Caregiver Catalyst Grants encourage innovation
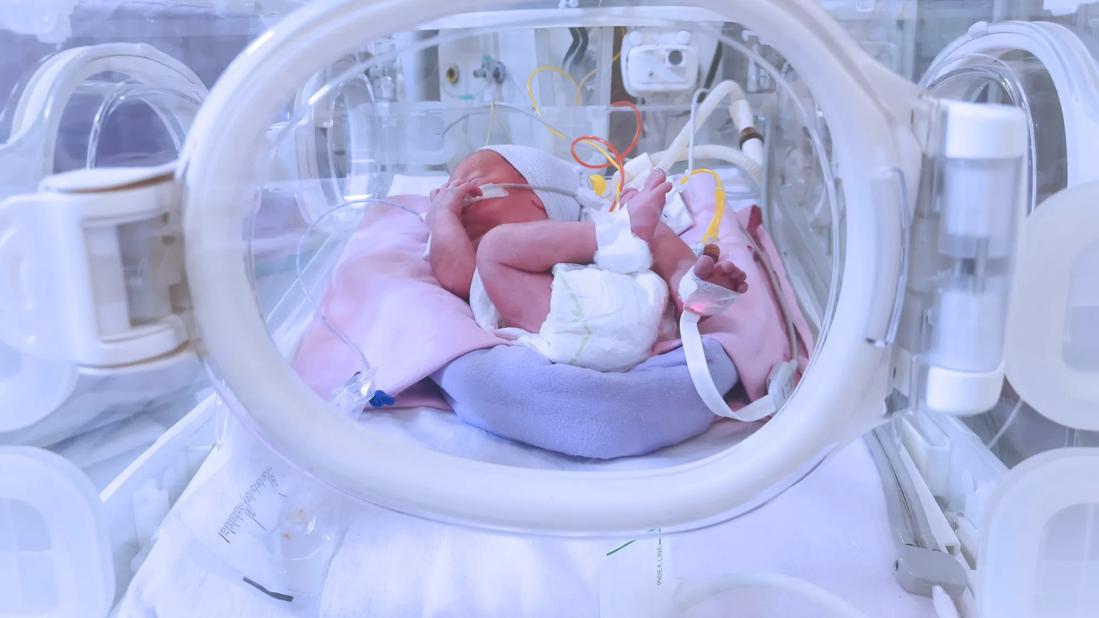
A NICU stay can have negative effects on infants born prematurely and their families. First Voices — a new project developed by Child Life Specialist Jessica Timms, MS, CCLS — aims to reduce that stress and promote a nurturing environment for families separated by a NICU stay.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Although NICUs provide lifesaving interventions, they are not natural environments for neonates and their families, which can negatively impact development and bonding.
“Around 15% of premature babies in the NICU suffer from developmental delay or learning disability during childhood,” says Hany Aly, MD, Chair of Neonatology at Cleveland Clinic Children’s. “This disability cannot be related to any one disease — it’s the experience in the NICU. Babies definitely feel the environmental stress, whether it is due to excessive light and noise, a lack of sleep or pain procedures. Additionally, babies born prematurely are deprived of the natural stimulation of the uterine environment. Babies definitely feel when their moms are not around.”
“Having a child in the NICU is also stressful for parents, who may feel anxiety about their baby’s health and — to some extent — helpless and unable to care for their baby,” Dr. Aly continues. “When a mom finds a way to get involved (e.g., expressing breast milk, reading stories to the baby, skin-to-skin contact), it reduces stress for all parties. First Voices allows NICU parents to participate in their baby’s care when they can’t physically be on the unit, and may help relieve the stress of delivering a premature baby.”
“We use parents’ voices in order to mimic the natural environment of the uterus,” Timms says. “In the third trimester, the baby’s auditory cortex is developing, and sounds coming from outside the uterus enhance this development. Studies have shown that parents’ voices can enhance their baby’s neurological functioning, increase their quiet alert state and optimize attachment, even when the family cannot be at the bedside. Just because a child is born early does not mean they should not or cannot have the same opportunities for development as babies born at term. Three hours per day of a mom’s voice or heartbeat can help with this.”
Advertisement
The auditory cortex develops around 28 weeks gestation, at which point babies begin to hear their mother’s voice and heart beat in utero.
“I thought we might be able to use recorded parental voices to bridge the gap between when the auditory cortex develops and when babies are discharged from the NICU,” Timms says. “With this program, babies receive auditory stimulation, and begin to develop an attachment to their parents’ voices as they would if they weren’t in the hospital.”
Timms says she relies on NICU nurses and social workers to help identify parents who might benefit from the First Voices program. Participating parents select a book from the library the grant helped to create, and then read the book into recording equipment. Parents also sometimes sing songs or record personal messages for their babies. The recordings are played in the isolette at intervals throughout the day.
“We use First Voices for the babies in many different instances. In stressful times or if they’re just a little bit fussy, it does have a calming effect,” says Julie Gamary, BSN, NICU Nurse Manager.
“We developed the library because we didn’t want parents to wonder what they should say to their baby, or how they should say it. Reading stories seems to come naturally. It also helps us segue into talking to parents about literacy and the importance of reading books to their children, even after discharge. After the recordings are made, we’ve had parents sit at the bedside and read to their babies. Parents might say, ‘I read books to you when you were in the NICU, and now that we’re home I get to read to you while you’re in my arms,’” Timms notes.
Advertisement

Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/90517060-3666-4c43-9749-a833097149d4/805x-Parental-Voice_jpg)
Timms received a Cleveland Clinic Caregiver Catalyst Grant to create the new program, which is seeing encouraging levels of participation. “Our original goal was to increase participation by 10% from 2019, which we’ve already seen in just two months of recruitment efforts. I expect recruitment to continue to improve now that NICU caregivers are comfortable with the program. Additionally, we’ve trained nurses on the recording equipment, which should make participation more convenient,” says Timms.
Start-up funds are essential to innovating care. “We wouldn’t be able to do something that’s so beneficial to the babies and their development without the help of giving,” Gamary notes.
Cleveland Clinic’s Caregiver Catalyst Grants pool the generosity of thousands of Cleveland Clinic donors and direct their collective giving to a fund allocated to caregiver’s ideas. It is a distinct way for philanthropic gifts of every size to make an immediate impact, as the funded projects must demonstrate outcomes within 12 months after the caregivers receive the grants. Since the program’s inception in 2018, more than $3 million have been awarded to help support 81 ideas.
Advertisement
Advertisement

Findings hold lessons for future pandemics

One pediatric urologist’s quest to improve the status quo

Overcoming barriers to implementing clinical trials

Interim results of RUBY study also indicate improved physical function and quality of life

Innovative hardware and AI algorithms aim to detect cardiovascular decline sooner

The benefits of this emerging surgical technology

Integrated care model reduces length of stay, improves outpatient pain management

A closer look at the impact on procedures and patient outcomes