Training initiative leads to new workforce redeployment resources for all providers
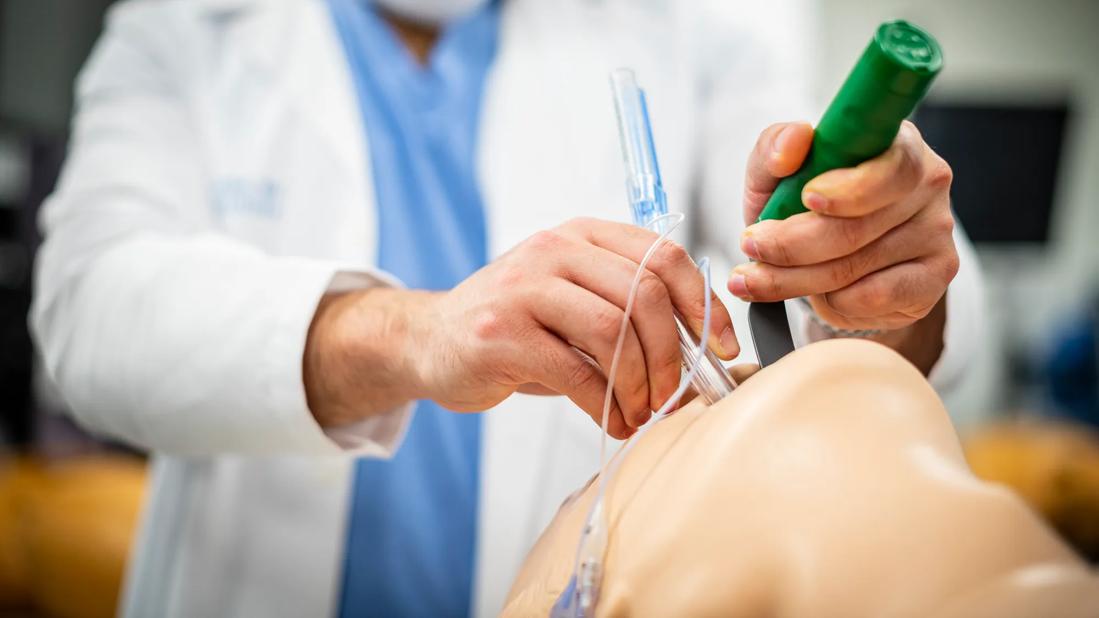
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/ceaa0764-4b90-4c26-8afa-b76ae4f6b6a4/PAI_2633916_01-19-21_129_SG-jpg)
1_650x450-Educational-Opportunities-Pandemic
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Since the earliest days of the COVID-19 pandemic, our lives have been inundated with news of hospital systems caring for overwhelming numbers of patients with acute respiratory failure and multiorgan system dysfunction. As cases peaked in China and then in Europe, it was as if a light switch flipped, instantly pausing all normal activity in our local environs. Beyond the abrupt halt of virtually all aspects of civilian life, the machinations of routine graduate medical education also seemed to halt. The usual humdrum of case conferences, journal clubs and pro-con debates were no match for the juggernaut of this pandemic. As the virus spread, Cleveland Clinic began an aggressive campaign to prepare for the possibility that what was unfolding an ocean away might soon take hold in the United States.
As the Critical Care fellowship program director, my initial instincts were to continue our educational programming throughout this planning process. I saw it as an attempt to maintain some sense of normalcy for our fellows. But as I did so, two things quickly became apparent. First, I was ignoring the key principles of adult learning theory in these efforts. Chief among them was to make learning relevant to the needs of our learners. Discussing the mechanisms of Tylenol toxicity in acute liver failure didn’t seem relevant to the moment. Second, we began to understand that COVID-19 wasn’t going to be a short-term nuisance. Despite extraordinary measures to prevent community spread in Ohio, officials were still predicting that as many as 2,500 ICU beds at Cleveland Clinic might be needed. Our approach to education, as with all things, had to be fundamentally different.
Advertisement
The solution to this conundrum came in the form of an invitation. As part of Cleveland Clinic’s pandemic preparedness plan, a massive redeployment of physicians and advanced practice providers into inpatient and medical intensive care units was planned. The natural question was how to give providers the necessary hands-on and didactic training to prepare them for this endeavor. I and a group of other educators from the Respiratory Institute were invited to lead this effort. More importantly, it was immediately apparent that we had an opportunity, not only to reengage our fellows in robust educational and leadership endeavors but to attract multiple learner groups across the enterprise if we did things correctly.
We immediately assembled a multidisciplinary team from the Respiratory Institute, Anesthesia Institute, Cleveland Clinic Lerner College of Medicine, Department of Internal Medicine, Center for Technology-Enhanced Knowledge and Instruction (cTEKI), and the Office of Interprofessional Education to create a web-based learning platform with up to date, relevant, and easy-to-access information germane to the position where a provider might be deployed. The group met and quickly identified basic providers who might need these resources. These included: training for current ICU providers, training for providers with limited ICU experience who might be redeployed to the ICU setting, and training for providers with limited inpatient medicine experience who might be redeployed to a non-ICU inpatient setting.
Advertisement
Once we identified provider groups, it became clear that each group would need both pre- and post-deployment resources. Leaders from our planning committee coordinated with volunteers from the Cleveland Clinic Lerner College of Medicine, the Center for Advanced Skills Training, the Internal Medicine Residency Program and Hospital Medicine Department to develop content. The content was loaded on learning platforms with the help of the Office of Interprofessional Education and the MyLearning Systems Resource Center. The content covers the following areas:
Advertisement
Access Cleveland Clinic’s entire suite of educational resources for COVID-19 care and workforce redeployment here.
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/5a4e6112-0da7-4b7f-b0f6-a7bbd99ff9cd/1_805x-Inset-Education-Resources_jpg)
Despite initially lamenting the temporary postponement of most of our traditional educational venues, I take great pride in the education and leadership opportunities this process has bestowed upon our fellows. Our fellows have been involved in every step of this process. They served as content mentors to help review and advise medical student authors from Cleveland Clinic Lerner College of Medicine as they built pre-deployment modules for future critical care and non-critical care providers. During the hands-on skills training, fellows filled the bulk of our teaching roles, reinforcing and drilling techniques fundamental to common procedures. In creating the post-deployment “Just in Time” guides, fellows again stepped up to serve as writers, editors and mentors for internal medicine residents.
As we now move from “build mode” to “maintenance mode,” our learning platform lives on web-based servers that offer users streamlined information on COVID-19 and non-COVID-19 patient care. Beyond the build, fellows continue to lead the way. A small committee, led by one of our chief fellows, is engaged in ensuring continued content quality and updates for the COVID-19 redeployment platform.
Despite the horrific toll, anxiety, social and economic ruin that the COVID-19 pandemic has produced, it has opened my eyes to the opportunities a crisis can also provide. In changing the paradigm of learning, our fellows have enhanced their critical care skills through a method more consistent with adult learning theory. But beyond this they have also espoused a core tenant of Cleveland Clinic’s mission. By sharing what they have learned about ICU and non-ICU best practices as well as COVID-19 specific care of patients with respiratory illnesses, the meaning of the words, “better education of those who serve” is abundantly visible.
Advertisement
About the author
Dr. Chaisson is the Director of the Critical Care Medicine Fellowship Program at Cleveland Clinic’s Respiratory Institute.
Advertisement
Patients report improved sense of smell and taste
Clinicians who are accustomed to uncertainty can do well by patients
Unique skin changes can occur after infection or vaccine
Cleveland Clinic analysis suggests that obtaining care for the virus might reveal a previously undiagnosed condition
As the pandemic evolves, rheumatologists must continue to be mindful of most vulnerable patients
Early results suggest positive outcomes from COVID-19 PrEP treatment
Could the virus have caused the condition or triggered previously undiagnosed disease?
Five categories of cutaneous abnormalities are associated with COVID-19