Patients age 80 and older report similar satisfaction and pain relief as younger patients
Patients who had total hip arthroplasty (THA) at age 80 or older reported the same pain relief and satisfaction outcomes as patients ages 65-79, according to a recent study by Cleveland Clinic. Results of the study contradict common misconceptions about age and outcomes that may lead older patients to avoid THA.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
The volume of THA procedures has been increasing as the world population continues to age. Improved peri- and postoperative processes, including safer anesthesia and more integrated approaches to care, have made THA an appropriate procedure for octogenarian and nonagenarian patient populations.
Still, there is some hesitancy among surgeons and patients alike when considering THA for older adults, notes Nicolas S. Piuzzi, MD, Adult Joint Reconstruction Research Director in Cleveland Clinic’s Department of Orthopaedic Surgery.
“Our team used PROMs [patient-reported outcome measures] data to investigate THA outcomes in older adults, especially those over age 80,” says Dr. Piuzzi. “We hoped our findings would provide additional clarity about outcomes and support shared decision-making between patients and surgeons.”
The team studied patients who had a total of 4,257 primary THA surgeries between August 2015 and August 2018. Using PROMs data, the researchers reviewed pain, function and health-related quality of life metrics one year after surgery across three age groups.
Compared to their younger counterparts, patients age 80 and older experienced a similar improvement in hip disability and osteoarthritis outcome score (HOOS) pain and HOOS-PS (physical function shortform) metrics following THA.
Consistent with medical literature, researchers also found that the 80-and-older cohort had the highest incidence of:
As expected, one-year mortality rates also were highest in this group compared to younger groups, however the rate was lower than the general mortality rate for U.S. adults of the same age.
Advertisement
Dr. Piuzzi says that this study reinforces that age alone is not an exclusionary criterion for THA. Rather, he argues, it underscores the need for more tailored perioperative care plans and data-driven outcome prediction tools.
“We have to be mindful that age is not a disqualifier for THA,” he says. “Patients age 80 and older are reporting high levels of satisfaction. There might be more postoperative healthcare utilization, but we can address that by managing patients’ expectations and developing specific care paths.”
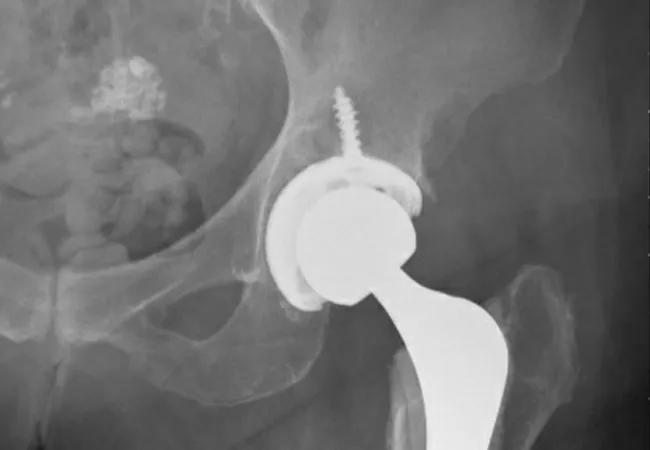
In his own practice, Dr. Piuzzi frequently sees good outcomes of THA in older patients. He recently treated a 90-year-old woman who presented with unilateral hip pain caused by severe arthritis (Figure 1). She reported difficulty going up and down stairs in her home and was at risk of falling. After the initial consultation, she decided to undergo primary THA. Nearly 12 months later, she has reported good outcomes and has resumed her daily activities without pain (Figure 2).
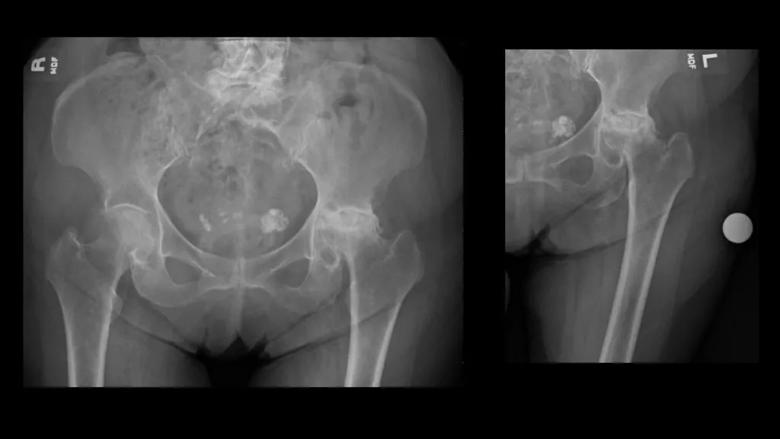
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/841ce347-499c-412b-94d0-3502cef6bd04/21-ORT-2060875-CQD-How-Old-is-Too-Old-Inset-1-1024x576_jpg)
Figure 1. Preoperative anteroposterior view of the pelvis and left hip, demonstrating advanced degenerative changes (severe osteoarthritis).
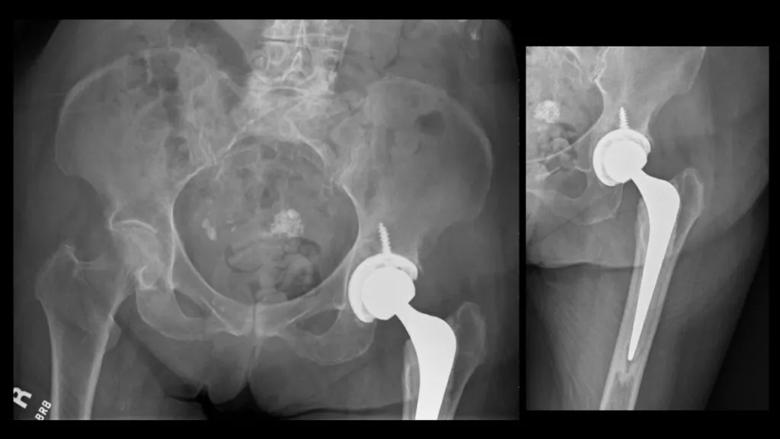
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/64395c31-e48e-4eab-bba8-5174b43213d2/21-ORT-2060875-CQD-How-Old-is-Too-Old-Inset-2-1024x576_jpg)
Figure 2. Postoperative anteroposterior view of the pelvis and left hip, showing a well-fixed and positioned cemented total hip arthroplasty.
According to Dr. Piuzzi, there are three factors to consider when evaluating a patient’s candidacy for THA: the patient, the healthcare team (including the surgeon) and the environment in which the patient will recover. Age is a factor when considering patient-level risks, but it’s not the only factor, he emphasizes. It should be part of a holistic evaluation.
Advertisement
“The continued advancement of personalized medicine will eclipse some of the outdated notions that age alone is a determinant in outcomes,” says Dr. Piuzzi. “We are heartened by the good outcomes we continue to see in the age-80-and-up patient population.”
Advertisement
Advertisement

How it’s similar but different from the direct anterior approach

Collaboration must cross borders and disciplines

Systematic review of MOON cohorts demonstrates a need for sex-specific rehab protocols

Should surgeons forgo posterior and lateral approaches?

How chiropractors can reduce unnecessary imaging, lower costs and ease the burden on primary care clinicians

Why shifting away from delayed repairs in high-risk athletes could prevent long-term instability and improve outcomes

Multidisciplinary care can make arthroplasty a safe option even for patients with low ejection fraction

Percutaneous stabilization can increase mobility without disrupting cancer treatment