Minimizing patient discomfort, improving quality of life
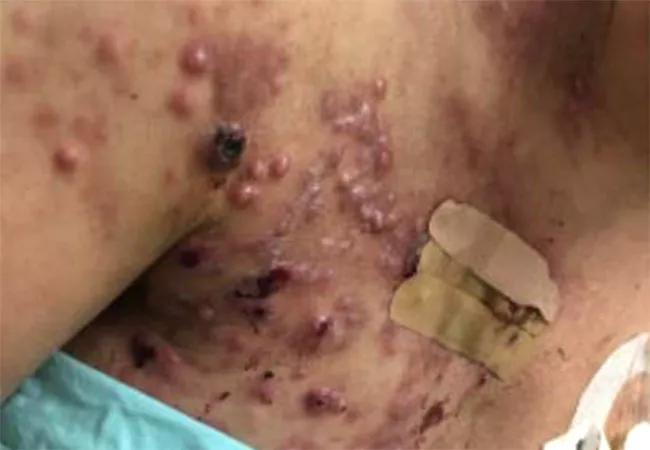
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/36d0e4ef-a5ca-4649-8c63-b358bcb8c9c7/650x450-Breast-Cancer-Skin-Reoccurances_jpg)
650×450-Breast-Cancer-Skin-Reoccurances
Thanks to advances in screening and treatments, patients with breast cancer are living longer. As a result, diffuse cutaneous metastases are becoming more common, and these skin lesions can severely impact patient quality of life. Cleveland Clinic Cancer Center’s Department of Radiation Oncology has developed techniques that minimize patient discomfort and improve quality of life using streamlined intensity-modulated radiation therapy (IMRT).
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“There’s a common myth that once a patient has been treated with radiation for breast cancer, they cannot be treated again, or that the area of skin metastases is too large to treat,” says Chirag Shah, MD, Director of Breast Radiation Oncology at Cleveland Clinic Cancer Center. “We absolutely can use radiation on large, diffuse skin metastases while sparing the heart and lung, which is really important because these cases are not commonly treated with surgical interventions.”
Conventional techniques, such as 3-dimension conformal radiation therapy and electron fields, are difficult to set up and cannot spare normal tissues as well in the re-irradiation setting. With IMRT, patients can receive high doses of radiation that avoid normal tissues and are effective in re-irradiation. Some centers use this approach for diffuse cutaneous metastases, but no published guidelines or preferred methodologies exist.
A recent report published in The Breast Journal offers a methodology that improved quality of life for several patients and is preferred by Cleveland Clinic clinicians for patients presenting with such clinical indications. The report discusses five patients who initially had locally advanced, nonmetastatic breast cancer and a median time to metastatic recurrence of 17 months. Four of five patients had been treated with postmastectomy radiation therapy (PMRT).
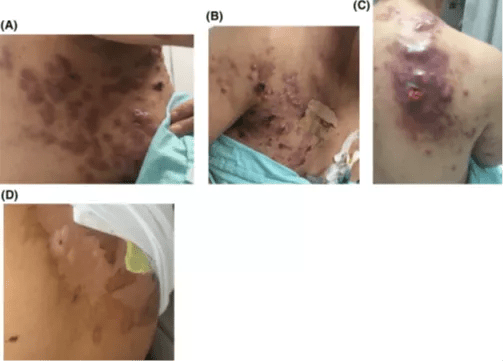
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/27ab7a72-9110-4732-a2b8-8673e8bdc34a/shah-skin-mets-1_png)
Clinical presentation. (A) Right axilla (B) Chest wall (C) Posterior chest wall (D) Posterior chest wall one month after completion of 30 Gy in 10 fractions with near complete response. Figure and caption republished with permission from Wiley.
Advertisement
“Our preferred technique involves mapping areas of disease and then wiring 2 to 3 centimeters beyond that while placing bolus to enhance skin dose. Then we utilize the treatment planning system to turn the wires into a volume to be treated. The patients are lying down, and this takes about an hour,” says Dr. Shah, senior author of the paper.
A dosimetrist working with a computer algorithm turns the map into preliminary radiation targets, which clinicians review and adjust to ensure accuracy. The dosimetrist in conjunction with the algorithm then develops an IMRT plan that spares normal tissue. Patients with metastatic disease and previous RT commonly receive a range of doses from 30 to 66 Gy/10 to 33 fractions.
Of the five patients in the report, four patients experienced a complete or near complete response at three months. Two had received concurrent hyperthermia during IMRT. All experienced grade 3 dermatitis.
“These patients can be very ill, and of the five we treated, three have since passed away,” says Dr. Shah. “But our efforts to alleviate their pain and improve their quality of life by reducing their burden of cutaneous metastases are an important part of what we do here. Patients with severe cancer recurrences can have improved quality of life with the proper planning and techniques.”
Advertisement
Advertisement
Reframing cancer survivorship
New guidelines empower clinicians with practical diagnostic framework
Pivotal Studies Guide Treatment Decisions in Muscle-Invasive Bladder Cancer
Reflections from an oncology provider and communications educator on new ASCO Guidelines on Patient-Clinician Communication
Phase 1 trial outcomes offer encouraging news for developing targeted therapy for solid tumors
Cleveland Clinic to administer first-of-its-kind T-cell therapy
Heavily pretreated patients experience improved progression-free survival and quality of life with CD20xCD3 therapy
Innovative procedure reduces scarring, recovery time and nipple sensation