New findings have clinical implications for myelomeningocele management
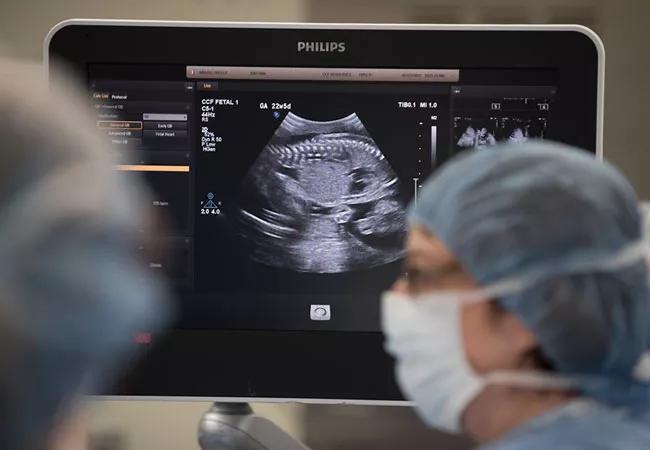
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/f2e69921-9c28-4eca-881b-37ab865ebf0c/19-OBG-1458-spinalBifidaImaging-650x450_jpg)
19-OBG-1458-spinalBifidaImaging-650×450
Magnetic resonance imaging (MRI) does not enhance long-term fetal or pediatric outcomes in cases of myelomeningocele (MMC), according to a new study. The findings are from a large retrospective analysis of patients referred to Cleveland Clinic’s Fetal Care Center, a collaborative team of highly skilled and compassionate healthcare professionals who offer state-of-the-art techniques and interventions with a family-centered approach.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
Also known as open spina bifida, MMC is the most common central nervous system congenital defect, occurring in approximately 1,645 births annually in the United States. It is characterized by incomplete neural tube closure and a fluid-filled sac containing an exposed, extruded segment of spinal cord and nerves.
MMC usually is diagnosed in the mid-second trimester, on routine anatomy ultrasounds (US), and the level of the defect in the spine is characterized with MRI, according to study co-author Katherine Singh, MD, maternal fetal medicine specialist at the Fetal Care Center.
“The fetuses were suspected to have myelomeningocele, based on routine anatomy ultrasounds,” Dr. Singh says. “We wanted to see how accurate MRI was as compared to an ultrasound or postnatal exam and whether MRI changed management or improved any outcomes in the babies we followed.”
The new analysis showed that MRI is not superior to US for diagnosis of MMC. An assessment of complete perinatal and pediatric outcomes up to age 12 years also found that pregnancies complicated by MMC did not vary in morbidity, and pediatric outcomes remained similar regardless of lesion level.
“We have a fairly large number of babies that are referred to us or who we follow for antenatal diagnosis of myelomeningocele,” says Dr. Singh. “In our population, MRI was not superior in qualifying or diagnosing a myelomeningocele in the pregnancies we followed. There was no significant agreement between diagnosis on physical exam and the imaging diagnosis.”
Advertisement
The cohort for the retrospective study, published in September 2019 in the Journal of Perinatal Medicine, included 49 patients with an antenatal diagnosis, of whom 20 decided to terminate pregnancy and two pursued fetal surgery. The objective was to directly compare antenatal US and MRI for diagnosis and localization of MMC and postnatal outcomes in the infants.
All of the patients were followed up at the MMC clinic, which includes neurosurgery, neurology, urology, orthopedics and pediatrics, and is part of Cleveland Clinic Children’s Fetal Care Center. The comprehensive analysis spanned antenatal diagnosis through pregnancy, delivery, postpartum and pediatric phases.
The researchers found that overall, spinal cord level correlation between US and MRI was very poor. When compared to physical exams performed by neonatologists and neurosurgeons, no direct correlation was statistically significant. (P-value kappas for physical exam, US and MRI, physical exam and US, and physical exam and MRI were 0.00, 0.01 and 0.02, respectively.) Says Dr. Singh, “Whatever diagnostic modality we used, we were often wrong in guessing where the lesion was.”
Sacral lesions—which were incidentally noted to occur earlier in pregnancy—were the only maternal or pregnancy characteristics other than time of diagnosis of MMC that were significant. Gestational age was significantly lower in the fetuses with sacral lesions (P < 0.05). Birth weight was found to be lower in infants with sacral lesions (3197.4 g vs 2645 g for lumbosacral and 3457.1 g for lumbar lesions; P = 0.005), but that was confounded by the 25-week delivery of a fetus due to preterm labor.
Advertisement
“The secondary outcomes we looked at were pediatric, to determine whether they differed based on final diagnosis at the level of the lesion,” says Dr. Singh. “We perform antenatal repair on many fetuses with myelomeningocele and they were not included in this study population.”
Follow-up during the pediatric period ranged from 2 to 144 months and was done by trained specialists in each field at Cleveland Clinic’s MMC clinic. Consistent with reports in other studies, the authors found that 26 of 29 patients developed neurogenic bladders, notably irrespective of the level of their spinal cord lesions. Given that all fetuses had ventriculomegaly at time of US, the authors believe the etiology of neurogenic bladder in these patients may be multifactorial.
“Until this year, minimal clinical information has been available in the literature on whether MRI is necessary for myelomeningocele diagnosis,” Dr. Singh says. “Our study shows that it is probably not needed, at least with the current resolution of fetal MRI.” One avenue of potential research is looking at ways to improve the accuracy of MRI for diagnosis.
“Another thing that might be helpful is to develop standard antenatal and pediatric outcomes to better assess pregnancies with myelomeningocele,” Dr. Singh says. “That is an area of active research at Cleveland Clinic’s Fetal Care Center.”
Taken together, the data in the new report show that MRI does not provide any additional value in enhancing pregnancy or fetal outcomes associated with MMC. The imaging is a requirement for planning fetal surgery but not for pregnancy outcomes. The results, Dr. Singh says, add to the literature and may provide physicians with information to help guide patients through an MMC diagnosis while optimizing healthcare resources and patient care.
Advertisement
Advertisement
Despite safety concerns and mixed trial results, experts see potential for this indication
Experts endorse a push to improve prevention and treatment following repetitive head injury
A population with very high lifetime risk presents care challenges and pathophysiologic insights
Two Cleveland Clinic neurologists review biomarker advances, targeted therapies and unresolved clinical challenges
Data-driven segmentation approach shows promise for seizure characterization with utility for clinical decision making
Alzheimer’s studies delve into preventing and modifying the disease’s trajectory and impact
Study finds broadly similar outcomes between MIS and open surgical approaches
System uses clinical data routinely collected at clinical visits