Cleveland Clinic orthopaedic surgeons share their best tips, most challenging cases and biggest misperceptions
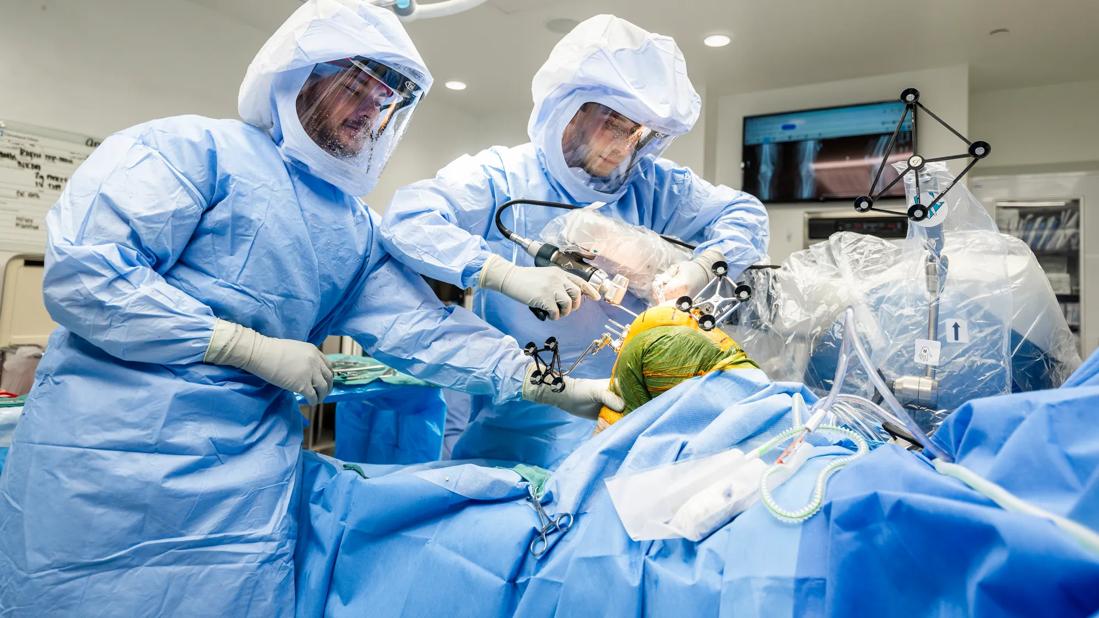
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/60858667-5671-4680-86fe-8a79683f3818/ORI_5833008_03-19-25_356_MLC)
Knee surgeons
Cleveland Clinic’s Department of Orthopaedic Surgery recently completed its 10,000th robot-assisted total joint replacement. Since 2016, Cleveland Clinic surgeons have been using robotic surgery systems to maximize precision and personalization in hip and knee arthroplasty.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“Robotics is here to stay,” says Nicolas S. Piuzzi, MD, Director of Cleveland Clinic Adult Reconstruction Research. “It’s not a trend or marketing tool. It’s a new approach and surgical tool that allows us to do a high volume of procedures with both precision and efficient, reliable delivery.”
Cleveland Clinic’s number of total joint replacements completed with robotic support is among the highest in the U.S., he says. But, with the big volume comes big responsibility.
“We are using our volumes and experience to help develop evidence-based practices for robot-assisted surgery that benefit not only Cleveland Clinic and its patients, but the whole field,” says Dr. Piuzzi. “We are constantly studying and publishing ways to increase value by improving patient outcomes and optimizing costs — improving the entire episode of care.”
By 2025, one in four total hip arthroplasties in the U.S. will be done robotically, according to a Cleveland Clinic study. By 2030, the number is predicted to be two in three, and one in two total knee arthroplasties.
For many hip and knee surgeons at Cleveland Clinic, the ratio is already higher. Dr. Piuzzi estimates that he uses robot assistance in 90% of his total knee arthroplasties (TKAs) and 30%-40% of his total hip arthroplasties (THAs).
In this Q&A, Cleveland Clinic orthopaedic surgeons share what they’ve learned on the way to tallying 10,000 robot-assisted total joint replacements.
Dr. Piuzzi: The robot allows me to integrate many more variables into the execution of a procedure, such as how to perform a cut. Instead of thinking two dimensionally, the robot helps me think three dimensionally, for added accuracy. Before I make any cuts, I know how I’m going to balance the knee and where I’m going to position the components. That helps me do fewer resections and soft-tissue releases for a less invasive surgery.
Advertisement
John McLaughlin, DO: I was reluctant to use robotics at first because I did not think there would be a significant benefit and that it would add too much time. I have been pleasantly surprised that my robotic surgeries have been time neutral. Robotics allows for fine-tuning of implant position, which could lead to better outcomes and lower revision rates. I feel that my patients experience less pain after robotic surgery, allowing for faster recovery.
Michael Bloomfield, MD: With robotic surgery, I now havedata to enhance preoperative planning and intraoperative decision-making regarding knee balancing in TKA and hip/spine considerations in THA.
Peter Surace, MD: Outliers have been nearly eliminated thanks to robotic surgery. Issues with implant position, stability and balancing are addressed so accurately that the end of these cases is always satisfying. In the total hip world, stability, leg length and cup position are improved with robotic assistance. In the knee world, limb alignment and ligamentous tension and balancing are improved compared to manual applications.
Matthew Deren, MD: The robot provides an added level of confidence in the operating room, even for trainees. Important structures are protected that could otherwise be damaged by the saw blade. And, if you correctly tension the knee’s ligaments, you can balance the knee replacement with small adjustments for extreme precision. I believe this ultimately results in a faster recovery for patients.
Dr. McLaughlin: I have had many cases in which I have used the robot to place implants in the setting of retained hardware, whether plates, screws or intramedullary nails.
Advertisement
Dr. Bloomfield: I performed robot-assisted TKA on a young woman with severely deficient distal femoral bone stock.
Dr. Surace: We have pushed the use of robotics to improve even the most complex cases, including patients with massive acetabular bone loss, previous operations, antibiotic spacers and even previous joint replacements. The improved fidelity of component position helps us remove less existing hardware, improve revision implant position and be more efficient.
Kim L. Stearns, MD: I was one of the early adopters of robotic surgery at Cleveland Clinic back in 2017 and worked on one of our first studies. I use robotic platforms for my most challenging cases, including for patients with severe deformities or contractures. Although patients are requesting robotic surgery more and more, I think it’s important to still be able to do a knee manually. Remember that robotic platforms are tools to assist the surgeon. They shouldn’t take the place of understanding how and why steps are taken to perform a surgery.
Dr. Piuzzi: You don’t need to apply robotic technology to every case. Some patients may benefit from having manual surgery, while others who have retained hardware or a deformity might benefit from the precision and augmentation of research that you get from robot- and computer-assisted surgery. When you’re learning, take time to see how more experienced centers are doing robotic surgery. It’s a different operating room setup and a different skill set for the entire surgical team, not just the surgeon.
Advertisement
Trevor Murray, MD: Be patient. Just like anything else, starting something new will have its ups and downs. Fortunately, the learning curve for robotic surgery is not steep. Schedule fewer cases the day you use robotics for the first time.
Dr. Bloomfield: There are a lot of educational resources and training available from robotic platform manufacturers. Take advantage of these to make your transition easier. For the hip, good exposure around the rim of the acetabulum makes registration easier.
Dr. Surace: There is a learning curve, but it affects time of operation, not the accuracy or efficacy of the surgery. Once you get used to cutting, reaming or registering with the robot, you can move through the case as efficiently as a manual hip or knee replacement.
Dr. Deren: Don’t be afraid to recheck things before you cut. In my workflow, we tension the ligaments, then model the planned resections, then check the ligaments again to ensure we don’t overcorrect a deformity prior to making cuts. I find this particularly helpful in knees where the deformity corrects to neutral before making any cuts.
Dr. Deren: Many think that robotic surgery takes longer. Actually, it’s time neutral. The difference is in the process. All the planning, adjusting and balancing is done up front. The robotic arm allows you to perfectly execute your plan, so you need to make your plan perfect. This is different from our manual procedures in which we make cuts and adjustments as we go.
Dr. Surace: One misconception is that we don’t need robotics because “joints have been doing great without it.” While it’s true that most total joints do great, there is a small number that don’t. Robotic platforms demonstrate improvement in hitting all anatomic positioning, balancing, leg length and stability targets — all things associated with improved patient outcomes. Performing robotic surgery does not imply that primary manual joints don’t do well. It’s an opportunity to improve accuracy and do more sophisticated planning to address the needs of those outlier cases.
Advertisement
Dr. Murray: I believe robotics will become almost ubiquitous within total joint surgery. I foresee improvements in understanding patient-specific details related to surgery and then robotics’ allowing us to execute those specific parameters intraoperatively.
Dr. Surace: I believe that robotic joint replacements will become more widespread in the next five to 10 years. The platforms are becoming more accurate and user friendly. I believe this will dramatically change the landscape for both primary and revision joints.
Dr. Deren: Revisions will be the next frontier for robotic assistance, which is very exciting. This will change the level of accuracy and precision in which we perform revision knees and hips, ultimately simplifying the procedures and improving outcomes.
Advertisement
Join us in Cleveland July 17 for a practical, first-of-kind course
As robotics in the OR grows, so does the role of nurses
Study finds that fracture and infection are rare
Recognition could help guide health policy, workforce development and resource allocation worldwide
With a better understanding of timelines and contributing factors, clinicians can help athletes undergoing TKAs set realistic expectations
A physician's perspective on confirmation imaging, diagnostic confidence and choosing the right robotic platform for patients
Increasing precision to conserve bone and protect soft tissue
How it’s similar but different from the direct anterior approach