Helps reduce risk of premature menopause
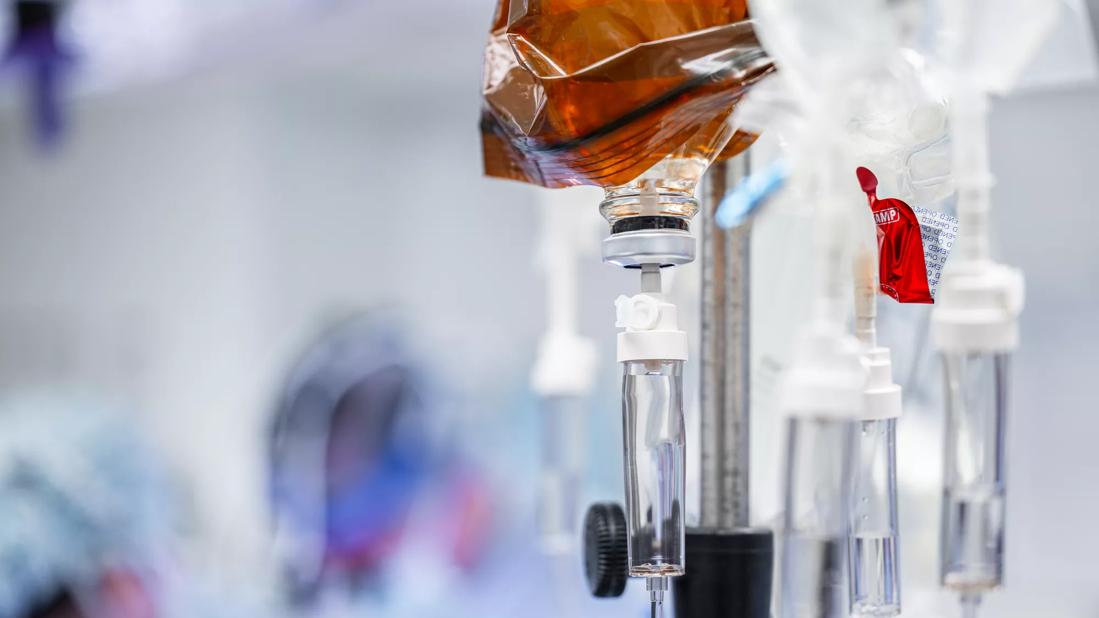
Image content: This image is available to view online.
View image online (https://assets.clevelandclinic.org/transform/0f5b7f67-5a7c-48d6-92f4-fb9cd777f4ab/REG_4720221_03-19-24_047_SCG)
Chemotherapy
Women undergoing chemotherapy for breast cancer and other malignancies face a serious risk of experiencing ovarian toxicity which can lead to premature menopause. This complication is especially concerning to patients of child-bearing age who wish to preserve their fertility. In addition, menopause is associated with symptoms that may adversely affect quality of life.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
“It’s a particular issue for breast cancer patients,” says Halle Moore, MD, staff in the Department of Solid Tumor Oncology. “We’re a little reluctant to give hormone replacement therapy to them — which would ordinarily help with premature menopausal symptoms — even if they don’t have hormone-sensitive breast cancer.”
In 2015, Dr. Moore and colleagues published in New England Journal of Medicine the results of the Prevention of Early Menopause Study (POEMS), a phase 3 clinical trial developed to assess whether ovarian failure could be prevented by temporarily suppressing ovarian function by including goserelin, a gonadotropin hormone-releasing hormone (GNRH) agonist, with standard chemotherapy. “We showed that goserelin use reduced the risk of ovarian failure by about 70 percent in our population,” Dr. Moore says.
Now, Dr. Moore has five-year follow-up results that continue to show that patients who receive both goserelin and chemotherapy are more likely have successful pregnancies and perhaps even live longer than those who don’t. She recently presented her data at the 2017 San Antonio Breast Cancer Symposium.
The POEMS study randomized 218 eligible female breast cancer patients whose cancers were estrogen-receptor and progesterone-receptor-negative to receive either cyclophosphamide-containing chemotherapy alone or with goserelin added.
Dr. Moore and her colleagues found that among 135 participants for whom ovarian function was assessable at two years, only 8 percent of those receiving the goserelin-supplemented treatment experienced ovarian failure, compared to 22 percent of the women who did not (OR = 0.30, P = 0.03).
Advertisement
“Goserelin shuts down ovarian cycling during chemotherapy. It puts the patients into essentially a temporary menopause during treatment, but in the long run it improves their chances of not developing premature menopause.”
With a median follow-up of 5.1 years, Dr. Moore and her colleagues found that 22 percent of patients in the goserelin group had at least one pregnancy compared with 12 percent in the standard group (OR 2.38; 95% CI, 1.08-5.26; P = 0.03).
They also found that disease free survival estimates were 88 percent in the goserelin arm compared with 79 percent in the standard arm (HR = 0.50, P = 0.05) and five-year overall survival was 92 percent with goserelin versus 83 percent in the standard arm (HR = 0.47, P = 0.06).
“With long-term follow-up, our data continue to show that women were significantly more likely to become pregnant if they used the goserelin,” Dr. Moore says, “and that they were more likely to be alive and free of their cancer.”
Dr. Moore says some organizations such as the National Comprehensive Cancer Network (NCCN) have included in its guidelines the use of goserelin for prevention of early menopause in women with ER negative breast cancer. However, she says the American Society of Clinical Oncology (ASCO) has not.
“It’s important to raise awareness of this relatively simple intervention to reduce the risk of ovarian failure with chemotherapy for breast cancer,” Dr. Moore says. “It should absolutely be included in the ASCO fertility guidelines.”
Advertisement
She adds, “Ovarian protection with GnRH agonist during chemotherapy is safe and effective. Not only does this intervention improve the prospects for fertility, but it also should reduce the other potential consequences of early menopause including osteoporosis, hot flashes, vaginal dryness and other distressing effects of early menopause.”
Advertisement
Advertisement
New guidelines empower clinicians with practical diagnostic framework
Pivotal Studies Guide Treatment Decisions in Muscle-Invasive Bladder Cancer
Reflections from an oncology provider and communications educator on new ASCO Guidelines on Patient-Clinician Communication
Phase 1 trial outcomes offer encouraging news for developing targeted therapy for solid tumors
Cleveland Clinic to administer first-of-its-kind T-cell therapy
Heavily pretreated patients experience improved progression-free survival and quality of life with CD20xCD3 therapy
Innovative procedure reduces scarring, recovery time and nipple sensation
Best practices for supporting patients with honesty and compassion