with quality of life

Screening also found to be cost-effective
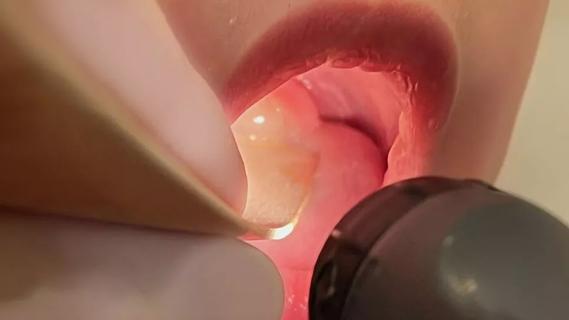
Prompt surgery was necessary when symptoms drastically increased