Enabling them to cough reduces their pneumonia risk
There are approximately 400,000 patients with multiple sclerosis (MS) in the United States. A significant number are not able to produce an effective cough to clear airway secretions, due to impairment of the central nervous system controlling the respiratory muscles. The inability to effectively cough elevates the risk of pneumonia.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Cleveland Clinic’s Director of Rehabilitation Research, Vernon Lin, MD, PhD, found that a technique called functional magnetic stimulation (FMS) improves respiratory muscle conditioning and coughing in patients with chronic spinal cord injury (SCI). Dr. Lin and his team are now applying the technique to patients with expiratory muscle dysfunction (including abdominal muscle weakness) due to MS.
“Expiratory muscle strength in patients with MS is significantly lower ‒ 27 percent to 74 percent of predicted ‒ than in normal subjects,” says Xiaoming Zhang, PhD, of Cleveland Clinic’s Department of Physical Medicine and Rehabilitation. “This can have a deleterious effect on their health, and they are more prone to develop pneumonia, which can be fatal.”
FMS is a painless, noninvasive technique that activates targeted muscles by stimulating corresponding spinal nerves where they exit the spinal cord. For patients with SCI and MS, FMS may substitute as a passive form of neuromuscular exercise.
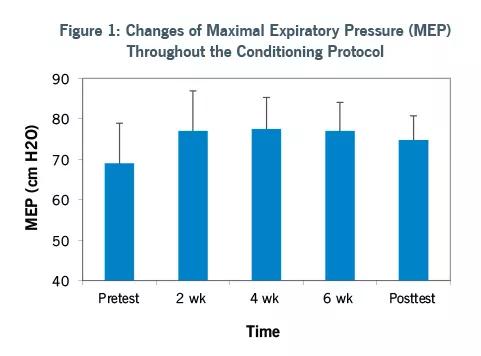
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/f98780e5-6d0f-4f3c-8aa9-87c62f78d4d2/LinZhang-fig1_jpg)
“Our laboratory has demonstrated the efficacies of FMS in improving physiological functions for patients with SCI, including improving coughing, breathing, bladder emptying, gastrointestinal motility and fibrinolysis, resulting in prevention of deep venous thrombosis,” says Dr. Zhang. “We are very optimistic that FMS will prove to be an effective tool for conditioning the expiratory muscles and improving quality of life in patients with MS.”
Functional magnetic stimulators consist of two components: a pulse generator producing discharge currents of 5,000 amps and a stimulating coil producing magnetic pulses with field strength of 2 Tesla and duration of about 250 μs. The magnetic field induces an electric field that excites neurons.
Advertisement
Placement of the coil varies with the therapeutic goal. In previous studies of FMS in SCI, lower thoracic spinal nerve stimulation resulted in maximal stimulation of expiratory muscles. Four to six weeks of conditioning of these expiratory muscles led to significant improvement in their voluntary expiratory functions, such as airway pressures, volumes and flow rates.
To study the effects of FMS in MS patients, researchers placed the center of the coil at the T9 spinous process and activated the stimulator for 20 minutes per day. The therapy was provided five days a week for six weeks, with stimulation intensity gradually increased from 40 percent to 70 percent of maximal capacity.
Pulmonary function tests performed at baseline and every two weeks measured maximal expiratory pressure, peak expiratory flow and expiratory reserve volume. The researchers observed continual improvements. At the end of the six-week study protocol, patients experienced a 20 percent increase over baseline in expiratory muscle strength, as measured by pressure.
“This increase is significant and may prevent pneumonia,” says Dr. Zhang. “However, these results are preliminary and will be used to apply for external funding for a more comprehensive study. When FMS units can be used at home, patients with MS may benefit from a more long-term and more convenient way of stimulating their respiratory muscles.”
Dr. Lin is Cleveland Clinic’s Director of Rehabilitation Research. Dr. Zhang is a Research Engineer in the Department of Physical Medicine and Rehabilitation.
Advertisement
Advertisement

Aim is for use with clinician oversight to make screening safer and more efficient

Rapid innovation is shaping the deep brain stimulation landscape

Study shows short-term behavioral training can yield objective and subjective gains

How we’re efficiently educating patients and care partners about treatment goals, logistics, risks and benefits

An expert’s take on evolving challenges, treatments and responsibilities through early adulthood

Comorbidities and medical complexity underlie far more deaths than SUDEP does

Novel Cleveland Clinic project is fueled by a $1 million NIH grant

Tool helps patients understand when to ask for help