Public health concerns mount as number of deaths increases
By Ellen Rome, MD, MPH, and Humberto Choi, MD
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
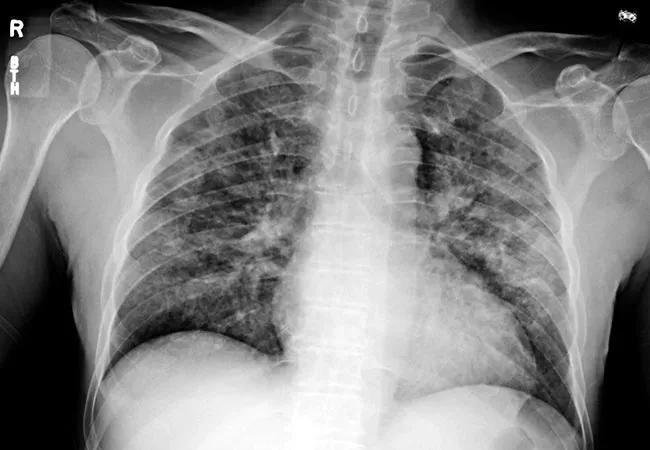
A young woman came to us at Cleveland Clinic reporting breathing difficulties. A CT scan showed inflammation in both lungs, but no signs of cancer or other sicknesses that typically cause this kind of inflammation. Only when the woman – in her twenties – explained that she had just started vaping two months ago did doctors ascertain the source of her problem.
E-cigarettes and vaping are relatively new, but many have thought of them as a harmless alternative to smoking. However, recent reports of serious respiratory illnesses likely tied to vaping are popping up across the country, including young patients being put on mechanical ventilators. The Centers for Disease Control and Prevention (CDC) reports approximately 380 possible cases across 36 states, including Ohio, and the U.S. Virgin Islands, as of September 12, 2019. Seven deaths have been reported, through September 17, 2019, potentially linked to vaping. Unfortunately, we have seen similar cases here at Cleveland Clinic.
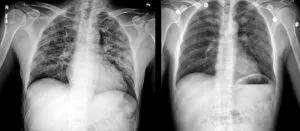
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/d845a625-c3fd-4075-af6f-42aeb93cd8b5/805x-Vaping-Inset-300x131_jpg)
Chest images from a patient who ended up in the ICU with suspected lung injury related to vaping. The images show improvement of lung opacities with no specific treatment other than avoiding exposure while in the hospital.
As these illnesses come into focus, physicians are quickly trying to learn more, as still little is known of the long-term effects of vaping. Along with these serious cases, anecdotal evidence reveals some of their impact mirrors that of traditional cigarettes.
In addition, the youngest group of vapers today have brains that are still developing incredibly critical functions such as self-control, emotional maturation and reward processing. Strong data suggests that nicotine exposure during teen years disrupts the brain’s neurotransmitter systems, leading to long-term changes in cognitive development and even decreased memory capacity.
Advertisement
The “vaping” craze surrounding e-cigarette use is also leading people, especially our youth, down the path of nicotine addiction.
As we know from decades of cultural experience and scientific research, once you begin using any nicotine-based product, it can be extremely difficult to stop. Our society is at a critical moment in which we need to learn from our history with cigarettes and act accordingly, especially with our future generations in mind.
Some may think vaping is a harmless alternative to smoking; however, the most popular e-cigarette on the market contains almost three times the nicotine as a single pack of cigarettes. Unlike cigarettes, which are smoked one-by-one and have a clear starting and stopping point, e-cigarettes can be puffed on continuously – further adding to the danger of addiction.
While it is true that these devices do not contain tar and tobacco, the high nicotine content gives an alarming number of teens and young adults their first exposure to the highly addictive stimulant. According to the 2018 National Youth Tobacco Survey, 78% of high schoolers have used e-cigarettes, as have 48% of middle schoolers.
To make matters worse, thanks to the alluring marketing tactics and flavors of e-cigarettes, America’s youth are – in many cases, unwittingly – becoming addicted to nicotine. A study from the Truth Initiative found that only about one-third of 12th graders are aware that Juuls, a brand of e-cigarettes, contain nicotine – and many are outraged when they learn the truth.
Advertisement
The CDC and the Food and Drug Administration (FDA) are now urging people who vape not to buy products off the street, and seek medical attention if they have trouble breathing or chest pain. But it is clear to us, as medical professionals, that our society must tackle the e-cigarette epidemic in the same manner as we have successfully fought traditional cigarettes.
Many of the tactics that worked so effectively on cigarettes can, and should, be deployed in the fight against vaping. Here are five proven avenues to cessation that should be enacted immediately:
Advertisement
We can, and should, put a stop to the rapid increase in vaping and e-cigarette use. Our society battled the scourge of cigarette smoking for decades. Let us take what we learned and apply it to this new form of nicotine addiction.
The lives of millions of teens and young adults may depend on us taking action … now.
Ellen Rome, MD, MPH, serves as Head of the Center for Adolescent Medicine at Cleveland Clinic Children’s Hospital and as a Professor of Pediatrics at the Cleveland Clinic Lerner College of Medicine of Case Western Reserve University. Humberto Choi, MD is a pulmonologist at Cleveland Clinic specializing in thoracic oncology and a medical intensivist. He is the Medical Director of the Respiratory Institute Smoking Cessation Program.
Advertisement
Advertisement

Findings hold lessons for future pandemics

One pediatric urologist’s quest to improve the status quo

Overcoming barriers to implementing clinical trials

Interim results of RUBY study also indicate improved physical function and quality of life

Innovative hardware and AI algorithms aim to detect cardiovascular decline sooner

The benefits of this emerging surgical technology

Integrated care model reduces length of stay, improves outpatient pain management

A closer look at the impact on procedures and patient outcomes