Lupus can cause a broad spectrum of clinical presentations. In this video, Emily Littlejohn, DO, MPH, shares an atypical presentation of systemic lupus erythematosus, illustrating the need for a keen eye when evaluating patients. Dr. Littlejohn is staff in the Orthopaedic and Rheumatologic Institute and Co-Director of the Lupus Clinic.
Advertisement
Cleveland Clinic is a non-profit academic medical center. Advertising on our site helps support our mission. We do not endorse non-Cleveland Clinic products or services. Policy
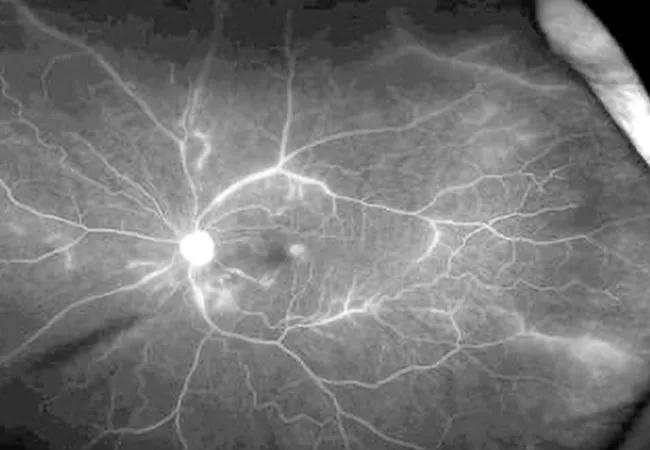
A 28-year-old healthy female presented with vision changes. Basic blood work revealed a low white blood cell count, which prompted a referral to hematology and a bone marrow biopsy. When the biopsy proved normal, she was sent to rheumatology, where bloodwork revealed a positive antinuclear antibody (ANA) screen, positive anti-Smith antibodies, low C4 and a positive lupus anticoagulant. Given the patient’s ongoing blurry vision, she was referred to ophthalmology, where she was diagnosed with retinal vasculitis. Her exam showed severe vascular sheathing and attenuation, cotton wool spots and scattered dot and blot hemorrhages of both eyes. Optical coherence tomography (OCT) showed atrophy and ellipsoid zone (EZ) loss without edema. Fluorescein angiography showed extensive nonperfusion in the macula with leakage as well as peripheral nonperfusion.
She was then hospitalized for further workup, which included a lumbar puncture, thorough infectious workup and magnetic resonance imaging (MRI) of her brain, which showed inflammatory leptomeningeal and white matter changes in the occipital lobe. Watch the video below to learn about her treatment.
Video content: This video is available to watch online.
View video online (https://www.youtube.com/embed/UM4Rn01AOFc?feature=oembed)
Lupus: Why We Need a Keen Eye
The right therapy for lupus retinal vasculitis can be sight- or lifesaving. Lupus retinal vasculitis may lead to significant vision loss if left untreated, and can be an indicator of underlying systemic disease, including lupus cerebral vasculitis. This is rare but can lead to cerebral infarction. It is crucial to differentiate lupus retinal vasculitis from standard vascular occlusion syndromes. Inflammatory causes of the vision symptoms this patient experienced may include lupus, giant cell arteritis, granulomatosis with polyangiitis, polyarteritis nodosa, inflammatory bowel disease, sarcoidosis and multiple sclerosis.
Advertisement
Advertisement

Motion-tracking Brillouin microscopy pinpoints corneal weakness in the anterior stroma

Registry data highlight visual gains in patients with legal blindness

Prescribing eye drops is complicated by unknown risk of fetotoxicity and lack of clinical evidence

A look at emerging technology shaping retina surgery

A primer on MIGS methods and devices

7 keys to success for comprehensive ophthalmologists

Study is first to show reduction in autoimmune disease with the common diabetes and obesity drugs

Treatment options range from tetracycline injections to fat repositioning and cheek lift