A maternal-fetal medicine specialist discusses home births, restricted visitation and efforts to ensure patient safety
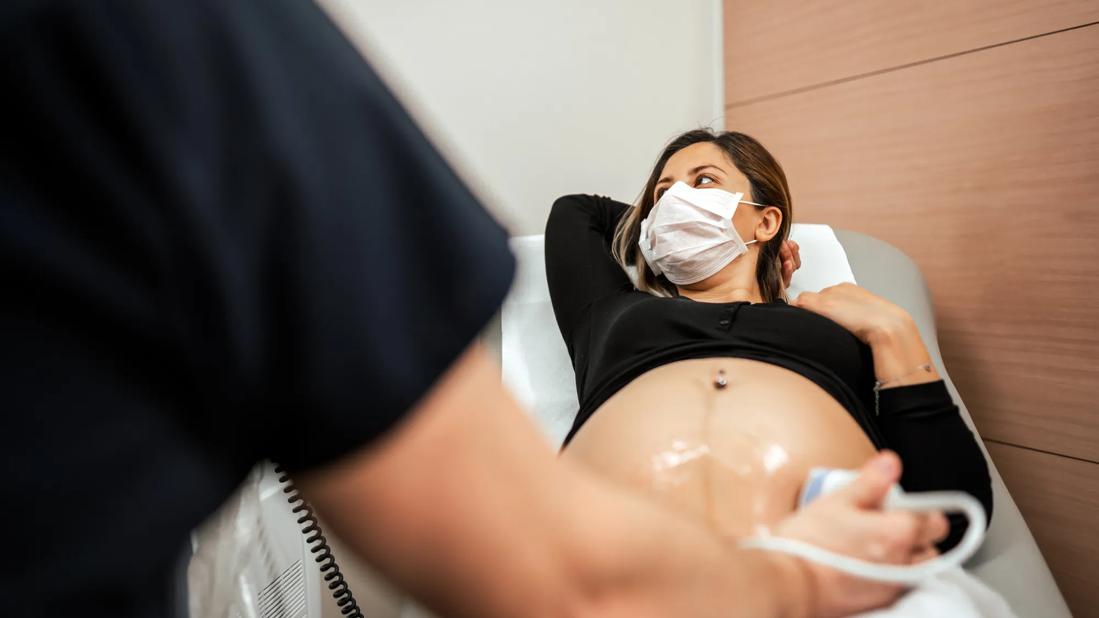
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/3df08a11-cc69-4e8f-a9f4-ef411cdba0d6/pregnancy-ultrasound-covid-1309595023)
Pregnant woman receiving ultrasound
Pregnancy, labor and delivery are already emotionally charged experiences, and as pregnant women face increased uncertainty amid the COVID-19 pandemic, many worry that their birth plans may no longer be possible for a variety of reasons. Inquiries into home births have increased significantly. To help physicians address these patient concerns, Consult QD sat down with maternal-fetal medicine specialist Edward Chien, MD, MBA, Chair of the Department of Obstetrics and Gynecology in Cleveland Clinic’s Ob/Gyn & Women’s Health Institute.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
As restrictions are placed on visitation in hospitals around the nation, many pregnant women are worried that they will have to go through labor and delivery alone, without the support of their birth partner. What advice should physicians give these patients?
Dr. Chien: Across the city of Cleveland — at Cleveland Clinic Fairview and Hillcrest Hospitals, Cleveland Clinic Akron General, University Hospitals, Cleveland and MetroHealth Medical Center — one support person is permitted to attend labor and delivery. The only caveat is that if the partner has COVID-19 or other symptoms associated with COVID-19 infection, then they would not be allowed to attend. We recommend that pregnant women identify a backup support person in case their intended support person becomes symptomatic. Additionally, we recommend that the support person remain with the mother throughout the course until discharge, if at all possible, to help support social distancing and reduce the risk of bringing an infection into the hospital unknowingly.
There appears to be an increased interest in home births. What does the literature say about the risks and benefits of home births compared with hospital births?
Dr. Chien: In the United States, about 0.9% of births take place in the home, and it’s important that women are presented with the potential risks and benefits related to this choice. There’s a twofold higher risk for perinatal death for home birth compared with a hospital birth. We also know from the literature that there’s a threefold increase in risk for either neonatal seizure or a serious neurological dysfunction in home births versus hospital-based birth. The risk for postpartum hemorrhage is fairly similar across both groups, but hospitals are better equipped to manage those emergencies. So those are some of the known risks related to home versus hospital birth.
Advertisement
The other is, that patients may not be aware of, is that — at least in Ohio — lay midwives or home birth attendants are unregulated. If a patient is considering a home birth, it’s important that they seek a certified nurse midwife with a clearly defined transfer arrangement or agreement with a provider.
Do you anticipate a shortage of beds or staff in our maternity wards? Do you think anticipate that beds will be taken for COVID-19 care?
Dr. Chien: I believe labor and delivery is a unique environment and I would expect that most institutions will not change how this space is used. At the current time, at least in Cleveland, we aren’t anticipating a shortage of staff or beds in labor and delivery. We have reassigned one of our overflow postpartum units, which is only used around 12% of the year.
I have seen some reports that several hospital systems across the country are establishing separate labor and delivery units for patients positive with COVID-19. Do we have any plans like that at Cleveland Clinic?
Dr. Chien: At Cleveland Clinic, we haven’t designated one hospital for labor and delivery for COVID-19 positive patients, but we have allocated specific locations for them within both labor and delivery and postpartum to provide more isolation and less traffic around those rooms.
I read that there’s a hospital in Minnesota that is inducing labor at 39 weeks to try to get families in and out before the COVID-19 peak. What are your thoughts about that practice?
Dr. Chien: I suggest that they use current recommendations for timing of delivery. We know that inductions of labor use more hospital resources just because the length of stay is longer. But it’s not an unreasonable strategy to reduce the risk of cesarean section because there is data, at least for first pregnancies, that the risk of cesarean section is lower with active management at 39 weeks as compared with waiting for spontaneous labor to start.
Advertisement
Has Cleveland Clinic adjusted its discharge timing at all to try to reduce resource use? Are you sending women home earlier?
Dr. Chien: We are encouraging discharge when the new mother and baby are medically stable. We also have support services for breastfeeding that can be obtained as an outpatient. At Cleveland Clinic, we have made adjustments to continue to provide those services amid the COVID-19 pandemic. We stopped group support services when the COVID-19 outbreak began, but still offer one-on-one individual and virtual visits for breastfeeding moms who need additional support.
How else might we minimize risk for women delivering in the hospital?
Dr. Chien: At least in the Cleveland area, and our neighboring counties, we are preparing for the COVID-19 surge and have plans in place to provide a safe environment for our mothers. As physicians, we should encourage our patients to express their concerns and ask their questions so that we can reassure them that we are providing a safe environment for labor. Other preventive measures at Cleveland Clinic include rapid testing available for symptomatic patients in labor, and virtual visits for prenatal care. We offer cloth face masks to patients to reduce the risk of spreading infection, and we strongly recommend patients follow the social distancing recommendations.
Advertisement
Advertisement
Patients report improved sense of smell and taste
Clinicians who are accustomed to uncertainty can do well by patients
Unique skin changes can occur after infection or vaccine
Cleveland Clinic analysis suggests that obtaining care for the virus might reveal a previously undiagnosed condition
As the pandemic evolves, rheumatologists must continue to be mindful of most vulnerable patients
Early results suggest positive outcomes from COVID-19 PrEP treatment
Could the virus have caused the condition or triggered previously undiagnosed disease?
Five categories of cutaneous abnormalities are associated with COVID-19