Should sleep history be incorporated into routine neurological care?
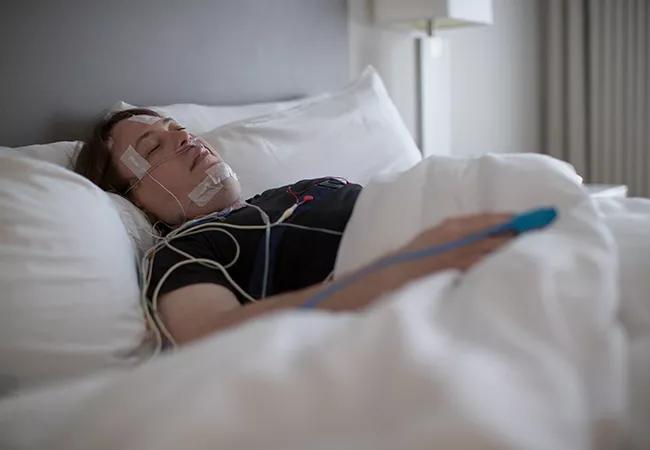
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/e2e598ff-7497-482d-896a-fbe3a1997c9f/18-NEU-817-Foldvary-Sleep-Neuro-650x450_jpg)
18-NEU-817-Foldvary-Sleep-Neuro-650×450
Both obstructive sleep apnea (OSA) and insomnia are found in a high percentage of patients with a variety of neurological diseases, according to new research from Cleveland Clinic investigators presented at the 2018 annual meeting of the American Academy of Neurology (AAN).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“These associations are of interest because there’s a vast body of literature showing that untreated sleep disorders are associated with worse disease-specific outcomes,” says senior investigator Nancy Foldvary-Schaefer, DO, MS, Director of Cleveland Clinic’s Sleep Disorders Center. “There is also evidence that treating sleep disorders improves neurological outcomes.”
In a previous study presented at the 2017 American Epilepsy Society meeting, Dr. Foldvary-Schaefer and colleagues found that treating OSA with continuous positive airway pressure (CPAP) therapy in patients with epilepsy led to better seizure control. In the new research, presented as a poster at the AAN meeting (see abstract here), they examined the association between sleep instrument scores and disease-specific outcomes across various neurological populations.
Using standardized instruments, the team performed a retrospective analysis of 19,052 adult initial outpatient visits to multiple centers within Cleveland Clinic’s Neurological Institute (psychiatry, brain tumor, movement disorders, cerebrovascular and epilepsy) from March 2015 to October 2016.
“We used the STOP instrument to detect sleep apnea symptoms and the Insomnia Severity Index (ISI) to detect significant insomnia symptoms,” Dr. Foldvary-Schaefer explains. High-risk OSA was defined as a STOP score ≥ 2 and significant insomnia as an ISI score ≥ 15.
The researchers found that one-third of neurological patients were at high risk for OSA and one-quarter had significant insomnia symptoms. Patients with STOP scores ≥ 2 were older and more likely to be male, while patients with ISI scores ≥ 15 were younger and more likely to be female.
Advertisement
“The highest prevalence of OSA was in the cerebrovascular disease population,” Dr. Foldvary-Schaefer reports, “which makes sense because stroke and cardiovascular disease have known associations with undiagnosed sleep apnea.” The prevalence of OSA was also higher in the epilepsy population, confirming the group’s previous work.
The highest prevalence of significant insomnia was in the psychiatry population, Dr. Foldvary-Schaefer continues, “which was also expected since depression and other psychiatric disorders are often linked with insomnia.” Significant insomnia was also associated with worse neurological status in movement disorder and epilepsy populations.
She notes that Cleveland Clinic is in a unique position to measure sleep outcomes across broad populations due to the Knowledge Program, a homegrown electronic data entry system for patient-reported outcomes integrated into the electronic medical record. The program was developed by the Neurological Institute over 10 years ago but is now used throughout Cleveland Clinic.
“When we presented data at a recent American Academy of Sleep Medicine meeting, other major institutions were in awe of our ability to capture so much patient-reported data,” says Dr. Foldvary-Schaefer. “The Knowledge Program allows for the collection of disease-specific outcome data and general health status measures from patients at every visit, improves patient care and provides incredible fodder for research. And because of the collaborative environment in our Neurological Institute, we’ve been able to gain buy-in from busy doctors and centers to gather sleep disorder data.”
Advertisement
Now that her team has acquired data on the extent of the problem — and they’re in the process of collecting data from other Neurological Institute centers — they hope to launch research to see if they can replicate the results of their study of CPAP in epilepsy patients in additional populations. “We’d like to investigate further to see if there is a role for sleep therapies on disease-specific outcomes in other neurological patients,” she says.
As a result of this research, Dr. Foldvary-Schaefer hopes neurologists will begin to recognize that a sleep history needs to be incorporated into the routine care of all neurological patients.
“Sleep impacts numerous neurological conditions, and treating sleep disorders can have trickle-down effects on the management of many of them,” she says. “The challenge is that most neurologists don’t have training in sleep disorders, but it’s actually simple to screen for them.”
For example, she says that assessing for the risk of OSA starts with asking patients just three questions:
“These three questions can identify a patient at high risk for OSA and might, for example, end up preventing a cerebrovascular patient from having a second stroke,” she explains. “Once identified as high-risk, patients can be referred to a sleep specialist for further evaluation and treatment.”
Advertisement
Advertisement
Two Cleveland Clinic neurologists review biomarker advances, targeted therapies and unresolved clinical challenges
Data-driven segmentation approach shows promise for seizure characterization with utility for clinical decision making
Alzheimer’s studies delve into preventing and modifying the disease’s trajectory and impact
Study finds broadly similar outcomes between MIS and open surgical approaches
System uses clinical data routinely collected at clinical visits
Newer protocols address testing, language and communication
Collaboration with AI startup promises to reshape neurocritical care monitoring at scale
Study looked at mobility measures and safety