A closer look at subanesthetic intravenous ketamine infusion

As physicians look for nonopioid treatments to manage pain, various types of infusion therapies are being reassessed for efficacy. Intravenous ketamine infusion therapy has been used for difficult to treat chronic pain syndromes such as complex regional pain syndrome (CRPS). But it has been used cautiously because of a number of effects, including “dissociative” phenomenon, hallucinations, elevated blood pressure and possible liver and bladder injury.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Since the 1970s, ketamine’s primary medical use has been for general anesthesia, and it is now being used in intensive care and pediatric procedures, in emergency medicine and as a secondary treatment for certain psychiatric conditions, including depression.
“This medicine has been used before for pain, but because of its adverse effect profile, it was discouraged for a while,” says Cleveland Clinic Pain Management Specialist Jijun Xu, MD, PhD. “In recent years it is coming back as an option for refractory chronic neuropathic pain because it works on one of the key receptors that mediates nerve pain.”
CRPS is one of the most challenging clinical pain syndromes to treat, with amplification of pain signals in the central nerve system (or central sensitization). Dr. Xu says ketamine has been used around the world in different ways to treat CRPS, but to date there has not been a consensus protocol and there has been little research done. Over the last two years, Dr. Xu has been doing extensive research on the drug with support from the Reflex Sympathetic Dystrophy Association. CRPS was formerly known as reflex sympathetic dystrophy (or RSD).
In February, Dr. Xu and the research team published a paper titled “Intravenous Ketamine Infusion for Complex Regional Pain Syndrome: Survey, Consensus, and a Reference Protocol.” The objective of the research was to come to a consensus on the usage of ketamine for the treatment of CRPS and to put together a reference protocol for future studies.
Advertisement
Dr. Xu’s research included a survey of 351 medical professionals from around the world on how ketamine is used in their practice for treating pain associated with CRPS. The survey asked questions about inpatient and outpatient treatment, children vs. adults, safety and basic demographic information. In most cases, ketamine was used at subanesthetic doses with close management by nurses to avoid adverse events and improve outcomes for patients.
Patients were titrated to “drowsy to moderate sedation” or pain reduction by 50 percent using a numeric pain rating scale. Study participants agreed that pain rating was the primary measurement used to assess how fast the infusion should happen and its impact. Study results showed that duration of pain relief ranged from one day to six months, with the majority reporting pain relief from one to six months.
Dr. Xu says this consensus statement for inpatient and outpatient care serves as a starting point for statistical validation of formal guidelines and a more uniform approach to research protocols.
“Ketamine has great promise as a treatment for CRPS, but we need to be cautious,” says Dr. Xu. “We have to be careful about the dose, the duration of use, and the side effects. Current evidence indicates that short-term use of subanesthetic ketamine infusion under clinical supervision is safe, but we don’t know the long-term cognitive effects it could have. We need more data and must gather more extensive outcome measurements.”
The next step is to validate the safety and efficacy of ketamine through controlled clinical trials. “With more feedback, we can make it a treatment modality that is a safe and effective treatment for CRPS,” Dr. Xu concludes.
Advertisement
Advertisement

Researchers seek solutions to siloed care, missed diagnoses and limited access to trauma-informed therapies

Study participants also reported better sleep quality and reduced use of pain medications

Two-hour training helps patients expand skills that return a sense of control
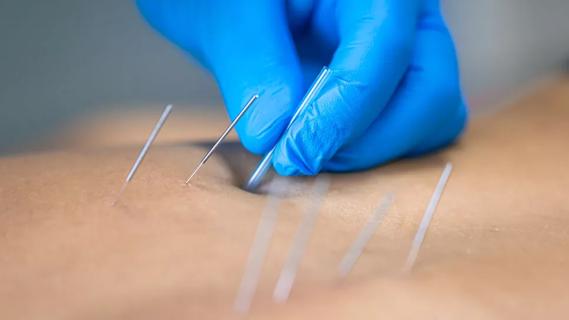
Program enhances cooperation between traditional and non-pharmacologic care

National Institutes of Health grant supports Cleveland Clinic study of first mechanism-guided therapy for CRPS
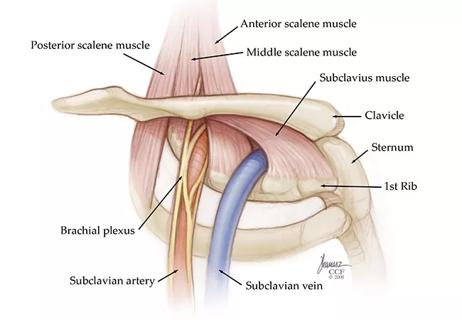
Pain specialists can play a role in identifying surgical candidates
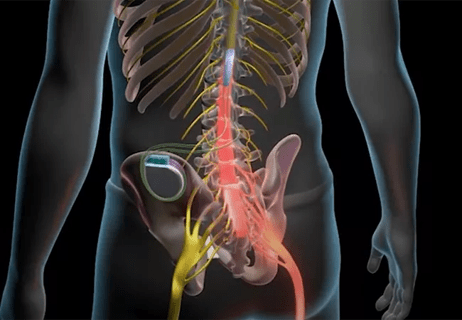
Individual needs should be matched to technological features
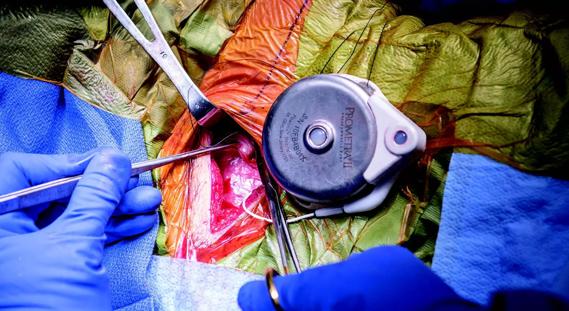
New technologies and tools offer hope for fuller understanding