Investigator speaks to potential applications beyond stroke
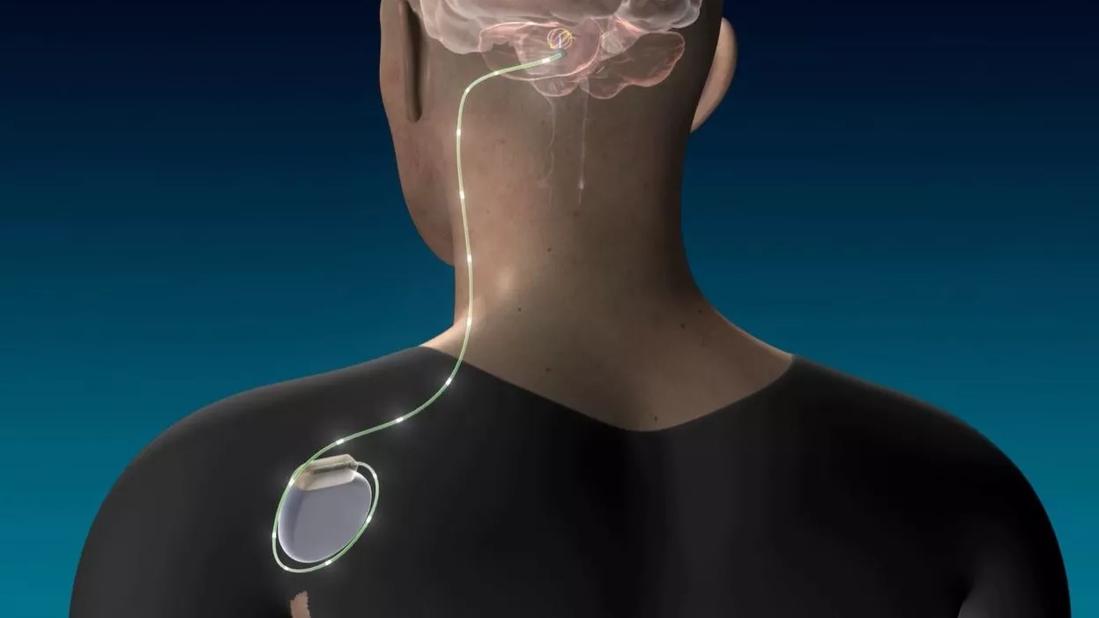
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/89ee648d-08c5-4a1a-97c6-77a61b1c9995/dbs1-jpg)
DBS
As previously reported on this blog, Cleveland Clinic researchers have launched the first clinical trial to examine the use of deep brain stimulation (DBS) to promote motor function recovery in disabled stroke survivors. The trial, launched in 2016 (a DBS device was implanted in the first patient in December), was awarded nearly $5 million in funding from the NIH’s Brain Research through Advancing Innovative Neurotechnologies (BRAIN) initiative.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The trial’s lead investigator, neurosurgeon Andre Machado, MD, PhD, recently shared some insights on the trial’s clinical implications in this video post. Dr. Machado explains the essentials of the trial, which patients are candidates, and how DBS for stroke recovery differs from neuromodulation for movement disorders.
“Our primary hypothesis is that by applying DBS to the connections between the cerebellum and cerebral cortex, we can facilitate the plasticity that occurs in the cortex around the stroke and thereby promote recovery of function beyond what physical therapy alone can do,” Dr. Machado notes. “We need more and better options to help the many patients who remain chronically disabled after a stroke.”
Now co-investigator Kenneth Baker, PhD, assistant staff in Cleveland Clinic’s Department of Neurosciences, speaks to some of the scientific implications of the study’s attempt to stimulate the brain’s dentatothalamocortical pathway to restore lost motor function. He also explains how Cleveland Clinic’s recent NIH BRAIN grant award is supporting the team’s work.
“We know that deep cerebellar stimulation promotes motor recovery in a preclinical model of cortical stroke,” says Dr. Baker. “Our goal is to advance this therapy to promote recovery of motor function in humans. This has the potential to be a significant advancement for the field.”
Check out his insights in the video below.
Video content: This video is available to watch online.
View video online (https://www.youtube.com/embed/EbJDJSQhxV8?feature=oembed)
Advertisement
Advertisement
How to use? Consider starting during the acute attack and seek patient preferences for chronic use
Quantitative imaging adds diagnostic value beyond 3T MRI in nearly half of patients
Expert shares insight on intrathecal baclofen pumps to treat spasticity
Opportunities and impacts of a growing surgical approach
Despite safety concerns and mixed trial results, experts see potential for this indication
Experts endorse a push to improve prevention and treatment following repetitive head injury
A population with very high lifetime risk presents care challenges and pathophysiologic insights
Two Cleveland Clinic neurologists review biomarker advances, targeted therapies and unresolved clinical challenges